Oral Cavity and Nasopharyngeal Cancers Screening (PDQ®)–Patient Version
What Is Screening?
Screening is looking for cancer before a person has any symptoms. This can help find cancer at an early stage. When abnormal tissue or cancer is found early, it may be easier to treat. By the time symptoms appear, cancer may have begun to spread.
Scientists are trying to better understand which people are more likely to get certain types of cancer. They also study the things we do and the things around us to see if they cause cancer. This information helps doctors recommend who should be screened for cancer, which screening tests should be used, and how often the tests should be done.
It is important to remember that your doctor does not necessarily think you have cancer if he or she suggests a screening test. Screening tests are given when you have no cancer symptoms.
If a screening test result is abnormal, you may need to have more tests done to find out if you have cancer. These are called diagnostic tests.
General Information About Oral Cavity and Nasopharyngeal Cancers
Key Points
- Oral cavity and nasopharyngeal cancers are diseases in which malignant (cancer) cells form in the mouth and throat.
- The number of new cases of oral cavity and nasopharyngeal cancers and the number of deaths from these cancers vary by sex and geographic region.
- Different factors increase or decrease the risk of oral cavity and nasopharyngeal cancers.
Oral cavity and nasopharyngeal cancers are diseases in which malignant (cancer) cells form in the mouth and throat.
Oral cavity cancer usually forms in the squamous cells (thin, flat cells lining the inside of the oral cavity).
Oral cavity cancer forms in any of these tissues of the oral cavity:
- the lips
- the front two thirds of the tongue
- the gingiva (gums)
- the buccal mucosa (the lining of the inside of the cheeks)
- the floor (bottom) of the mouth under the tongue
- the hard palate (the front of the roof of the mouth)
- the retromolar trigone (the small area behind the wisdom teeth)

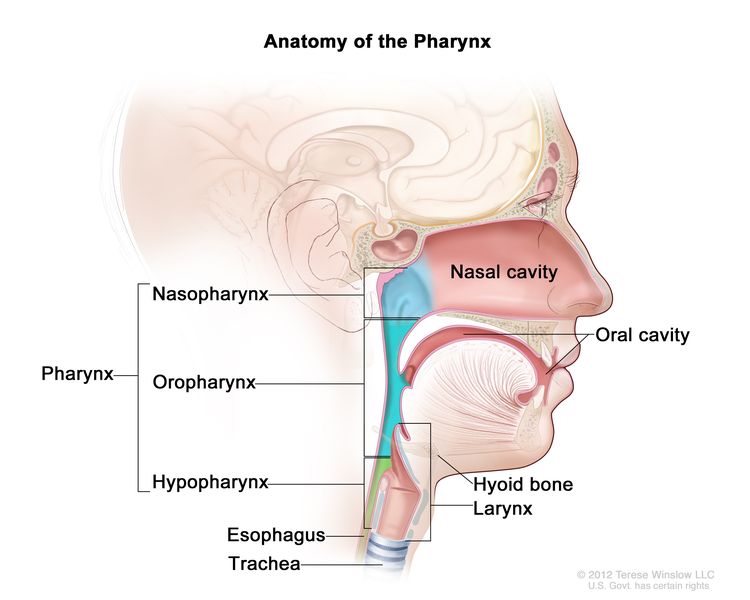
Pharyngeal cancer forms in the tissues of the pharynx (throat), including the nasopharynx, oropharynx, and hypopharynx. This summary covers nasopharyngeal cancer, which forms in the tissue of the nasopharynx (the upper part of the throat behind the nose).
Other PDQ summaries containing information related to oral cavity and nasopharyngeal cancers include:
The number of new cases of oral cavity and nasopharyngeal cancers and the number of deaths from these cancers vary by sex and geographic region.
From 2012 to 2021, the number of new cases of oral cavity cancer in the United States increased slightly each year.
Oral cavity cancer is more common in men than in women. Although oral cavity cancer may occur in adults of any age, it occurs most often in those aged 75 to 84 years.
France, Brazil, and parts of Asia have much higher rates of oral cavity cancer than most other countries.
Nasopharyngeal cancer is rare in the United States. Some indigenous populations in Southeast Asia, the Arctic, North Africa, and the Middle East have higher rates of nasopharyngeal cancers.
Different factors increase or decrease the risk of oral cavity and nasopharyngeal cancers.
Anything that increases your chance of getting a disease is called a risk factor. Anything that decreases your chance of getting a disease is called a protective factor.
Being infected with Epstein-Barr virus (EBV) increases the risk of nasopharyngeal cancer.
Other PDQ summaries containing information related to oral cavity and nasopharyngeal cancers include:
Oral Cavity and Nasopharyngeal Cancers Screening
Key Points
- Tests are used to screen for different types of cancer when a person does not have symptoms.
- There are no standard or routine screening tests for oral cavity and nasopharyngeal cancers.
- Screening tests for oral cavity and nasopharyngeal cancers are being studied in clinical trials.
Tests are used to screen for different types of cancer when a person does not have symptoms.
Scientists study screening tests to find those with the fewest harms and most benefits. Cancer screening trials also are meant to show whether early detection (finding cancer before it causes symptoms) helps a person live longer or decreases a person's chance of dying from the disease. For some types of cancer, the chance of recovery is better if the disease is found and treated at an early stage.
There are no standard or routine screening tests for oral cavity and nasopharyngeal cancers.
No studies have shown that screening for oral cavity cancer and nasopharyngeal cancer would lower the risk of dying from these diseases.
A dentist or medical doctor may check the oral cavity during a routine check-up. The exam will include looking for lesions, including areas of leukoplakia (an abnormal white patch of cells) and erythroplakia (an abnormal red patch of cells). Leukoplakia and erythroplakia lesions on the mucous membranes may become cancerous.
If lesions are seen in the mouth, the following procedures may be used to find abnormal tissue that might become oral cavity cancer:
- Toluidine blue stain: A procedure in which lesions in the mouth are coated with a blue dye. Areas that stain darker are more likely to be cancer or become cancer.
- Fluorescence staining: A procedure in which lesions in the mouth are viewed using a special light. After the patient uses a fluorescent mouth rinse, normal tissue looks different from abnormal tissue when seen under the light.
- Exfoliative cytology: A procedure to collect cells from the oral cavity. A piece of cotton, a brush, or a small wooden stick is used to gently scrape cells from the lips, tongue, or mouth. The cells are viewed under a microscope to find out if they are abnormal.
- Brush biopsy: The removal of cells using a brush that is designed to collect cells from all layers of a lesion. The cells are viewed under a microscope to find out if they are abnormal.
More than half of oral cancers have already spread to lymph nodes or other areas by the time they are found.
Epstein-Barr virus (EBV) has been linked to nasopharyngeal cancer. Screening for nasopharyngeal cancer using the EBV antibody test or EBV DNA test has been studied. These are laboratory tests used to check the blood for EBV antibodies or EBV DNA. If EBV antibodies or DNA are found in the blood, more tests may be done to check for nasopharyngeal cancer. No studies have shown that screening would decrease the risk of dying from this disease.
Screening tests for oral cavity and nasopharyngeal cancers are being studied in clinical trials.
Information about clinical trials supported by NCI can be found on NCI’s clinical trials search webpage. Clinical trials supported by other organizations can be found on the ClinicalTrials.gov website.
Risks of Oral Cavity and Nasopharyngeal Cancers Screening
Key Points
- Screening tests have risks.
- The risks of screening for oral cavity and nasopharyngeal cancers include:
- Finding these cancers may not improve health or help a person live longer.
- False-negative test results can occur.
- False-positive test results can occur.
Screening tests have risks.
Decisions about screening tests can be difficult. Not all screening tests are helpful and most have risks. Before having any screening test, you may want to discuss the test with your doctor. It is important to know the risks of the test and whether it has been proven to reduce the risk of dying from cancer.
The risks of screening for oral cavity and nasopharyngeal cancers include:
Finding these cancers may not improve health or help a person live longer.
Some cancers never cause symptoms or become life-threatening, but if found by a screening test, the cancer may be treated. Finding these cancers is called overdiagnosis. It is not known if treatment of oral cavity cancer or nasopharyngeal cancer would help you live longer than if no treatment were given, and treatments for cancer, such as surgery and radiation therapy, may have serious side effects.
False-negative test results can occur.
Screening test results may appear to be normal even though oral cavity cancer or nasopharyngeal cancer is present. A person who receives a false-negative test result (one that shows there is no cancer when there really is) may delay seeking medical care even if there are symptoms.
False-positive test results can occur.
Screening test results may appear to be abnormal even though no cancer is present. A false-positive test result (one that shows there is cancer when there really isn't) can cause anxiety and is usually followed by more tests and procedures (such as biopsy), which also have risks.
About This PDQ Summary
About PDQ
Physician Data Query (PDQ) is the National Cancer Institute's (NCI's) comprehensive cancer information database. The PDQ database contains summaries of the latest published information on cancer prevention, detection, genetics, treatment, supportive care, and complementary and alternative medicine. Most summaries come in two versions. The health professional versions have detailed information written in technical language. The patient versions are written in easy-to-understand, nontechnical language. Both versions have cancer information that is accurate and up to date and most versions are also available in Spanish.
PDQ is a service of the NCI. The NCI is part of the National Institutes of Health (NIH). NIH is the federal government’s center of biomedical research. The PDQ summaries are based on an independent review of the medical literature. They are not policy statements of the NCI or the NIH.
Purpose of This Summary
This PDQ cancer information summary has current information about oral cavity and nasopharyngeal cancers screening. It is meant to inform and help patients, families, and caregivers. It does not give formal guidelines or recommendations for making decisions about health care.
Reviewers and Updates
Editorial Boards write the PDQ cancer information summaries and keep them up to date. These Boards are made up of experts in cancer treatment and other specialties related to cancer. The summaries are reviewed regularly and changes are made when there is new information. The date on each summary ("Updated") is the date of the most recent change.
The information in this patient summary was taken from the health professional version, which is reviewed regularly and updated as needed, by the PDQ Screening and Prevention Editorial Board.
Clinical Trial Information
A clinical trial is a study to answer a scientific question, such as whether one treatment is better than another. Trials are based on past studies and what has been learned in the laboratory. Each trial answers certain scientific questions in order to find new and better ways to help cancer patients. During treatment clinical trials, information is collected about the effects of a new treatment and how well it works. If a clinical trial shows that a new treatment is better than one currently being used, the new treatment may become "standard." Patients may want to think about taking part in a clinical trial. Some clinical trials are open only to patients who have not started treatment.
Clinical trials can be found online at NCI's website. For more information, call the Cancer Information Service (CIS), NCI's contact center, at 1-800-4-CANCER (1-800-422-6237).
Permission to Use This Summary
PDQ is a registered trademark. The content of PDQ documents can be used freely as text. It cannot be identified as an NCI PDQ cancer information summary unless the whole summary is shown and it is updated regularly. However, a user would be allowed to write a sentence such as “NCI’s PDQ cancer information summary about breast cancer prevention states the risks in the following way: [include excerpt from the summary].”
The best way to cite this PDQ summary is:
PDQ® Screening and Prevention Editorial Board. PDQ Oral Cavity and Nasopharyngeal Cancers Screening. Bethesda, MD: National Cancer Institute. Updated <MM/DD/YYYY>. Available at: https://www.cancer.gov/types/head-and-neck/patient/oral-screening-pdq. Accessed <MM/DD/YYYY>. [PMID: 26389441]
Images in this summary are used with permission of the author(s), artist, and/or publisher for use in the PDQ summaries only. If you want to use an image from a PDQ summary and you are not using the whole summary, you must get permission from the owner. It cannot be given by the National Cancer Institute. Information about using the images in this summary, along with many other images related to cancer can be found in Visuals Online. Visuals Online is a collection of more than 3,000 scientific images.
Disclaimer
The information in these summaries should not be used to make decisions about insurance reimbursement. More information on insurance coverage is available on Cancer.gov on the Managing Cancer Care page.
Contact Us
More information about contacting us or receiving help with the Cancer.gov website can be found on our Contact Us for Help page. Questions can also be submitted to Cancer.gov through the website’s E-mail Us.