Pancreatic Neuroendocrine Tumors (Islet Cell Tumors) Treatment (PDQ®)–Patient Version
General Information About Pancreatic Neuroendocrine Tumors (Islet Cell Tumors)
Key Points
- Pancreatic neuroendocrine tumors form in hormone-making cells (islet cells) of the pancreas.
- Pancreatic NETs may or may not cause signs or symptoms.
- There are different kinds of functional pancreatic NETs.
- Having certain syndromes can increase the risk of pancreatic NETs.
- Different types of pancreatic NETs have different signs and symptoms.
- Lab tests and imaging tests are used to diagnose pancreatic NETs.
- Other kinds of lab tests are used to check for the specific type of pancreatic NETs.
- Certain factors affect prognosis (chance of recovery) and treatment options.
Pancreatic neuroendocrine tumors form in hormone-making cells (islet cells) of the pancreas.
The pancreas is a gland about 6 inches long that is shaped like a thin pear lying on its side. The wider end of the pancreas is called the head, the middle section is called the body, and the narrow end is called the tail. The pancreas lies behind the stomach and in front of the spine. 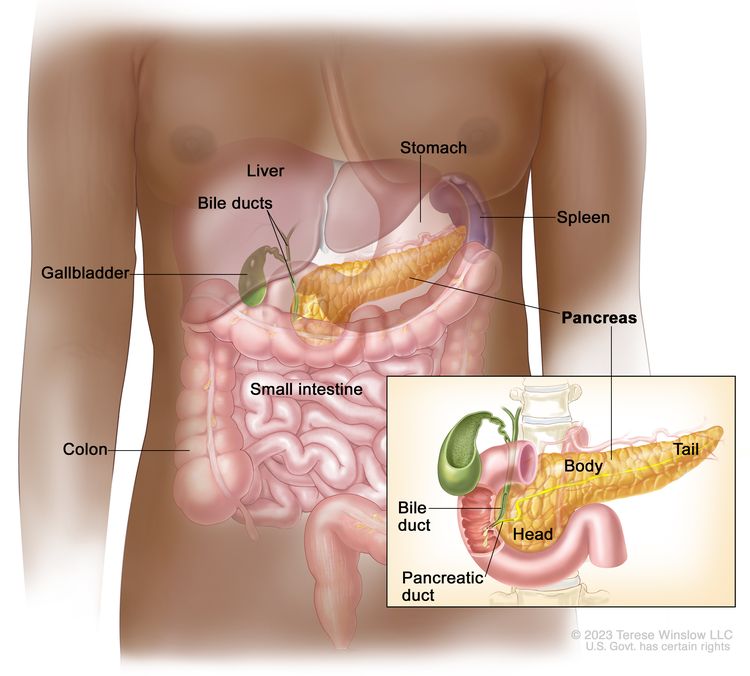
There are two kinds of cells in the pancreas:
- Endocrine pancreas cells make several kinds of hormones (chemicals that control the actions of certain cells or organs in the body), such as insulin to control blood sugar. They cluster together in many small groups (islets) throughout the pancreas. Endocrine pancreas cells are also called islet cells or islets of Langerhans. Tumors that form in islet cells are called islet cell tumors, pancreatic endocrine tumors, or pancreatic neuroendocrine tumors (pancreatic NETs).
- Exocrine pancreas cells make enzymes that are released into the small intestine to help the body digest food. Most of the pancreas is made of ducts with small sacs at the end of the ducts, which are lined with exocrine cells.
This summary discusses islet cell tumors of the endocrine pancreas. See the PDQ summary on Pancreatic Cancer Treatment for information on exocrine pancreatic cancer.
Pancreatic neuroendocrine tumors (NETs) may be benign (not cancer) or malignant (cancer). When pancreatic NETs are malignant, they are called pancreatic endocrine cancer or islet cell carcinoma.
Pancreatic NETs are much less common than pancreatic exocrine tumors and have a better prognosis.
Pancreatic NETs may or may not cause signs or symptoms.
Pancreatic NETs may be functional or nonfunctional:
Most pancreatic NETs are functional tumors.
There are different kinds of functional pancreatic NETs.
Pancreatic NETs make different kinds of hormones such as gastrin, insulin, and glucagon. Functional pancreatic NETs include the following:
- Gastrinoma: A tumor that forms in cells that make gastrin. Gastrin is a hormone that causes the stomach to release an acid that helps digest food. Both gastrin and stomach acid are increased by gastrinomas. When increased stomach acid, stomach ulcers, and diarrhea are caused by a tumor that makes gastrin, it is called Zollinger-Ellison syndrome. A gastrinoma usually forms in the head of the pancreas and sometimes forms in the small intestine. Most gastrinomas are malignant (cancer).
- Insulinoma: A tumor that forms in cells that make insulin. Insulin is a hormone that controls the amount of glucose (sugar) in the blood. It moves glucose into the cells, where it can be used by the body for energy. Insulinomas are usually slow-growing tumors that rarely spread. An insulinoma forms in the head, body, or tail of the pancreas. Insulinomas are usually benign (not cancer).
- Glucagonoma: A tumor that forms in cells that make glucagon. Glucagon is a hormone that increases the amount of glucose in the blood. It causes the liver to break down glycogen. Too much glucagon causes hyperglycemia (high blood sugar). A glucagonoma usually forms in the tail of the pancreas. Most glucagonomas are malignant (cancer).
- Other types of tumors: There are other rare types of functional pancreatic NETs that make hormones, including hormones that control the balance of sugar, salt, and water in the body. These tumors include: These other types of tumors are grouped together because they are treated in much the same way.
- VIPomas, which make vasoactive intestinal peptide. VIPoma may also be called Verner-Morrison syndrome.
- Somatostatinomas, which make somatostatin.
Having certain syndromes can increase the risk of pancreatic NETs.
Anything that increases your risk of getting a disease is called a risk factor. Having a risk factor does not mean that you will get cancer; not having risk factors doesn't mean that you will not get cancer. Talk with your doctor if you think you may be at risk.
Multiple endocrine neoplasia type 1 (MEN1) syndrome is a risk factor for pancreatic NETs.
Different types of pancreatic NETs have different signs and symptoms.
Signs or symptoms can be caused by the growth of the tumor and/or by hormones the tumor makes or by other conditions. Some tumors may not cause signs or symptoms. Check with your doctor if you have any of these problems.
Signs and symptoms of a non-functional pancreatic NET
A non-functional pancreatic NET may grow for a long time without causing signs or symptoms. It may grow large or spread to other parts of the body before it causes signs or symptoms, such as:
- Diarrhea.
- Indigestion.
- A lump in the abdomen.
- Pain in the abdomen or back.
- Yellowing of the skin and whites of the eyes.
Signs and symptoms of a functional pancreatic NET
The signs and symptoms of a functional pancreatic NET depend on the type of hormone being made.
Too much gastrin may cause:
- Stomach ulcers that keep coming back.
- Pain in the abdomen, which may spread to the back. The pain may come and go and it may go away after taking an antacid.
- The flow of stomach contents back into the esophagus (gastroesophageal reflux).
- Diarrhea.
Too much insulin may cause:
- Low blood sugar. This can cause blurred vision, headache, and feeling lightheaded, tired, weak, shaky, nervous, irritable, sweaty, confused, or hungry.
- Fast heartbeat.
Too much glucagon may cause:
- Skin rash on the face, stomach, or legs.
- High blood sugar. This can cause headaches, frequent urination, dry skin and mouth, or feeling hungry, thirsty, tired, or weak.
- Blood clots. Blood clots in the lung can cause shortness of breath, cough, or pain in the chest. Blood clots in the arm or leg can cause pain, swelling, warmth, or redness of the arm or leg.
- Diarrhea.
- Weight loss for no known reason.
- Sore tongue or sores at the corners of the mouth.
Too much vasoactive intestinal peptide (VIP) may cause:
- Very large amounts of watery diarrhea.
- Dehydration. This can cause feeling thirsty, making less urine, dry skin and mouth, headaches, dizziness, or feeling tired.
- Low potassium level in the blood. This can cause muscle weakness, aching, or cramps, numbness and tingling, frequent urination, fast heartbeat, and feeling confused or thirsty.
- Cramps or pain in the abdomen.
- Weight loss for no known reason.
Too much somatostatin may cause:
- High blood sugar. This can cause headaches, frequent urination, dry skin and mouth, or feeling hungry, thirsty, tired, or weak.
- Diarrhea.
- Steatorrhea (very foul-smelling stool that floats).
- Gallstones.
- Yellowing of the skin and whites of the eyes.
- Weight loss for no known reason.
A pancreatic NET may also make too much adrenocorticotropic hormone (ACTH) and cause Cushing syndrome. Signs and symptoms of Cushing syndrome include the following:
- Headache.
- Some loss of vision.
- Weight gain in the face, neck, and trunk of the body, and thin arms and legs.
- A lump of fat on the back of the neck.
- Thin skin that may have purple or pink stretch marks on the chest or abdomen.
- Easy bruising.
- Growth of fine hair on the face, upper back, or arms.
- Bones that break easily.
- Sores or cuts that heal slowly.
- Anxiety, irritability, and depression.
The treatment of pancreatic NETs that make too much ACTH and Cushing syndrome are not discussed in this summary.
Lab tests and imaging tests are used to diagnose pancreatic NETs.
The following tests and procedures may be used:
- Physical exam and health history: An exam of the body to check general signs of health, including checking for signs of disease, such as lumps or anything else that seems unusual. A history of the patient’s health habits and past illnesses and treatments will also be taken.
- Blood chemistry studies: A procedure in which a blood sample is checked to measure the amounts of certain substances, such as glucose (sugar), released into the blood by organs and tissues in the body. An unusual (higher or lower than normal) amount of a substance can be a sign of disease.
- Chromogranin A test: A test in which a blood sample is checked to measure the amount of chromogranin A in the blood. A higher than normal amount of chromogranin A and normal amounts of hormones such as gastrin, insulin, and glucagon can be a sign of a non-functional pancreatic NET.
- Abdominal CT scan (CAT scan): A procedure that makes a series of detailed pictures of the abdomen, taken from different angles. The pictures are made by a computer linked to an x-ray machine. A dye may be injected into a vein or swallowed to help the organs or tissues show up more clearly. This procedure is also called computed tomography, computerized tomography, or computerized axial tomography.
- MRI (magnetic resonance imaging): A procedure that uses a magnet, radio waves, and a computer to make a series of detailed pictures of areas inside the body. This procedure is also called nuclear magnetic resonance imaging (NMRI).
- Somatostatin receptor scintigraphy: A type of radionuclide scan that may be used to find small pancreatic NETs. A small amount of radioactive octreotide (a hormone that attaches to tumors) is injected into a vein and travels through the blood. The radioactive octreotide attaches to the tumor and a special camera that detects radioactivity is used to show where the tumors are in the body. This procedure is also called octreotide scan and SRS.
- Endoscopic ultrasound (EUS): A procedure in which an endoscope is inserted into the body, usually through the mouth or rectum. An endoscope is a thin, tube-like instrument with a light and a lens for viewing. A probe at the end of the endoscope is used to bounce high-energy sound waves (ultrasound) off internal tissues or organs and make echoes. The echoes form a picture of body tissues called a sonogram. This procedure is also called endosonography.
- Endoscopic retrograde cholangiopancreatography (ERCP): A procedure used to x-ray the ducts (tubes) that carry bile from the liver to the gallbladder and from the gallbladder to the small intestine. Sometimes pancreatic cancer causes these ducts to narrow and block or slow the flow of bile, causing jaundice. An endoscope is passed through the mouth, esophagus, and stomach into the first part of the small intestine. An endoscope is a thin, tube-like instrument with a light and a lens for viewing. A catheter (a smaller tube) is then inserted through the endoscope into the pancreatic ducts. A dye is injected through the catheter into the ducts and an x-ray is taken. If the ducts are blocked by a tumor, a fine tube may be inserted into the duct to unblock it. This tube (or stent) may be left in place to keep the duct open. Tissue samples may also be taken and checked under a microscope for signs of cancer.
- Angiogram: A procedure to look at blood vessels and the flow of blood. A contrast dye is injected into the blood vessel. As the contrast dye moves through the blood vessel, x-rays are taken to see if there are any blockages.
- Laparotomy: A surgical procedure in which an incision (cut) is made in the wall of the abdomen to check the inside of the abdomen for signs of disease. The size of the incision depends on the reason the laparotomy is being done. Sometimes organs are removed or tissue samples are taken and checked under a microscope for signs of disease.
- Intraoperative ultrasound: A procedure that uses high-energy sound waves (ultrasound) to create images of internal organs or tissues during surgery. A transducer placed directly on the organ or tissue is used to make the sound waves, which create echoes. The transducer receives the echoes and sends them to a computer, which uses the echoes to make pictures called sonograms.
- Biopsy: The removal of cells or tissues so they can be viewed under a microscope by a pathologist to check for signs of cancer. There are several ways to do a biopsy for pancreatic NETs. Cells may be removed using a fine or wide needle inserted into the pancreas during an x-ray or ultrasound. Tissue may also be removed during a laparoscopy (a surgical incision made in the wall of the abdomen).
- Bone scan: A procedure to check if there are rapidly dividing cells, such as cancer cells, in the bone. A very small amount of radioactive material is injected into a vein and travels through the bloodstream. The radioactive material collects in bones with cancer and is detected by a scanner.
Other kinds of lab tests are used to check for the specific type of pancreatic NETs.
The following tests and procedures may be used:
Gastrinoma
- Fasting serum gastrin test: A test in which a blood sample is checked to measure the amount of gastrin in the blood. This test is done after the patient has had nothing to eat or drink for at least 8 hours. Conditions other than gastrinoma can cause an increase in the amount of gastrin in the blood.
- Basal acid output test: A test to measure the amount of acid made by the stomach. The test is done after the patient has had nothing to eat or drink for at least 8 hours. A tube is inserted through the nose or throat, into the stomach. The stomach contents are removed and four samples of gastric acid are removed through the tube. These samples are used to find out the amount of gastric acid made during the test and the pH level of the gastric secretions.
- Secretin stimulation test: If the basal acid output test result is not normal, a secretin stimulation test may be done. The tube is moved into the small intestine and samples are taken from the small intestine after a drug called secretin is injected. Secretin causes the small intestine to make acid. When there is a gastrinoma, the secretin causes an increase in how much gastric acid is made and the level of gastrin in the blood.
- Somatostatin receptor scintigraphy: A type of radionuclide scan that may be used to find small pancreatic NETs. A small amount of radioactive octreotide (a hormone that attaches to tumors) is injected into a vein and travels through the blood. The radioactive octreotide attaches to the tumor and a special camera that detects radioactivity is used to show where the tumors are in the body. This procedure is also called octreotide scan and SRS.
Insulinoma
- Fasting serum glucose and insulin test: A test in which a blood sample is checked to measure the amounts of glucose (sugar) and insulin in the blood. The test is done after the patient has had nothing to eat or drink for at least 24 hours.
Glucagonoma
- Fasting serum glucagon test: A test in which a blood sample is checked to measure the amount of glucagon in the blood. The test is done after the patient has had nothing to eat or drink for at least 8 hours.
Other tumor types
- VIPoma
- Serum VIP (vasoactive intestinal peptide) test: A test in which a blood sample is checked to measure the amount of VIP.
- Blood chemistry studies: A procedure in which a blood sample is checked to measure the amounts of certain substances released into the blood by organs and tissues in the body. An unusual (higher or lower than normal) amount of a substance can be a sign of disease. In VIPoma, there is a lower than normal amount of potassium.
- Stool analysis: A stool sample is checked for a higher than normal sodium (salt) and potassium levels.
- Somatostatinoma
- Fasting serum somatostatin test: A test in which a blood sample is checked to measure the amount of somatostatin in the blood. The test is done after the patient has had nothing to eat or drink for at least 8 hours.
- Somatostatin receptor scintigraphy: A type of radionuclide scan that may be used to find small pancreatic NETs. A small amount of radioactive octreotide (a hormone that attaches to tumors) is injected into a vein and travels through the blood. The radioactive octreotide attaches to the tumor and a special camera that detects radioactivity is used to show where the tumors are in the body. This procedure is also called octreotide scan and SRS.
Certain factors affect prognosis (chance of recovery) and treatment options.
Pancreatic NETs can often be cured. The prognosis and treatment options depend on the following:
- The type of cancer cell.
- Where the tumor is found in the pancreas.
- Whether the tumor has spread to more than one place in the pancreas or to other parts of the body.
- Whether the patient has MEN1 syndrome.
- The patient's age and general health.
- Whether the cancer has just been diagnosed or has recurred (come back).
Stages of Pancreatic Neuroendocrine Tumors
Key Points
- The plan for cancer treatment depends on where the NET is found in the pancreas and whether it has spread.
- There are three ways that cancer spreads in the body.
- Cancer may spread from where it began to other parts of the body.
- Pancreatic NETs can recur (come back) after they have been treated.
The plan for cancer treatment depends on where the NET is found in the pancreas and whether it has spread.
The process used to find out if cancer has spread within the pancreas or to other parts of the body is called staging. The results of the tests and procedures used to diagnose pancreatic neuroendocrine tumors (NETs) are also used to find out whether the cancer has spread. See the General Information section for a description of these tests and procedures.
Although there is a standard staging system for pancreatic NETs, it is not used to plan treatment. Treatment of pancreatic NETs is based on the following:
- Whether the cancer is found in one place in the pancreas.
- Whether the cancer is found in several places in the pancreas.
- Whether the cancer has spread to lymph nodes near the pancreas or to other parts of the body such as the liver, lung, peritoneum, or bone.
There are three ways that cancer spreads in the body.
Cancer can spread through tissue, the lymph system, and the blood:
- Tissue. The cancer spreads from where it began by growing into nearby areas.
- Lymph system. The cancer spreads from where it began by getting into the lymph system. The cancer travels through the lymph vessels to other parts of the body.
- Blood. The cancer spreads from where it began by getting into the blood. The cancer travels through the blood vessels to other parts of the body.
Cancer may spread from where it began to other parts of the body.
When cancer spreads to another part of the body, it is called metastasis. Cancer cells break away from where they began (the primary tumor) and travel through the lymph system or blood.
- Lymph system. The cancer gets into the lymph system, travels through the lymph vessels, and forms a tumor (metastatic tumor) in another part of the body.
- Blood. The cancer gets into the blood, travels through the blood vessels, and forms a tumor (metastatic tumor) in another part of the body.
The metastatic tumor is the same type of tumor as the primary tumor. For example, if a pancreatic neuroendocrine tumor spreads to the liver, the tumor cells in the liver are actually neuroendocrine tumor cells. The disease is metastatic pancreatic neuroendocrine tumor, not liver cancer.
Pancreatic NETs can recur (come back) after they have been treated.
The tumors may come back in the pancreas or in other parts of the body.
Treatment Option Overview
Key Points
- There are different types of treatment for patients with pancreatic NETs.
- The following types of treatment are used:
- Surgery
- Chemotherapy
- Hormone therapy
- Hepatic arterial occlusion or chemoembolization
- Targeted therapy
- Supportive care
- New types of treatment are being tested in clinical trials.
- Treatment for pancreatic neuroendocrine tumors may cause side effects.
- Patients may want to think about taking part in a clinical trial.
- Patients can enter clinical trials before, during, or after starting their cancer treatment.
- Follow-up tests may be needed.
There are different types of treatment for patients with pancreatic NETs.
Different types of treatments are available for patients with pancreatic neuroendocrine tumors (NETs). Some treatments are standard (the currently used treatment), and some are being tested in clinical trials. A treatment clinical trial is a research study meant to help improve current treatments or obtain information on new treatments for patients with cancer. When clinical trials show that a new treatment is better than the standard treatment, the new treatment may become the standard treatment. Patients may want to think about taking part in a clinical trial. Some clinical trials are open only to patients who have not started treatment.
The following types of treatment are used:
Surgery
An operation may be done to remove the tumor. One of the following types of surgery may be used:
- Enucleation: Surgery to remove the tumor only. This may be done when cancer occurs in one place in the pancreas.
- Pancreatoduodenectomy: A surgical procedure in which the head of the pancreas, the gallbladder, nearby lymph nodes and part of the stomach, small intestine, and bile duct are removed. Enough of the pancreas is left to make digestive juices and insulin. The organs removed during this procedure depend on the patient's condition. This is also called the Whipple procedure.
- Distal pancreatectomy: Surgery to remove the body and tail of the pancreas. The spleen may also be removed if cancer has spread to the spleen.
- Total gastrectomy: Surgery to remove the whole stomach.
- Parietal cell vagotomy: Surgery to cut the nerve that causes stomach cells to make acid.
- Liver resection: Surgery to remove part or all of the liver.
- Radiofrequency ablation: The use of a special probe with tiny electrodes that kill cancer cells. Sometimes the probe is inserted directly through the skin and only local anesthesia is needed. In other cases, the probe is inserted through an incision in the abdomen. This is done in the hospital with general anesthesia.
- Cryosurgical ablation: A procedure in which tissue is frozen to destroy abnormal cells. This is usually done with a special instrument that contains liquid nitrogen or liquid carbon dioxide. The instrument may be used during surgery or laparoscopy or inserted through the skin. This procedure is also called cryoablation.
Chemotherapy
Chemotherapy is a cancer treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. When chemotherapy is taken by mouth or injected into a vein or muscle, the drugs enter the bloodstream and can reach cancer cells throughout the body (systemic chemotherapy). When chemotherapy is placed directly into the cerebrospinal fluid, an organ, or a body cavity such as the abdomen, the drugs mainly affect cancer cells in those areas (regional chemotherapy). Combination chemotherapy is the use of more than one anticancer drug. The way the chemotherapy is given depends on the type of the cancer being treated.
Hormone therapy
Hormone therapy is a cancer treatment that removes hormones or blocks their action and stops cancer cells from growing. Hormones are substances made by glands in the body and circulated in the bloodstream. Some hormones can cause certain cancers to grow. If tests show that the cancer cells have places where hormones can attach (receptors), drugs, surgery, or radiation therapy is used to reduce the production of hormones or block them from working.
Hepatic arterial occlusion or chemoembolization
Hepatic arterial occlusion uses drugs, small particles, or other agents to block or reduce the flow of blood to the liver through the hepatic artery (the major blood vessel that carries blood to the liver). This is done to kill cancer cells growing in the liver. The tumor is prevented from getting the oxygen and nutrients it needs to grow. The liver continues to receive blood from the hepatic portal vein, which carries blood from the stomach and intestine.
Chemotherapy delivered during hepatic arterial occlusion is called chemoembolization. The anticancer drug is injected into the hepatic artery through a catheter (thin tube). The drug is mixed with the substance that blocks the artery and cuts off blood flow to the tumor. Most of the anticancer drug is trapped near the tumor and only a small amount of the drug reaches other parts of the body.
The blockage may be temporary or permanent, depending on the substance used to block the artery.
Targeted therapy
Targeted therapy is a type of treatment that uses drugs or other substances to identify and attack specific cancer cells. Targeted therapies usually cause less harm to normal cells than chemotherapy or radiation therapy do. Certain types of targeted therapies are being studied in the treatment of pancreatic NETs.
Supportive care
Supportive care is given to lessen the problems caused by the disease or its treatment. Supportive care for pancreatic NETs may include treatment for the following:
- Stomach ulcers may be treated with drug therapy such as:
- Proton pump inhibitor drugs such as omeprazole, lansoprazole, or pantoprazole.
- Histamine blocking drugs such as cimetidine, ranitidine, or famotidine.
- Somatostatin-type drugs such as octreotide.
- Diarrhea may be treated with:
- Intravenous (IV) fluids with electrolytes such as potassium or chloride.
- Somatostatin-type drugs such as octreotide.
- Low blood sugar may be treated by having small, frequent meals or with drug therapy to maintain a normal blood sugar level.
- High blood sugar may be treated with drugs taken by mouth or insulin by injection.
New types of treatment are being tested in clinical trials.
Information about clinical trials is available from the NCI website.
Treatment for pancreatic neuroendocrine tumors may cause side effects.
For information about side effects caused by treatment for cancer, visit our Side Effects page.
Patients may want to think about taking part in a clinical trial.
For some patients, taking part in a clinical trial may be the best treatment choice. Clinical trials are part of the cancer research process. Clinical trials are done to find out if new cancer treatments are safe and effective or better than the standard treatment.
Many of today's standard treatments for cancer are based on earlier clinical trials. Patients who take part in a clinical trial may receive the standard treatment or be among the first to receive a new treatment.
Patients who take part in clinical trials also help improve the way cancer will be treated in the future. Even when clinical trials do not lead to effective new treatments, they often answer important questions and help move research forward.
Patients can enter clinical trials before, during, or after starting their cancer treatment.
Some clinical trials only include patients who have not yet received treatment. Other trials test treatments for patients whose cancer has not gotten better. There are also clinical trials that test new ways to stop cancer from recurring (coming back) or reduce the side effects of cancer treatment.
Clinical trials are taking place in many parts of the country. Information about clinical trials supported by NCI can be found on NCI’s clinical trials search webpage. Clinical trials supported by other organizations can be found on the ClinicalTrials.gov website.
Follow-up tests may be needed.
As you go through treatment, you will have follow-up tests or check-ups. Some tests that were done to diagnose or stage the cancer may be repeated to see how well the treatment is working. Decisions about whether to continue, change, or stop treatment may be based on the results of these tests.
Some of the tests will continue to be done from time to time after treatment has ended. The results of these tests can show if your condition has changed or if the cancer has recurred (come back).
Treatment of Gastrinoma
For information about the treatments listed below, see the Treatment Option Overview section.
Treatment of gastrinoma may include supportive care and the following:
- For symptoms caused by too much stomach acid, treatment may be a drug that decreases the amount of acid made by the stomach.
- For a single tumor in the head of the pancreas:
- For a single tumor in the body or tail of the pancreas, treatment is usually surgery to remove the body or tail of the pancreas.
- For several tumors in the pancreas, treatment is usually surgery to remove the body or tail of the
pancreas. If tumor remains after surgery, treatment may include either:
- Surgery to cut the nerve that causes stomach cells to make acid and treatment with a drug that decreases stomach acid; or
- Surgery to remove the whole stomach (rare).
- For one or more tumors in the duodenum (the part of the small intestine that connects to the stomach), treatment is usually pancreatoduodenectomy (surgery to remove the head of the pancreas, the gallbladder, nearby lymph nodes and part of the stomach, small intestine, and bile duct).
- If no tumor is found, treatment may include the following:
- Surgery to cut the nerve that causes stomach cells to make acid and treatment with a drug that decreases stomach acid.
- Surgery to remove the whole stomach (rare).
- If the cancer has spread to the liver, treatment may include:
- Surgery to remove part or all of the liver.
- Radiofrequency ablation or cryosurgical ablation.
- Chemoembolization.
- If cancer has spread to other parts of the body or does not get better with surgery or drugs to decrease stomach acid, treatment may include:
- If the cancer mostly affects the liver and the patient has severe symptoms from hormones or from the size of tumor, treatment may include:
- Hepatic arterial occlusion, with or without systemic chemotherapy.
- Chemoembolization, with or without systemic chemotherapy.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Insulinoma
For information about the treatments listed below, see the Treatment Option Overview section.
Treatment of insulinoma may include the following:
- For one small tumor in the head or tail of the pancreas, treatment is usually surgery to remove the tumor.
- For one large tumor in the head of the pancreas that cannot be removed by surgery, treatment is usually pancreatoduodenectomy (surgery to remove the head of the pancreas, the gallbladder, nearby lymph nodes and part of the stomach, small intestine, and bile duct).
- For one large tumor in the body or tail of the pancreas, treatment is usually a distal pancreatectomy (surgery to remove the body and tail of the pancreas).
- For more than one tumor in the pancreas, treatment is usually surgery to remove any tumors in the head of the pancreas and the body and tail of the pancreas.
- For tumors that cannot be removed by surgery, treatment may include the following:
- Combination chemotherapy.
- Palliative drug therapy to decrease the amount of insulin made by the pancreas.
- Hormone therapy.
- Radiofrequency ablation or cryosurgical ablation.
- For cancer that has spread to lymph nodes or other parts of the body, treatment may include the following:
- Surgery to remove the cancer.
- Radiofrequency ablation or cryosurgical ablation, if the cancer cannot be removed by surgery.
- If the cancer mostly affects the liver and the patient has severe symptoms from hormones or from the size of tumor, treatment may include:
- Hepatic arterial occlusion, with or without systemic chemotherapy.
- Chemoembolization, with or without systemic chemotherapy.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Glucagonoma
For information about the treatments listed below, see the Treatment Option Overview section.
Treatment may include the following:
- For one small tumor in the head or tail of the pancreas, treatment is usually surgery to remove the tumor.
- For one large tumor in the head of the pancreas that cannot be removed by surgery, treatment is usually pancreatoduodenectomy (surgery to remove the head of the pancreas, the gallbladder, nearby lymph nodes and part of the stomach, small intestine, and bile duct).
- For more than one tumor in the pancreas, treatment is usually surgery to remove the tumor or surgery to remove the body and tail of the pancreas.
- For tumors that cannot be removed by surgery, treatment may include the following:
- For cancer that has spread to lymph nodes or other parts of the body, treatment may include the following:
- Surgery to remove the cancer.
- Radiofrequency ablation or cryosurgical ablation, if the cancer cannot be removed by surgery.
- If the cancer mostly affects the liver and the patient has severe symptoms from hormones or from the size of tumor, treatment may include:
- Hepatic arterial occlusion, with or without systemic chemotherapy.
- Chemoembolization, with or without systemic chemotherapy.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Other Pancreatic Neuroendocrine Tumors (Islet Cell Tumors)
For information about the treatments listed below, see the Treatment Option Overview section.
For VIPoma, treatment may include the following:
- Fluids and hormone therapy to replace fluids and electrolytes that have been lost from the body.
- Surgery to remove the tumor and nearby lymph nodes.
- Surgery to remove as much of the tumor as possible when the tumor cannot be completely removed or has spread to distant parts of the body. This is palliative therapy to relieve symptoms and improve the quality of life.
- For tumors that have spread to lymph nodes or other parts of the body, treatment may include the following:
- Surgery to remove the tumor.
- Radiofrequency ablation or cryosurgical ablation, if the tumor cannot be removed by surgery.
- For tumors that continue to grow during treatment or have spread to other parts of the body, treatment may include the following:
For somatostatinoma, treatment may include the following:
- Surgery to remove the tumor.
- For cancer that has spread to distant parts of the body, surgery to remove as much of the cancer as possible to relieve symptoms and improve quality of life.
- For tumors that continue to grow during treatment or have spread to other parts of the body, treatment may include the following:
- Chemotherapy.
- Targeted therapy.
Treatment of other types of pancreatic neuroendocrine tumors (NETs) may include the following:
- Surgery to remove the tumor.
- For cancer that has spread to distant parts of the body, surgery to remove as much of the cancer as possible or hormone therapy to relieve symptoms and improve quality of life.
- For tumors that continue to grow during treatment or have spread to other parts of the body, treatment may include the following:
- Chemotherapy.
- Targeted therapy.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Recurrent or Progressive Pancreatic Neuroendocrine Tumors
(Islet Cell Tumors)
For information about the treatments listed below, see the Treatment Option Overview section.
Treatment of pancreatic neuroendocrine tumors (NETs) that continue to grow during treatment or recur (come back) may include the following:
- Surgery to remove the tumor.
- Chemotherapy.
- Hormone therapy.
- Targeted therapy.
- For liver metastases:
- Regional chemotherapy.
- Hepatic arterial occlusion or chemoembolization, with or without systemic chemotherapy.
- A clinical trial of a new therapy.
To Learn More About Pancreatic Neuroendocrine Tumors (Islet Cell Tumors)
For more information from the National Cancer Institute about pancreatic neuroendocrine tumors (NETs), see the following:
For general cancer information and other resources from the National Cancer Institute, visit:
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
About This PDQ Summary
About PDQ
Physician Data Query (PDQ) is the National Cancer Institute's (NCI's) comprehensive cancer information database. The PDQ database contains summaries of the latest published information on cancer prevention, detection, genetics, treatment, supportive care, and complementary and alternative medicine. Most summaries come in two versions. The health professional versions have detailed information written in technical language. The patient versions are written in easy-to-understand, nontechnical language. Both versions have cancer information that is accurate and up to date and most versions are also available in Spanish.
PDQ is a service of the NCI. The NCI is part of the National Institutes of Health (NIH). NIH is the federal government’s center of biomedical research. The PDQ summaries are based on an independent review of the medical literature. They are not policy statements of the NCI or the NIH.
Purpose of This Summary
This PDQ cancer information summary has current information about the treatment of pancreatic neuroendocrine tumors (islet cell tumors). It is meant to inform and help patients, families, and caregivers. It does not give formal guidelines or recommendations for making decisions about health care.
Reviewers and Updates
Editorial Boards write the PDQ cancer information summaries and keep them up to date. These Boards are made up of experts in cancer treatment and other specialties related to cancer. The summaries are reviewed regularly and changes are made when there is new information. The date on each summary ("Updated") is the date of the most recent change.
The information in this patient summary was taken from the health professional version, which is reviewed regularly and updated as needed, by the PDQ Adult Treatment Editorial Board.
Clinical Trial Information
A clinical trial is a study to answer a scientific question, such as whether one treatment is better than another. Trials are based on past studies and what has been learned in the laboratory. Each trial answers certain scientific questions in order to find new and better ways to help cancer patients. During treatment clinical trials, information is collected about the effects of a new treatment and how well it works. If a clinical trial shows that a new treatment is better than one currently being used, the new treatment may become "standard." Patients may want to think about taking part in a clinical trial. Some clinical trials are open only to patients who have not started treatment.
Clinical trials can be found online at NCI's website. For more information, call the Cancer Information Service (CIS), NCI's contact center, at 1-800-4-CANCER (1-800-422-6237).
Permission to Use This Summary
PDQ is a registered trademark. The content of PDQ documents can be used freely as text. It cannot be identified as an NCI PDQ cancer information summary unless the whole summary is shown and it is updated regularly. However, a user would be allowed to write a sentence such as “NCI’s PDQ cancer information summary about breast cancer prevention states the risks in the following way: [include excerpt from the summary].”
The best way to cite this PDQ summary is:
PDQ® Adult Treatment Editorial Board. PDQ Pancreatic Neuroendocrine Tumors (Islet Cell Tumors) Treatment. Bethesda, MD: National Cancer Institute. Updated <MM/DD/YYYY>. Available at: https://www.cancer.gov/types/pancreatic/patient/pnet-treatment-pdq. Accessed <MM/DD/YYYY>. [PMID: 26389340]
Images in this summary are used with permission of the author(s), artist, and/or publisher for use in the PDQ summaries only. If you want to use an image from a PDQ summary and you are not using the whole summary, you must get permission from the owner. It cannot be given by the National Cancer Institute. Information about using the images in this summary, along with many other images related to cancer can be found in Visuals Online. Visuals Online is a collection of more than 3,000 scientific images.
Disclaimer
The information in these summaries should not be used to make decisions about insurance reimbursement. More information on insurance coverage is available on Cancer.gov on the Managing Cancer Care page.
Contact Us
More information about contacting us or receiving help with the Cancer.gov website can be found on our Contact Us for Help page. Questions can also be submitted to Cancer.gov through the website’s E-mail Us.