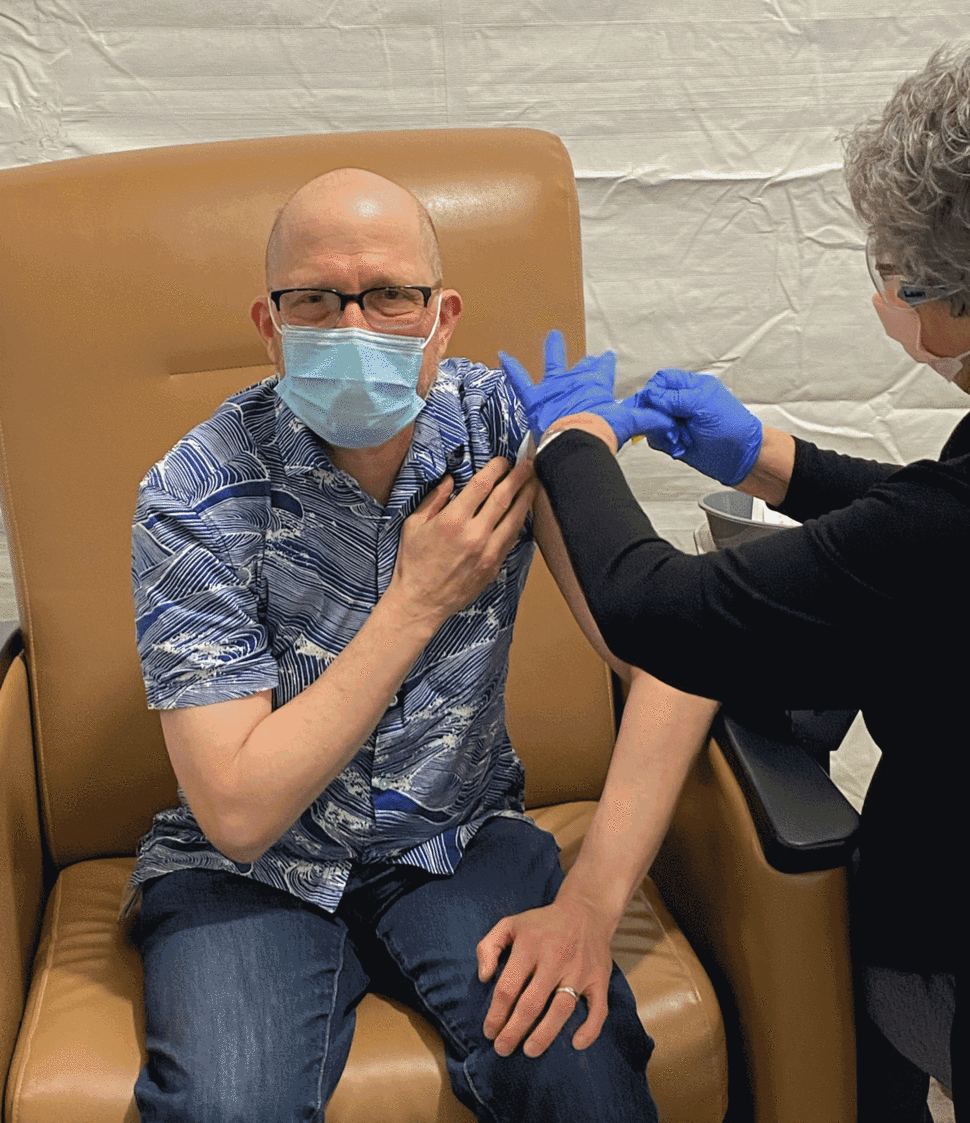
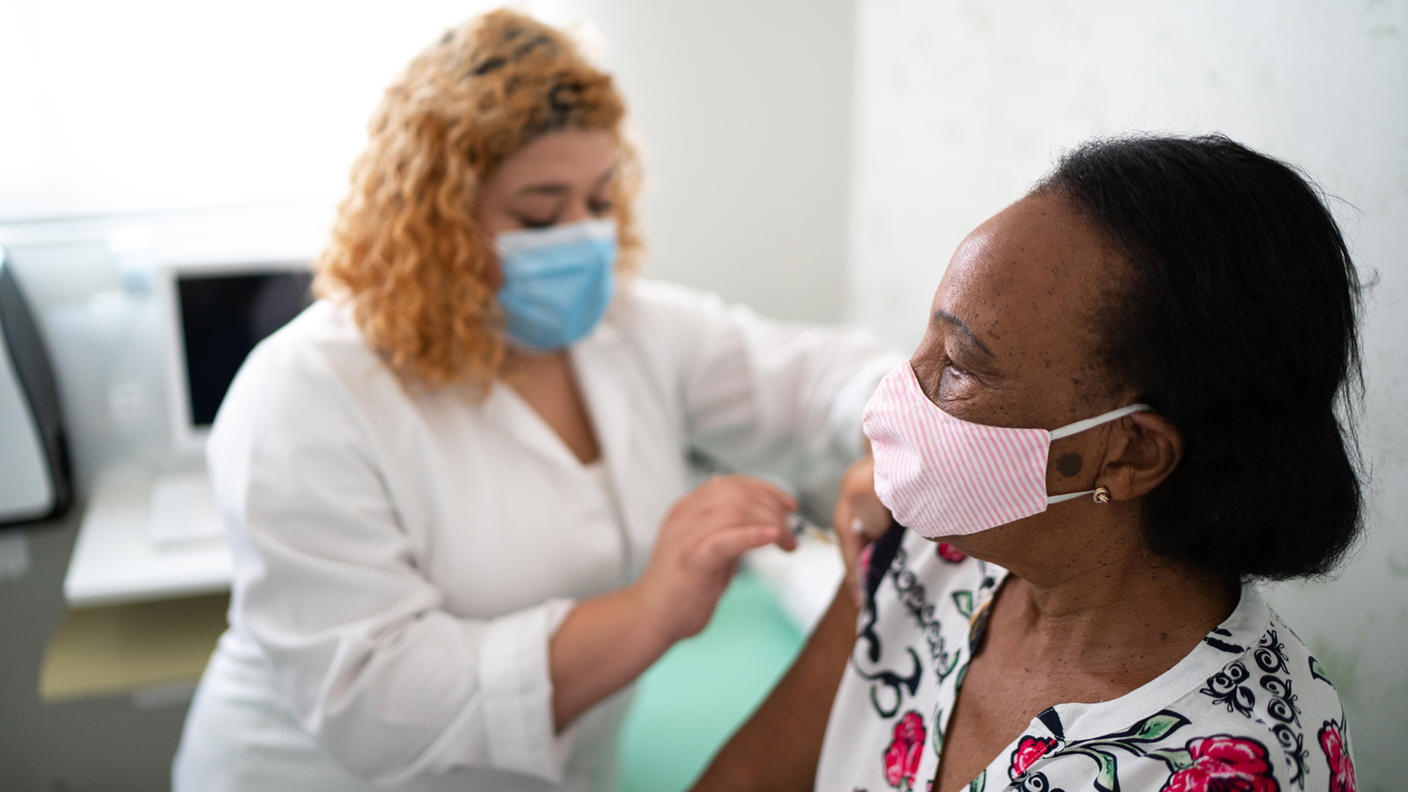
CDC, NCCN, and other cancer-related organizations urge cancer patients to get COVID-19 vaccinations and booster shots. Why?
Data show that people with cancer and others with weakened immune systems are at high risk for severe complications from COVID-19. Vaccines have been shown to decrease the risk of hospitalization and death from COVID-19, even among people with cancer. Plus, we have evidence that the virus can persist in immunocompromised people, which may lead to the rise of new variants. Therefore, vaccinating these individuals—and the population as a whole—continues to be important to slow the spread of the virus and save lives.
Are there any patients undergoing active cancer treatment who should not get vaccinated?
For patients who have just had a stem cell transplant or received CAR T-cell therapy, who are typically receiving immunosuppressive therapy, we continue to recommend that they delay COVID-19 vaccination (or revaccination as is recommended for patients undergoing these therapies) until at least 3 months after they’ve completed treatment. That’s based on data that [other] vaccines have had limited efficacy during periods when these patients are their most immunosuppressed.
All other patients who are being treated for cancer, including those getting aggressive chemotherapy, should get vaccinated and boosted without delay.
Will receiving the vaccine during cancer treatment make the cancer treatment less effective?
No. There is no evidence that any vaccines, including COVID-19 vaccines, make cancer therapy less effective.
And survivors, those not undergoing active cancer treatment. Are there any reasons they shouldn’t get vaccinated?
Many cancer survivors have weakened immune systems, so they may be at high risk of severe and/or persistent COVID-19. Cancer survivors also tend to be older and have other comorbidities—heart disease, kidney or lung dysfunction—so they’re going to have other reasons that will put them at risk for developing severe COVID-19. These are all reasons for them to get vaccinated.
And what about those who may be undergoing treatment soon, such as somebody just diagnosed with cancer or whose treatment has been delayed by the pandemic?
The best approach is to get the vaccine as soon as you can. However, we do recommend delays for patients undergoing stem cell transplant and those getting CAR T-cell therapy. In addition, cancer patients who are about to undergo surgery should wait a few days to up to 2 weeks after surgery to get vaccinated. This helps doctors know whether any symptoms—for example, a fever—are due to the surgery or the vaccine.
Can COVID-19 vaccines cause cancer? Can the vaccines cause cancer to recur or make it more aggressive?
There is no evidence that COVID-19 vaccines cause cancer, lead to recurrence, or lead to disease progression. Furthermore, COVID-19 vaccines do not change your DNA (i.e., your genetic code).
Can getting vaccinated cause a rise in tumor markers or signs of cancer recurrence just after a vaccination?
We are not aware of any evidence that suggests vaccines can affect cancer biomarkers in this way. However, we do know that the Pfizer and Moderna vaccines can lead to enlarged lymph nodes, particularly those in your armpit, called axillary lymph nodes. Developing new swelling in the armpit of your vaccinated arm a few days after getting your shot likely means the vaccine is producing a good immune response.
Some recently vaccinated people who have had imaging scans have had these lymph nodes “light up,” so our committee recommends talking to your cancer care team about any upcoming scans to make sure that they are aware of your recent vaccine. They may want to delay your scan unless it is urgent.
If you do get swelling after being vaccinated, and it doesn’t go away after about a week, make sure to tell your doctor.
I have lymphedema from lymph node surgery in one of my arms. Can I still get the shot in that arm?
Patients with lymphedema or those who have had a lymph node dissection in one arm, say for treatment of breast cancer, should get vaccinated in the other arm. Patients with lymphedema are at increased risk of infection and should avoid vaccinations in the affected arm.
If you have lymphedema in both arms, then the thigh can also be used as an alternate site for vaccine injection. In either case, if you have any lymphedema or have had a lymph node dissection, make sure you tell the personnel working at the vaccination site and they can vaccinate you in your other arm.
Is one COVID-19 vaccine better than another for people with cancer or cancer survivors?
CDC recommends that everyone age 6 months and older get a 2023–2024 updated COVID-19 vaccine to protect against serious illness from COVID-19. The three CDC-recommended vaccines are the Pfizer-BioNTech and Moderna mRNA vaccines (approved for people age 6 months and older) and the Novavax protein subunit vaccine (approved for people age 12 years and older). Aside from these age requirements, none of the 2023–2024 updated COVID-19 vaccines is preferred over another.
Are researchers collecting data on how effective the vaccines are in people with cancer?
A number of research groups are studying COVID-19 vaccine efficacy in people with cancer, from those with solid tumors to those receiving bone marrow transplants. For example, there are researchers looking at people who have blood cancers, like CLL or CML, because they are more likely to have immunodeficiency over a long period of time. Data from immunosuppressed patient populations have indicated that additional COVID-19 vaccine doses in the primary series and boosters can help improve immune responses in some people with cancer.
Every cancer doctor wants to know the answer to the question: How do my patients respond to these vaccines? There are lots of analyses that still need to be done—and so many subgroups of cancer patients and cancer treatments that require additional study. The more data we have that characterize vaccine responses in individual cancer populations, the better we can advise patients.
Do COVID-19 vaccines provide less protection to cancer patients or survivors?
Studies show that, compared with people who have never had cancer, COVID vaccines may be less effective in some people with cancer—in particular, patients with blood cancers (such as leukemia and lymphoma) or those receiving aggressive chemotherapy that weakens their immune systems.
The expectation is that most patients will respond to the vaccine. Patients with cancer may not see the same degree of protection from hospitalization from the vaccines seen in the general public. But any amount of protection is still a major benefit—particularly since these vaccines are best at preventing major complications from COVID-19.
Layers of prevention remain important for people with cancer, even if they are vaccinated, particularly those with hematologic malignancies, those who are getting chemotherapy or radiation, and those with other health conditions known to increase risk for COVID-19. We continue to recommend that these patients wear masks when in public places and avoid large get-togethers and crowds. These efforts are important because if you get COVID-19 it may lead to delays in your cancer treatment.
Existing COVID-19 vaccines do not prevent COVID-19 in all of those who get vaccinated, but they can prevent people with cancer from developing severe COVID-19 disease or hospitalization.
What about family members and caregivers of those with cancer? Is it important that they get vaccinated?
This is an underappreciated question. If you think about a vaccine strategy, if some people with cancer aren’t going to be fully protected by the COVID-19 vaccine, one of the best ways to protect them is to give the vaccine to people who will respond well. And that means anybody who they spend time with. So, anybody who is a caregiver, a loved one, or is in close contact with somebody with cancer, it’s important for them to get vaccinated and boosted, wear masks when out and about, avoid crowds, and take any other preventive measures.
These steps can help decrease a caregiver’s risk of developing symptomatic infections and symptomatic people are more likely to transmit the virus to people around them.
Vaccines and other precautions are also thought to help prevent transmission. So, when caregivers and loved ones take precautions, they may be less likely to get the virus and bring it home.
How do you see the approach to vaccination and booster shots changing over the coming months and years?
We know that immunity to coronaviruses, including SARS-CoV-2, wane over time. Additionally, viral variants can emerge that are better able to escape our immune responses. For these reasons, yearly boosters may be needed. Further research into the frequency and timing of additional boosters is ongoing, as are studies looking at more “variant-specific” boosters.