Surviving Life-Altering Effects of a Brain Tumor
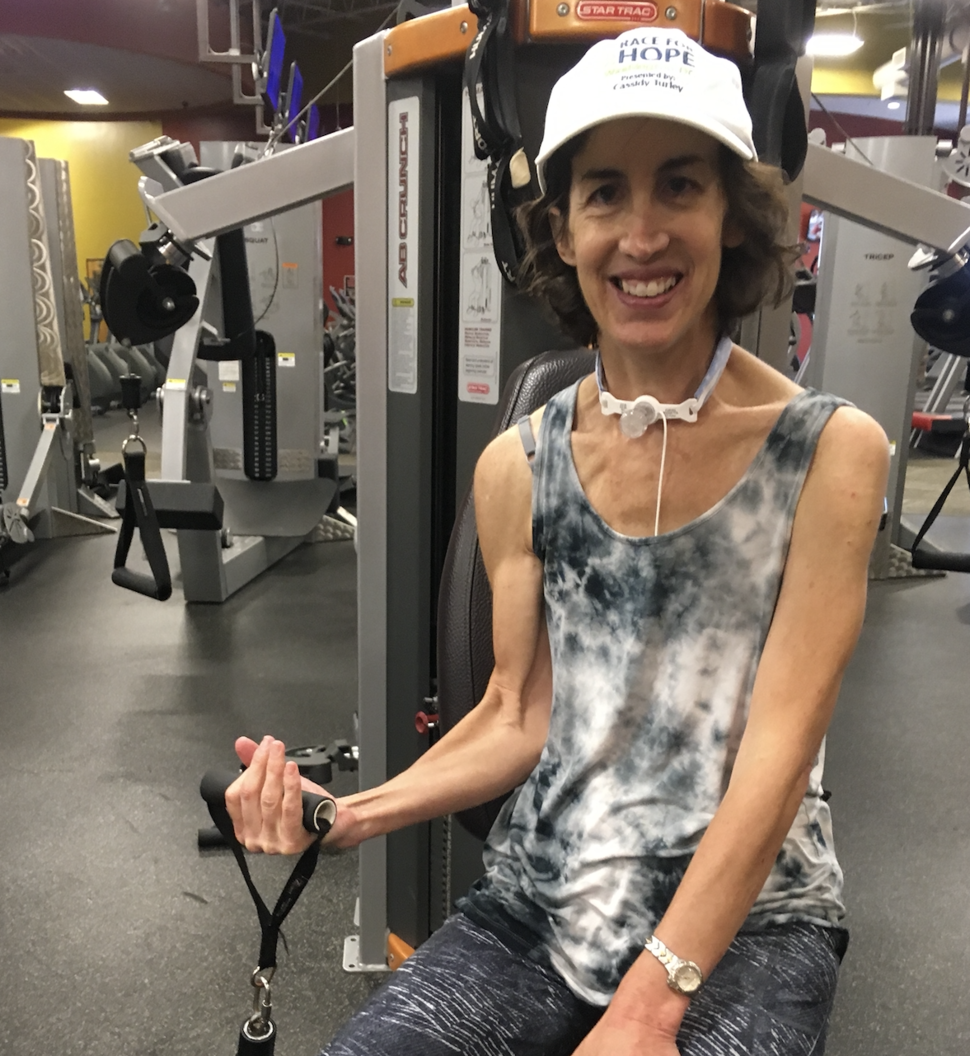
, by Carol, Ependymoma Survivor
Carol has spent nearly half her life living with her ependymoma diagnosis. She shares her long-term side effects and positive experiences from throughout her cancer journey.
In Memoriam
We pay tribute to the life of Carol. We are grateful she chose to share her diagnosis, treatment, and cancer journey with us to help improve treatments for others. She was kind, cared deeply for her family, and faced her challenges heroically. Our condolences go out to her family and friends.
In the year before I turned 30, I started having unusual symptoms, including nausea, vomiting, balance troubles, and violent hiccups. In April 2000, following months of tests and misdiagnoses, my sister insisted that we speak to a different doctor.
After a visit to the emergency room, I was diagnosed with an ependymoma, a rare tumor in the posterior fossa of my brain. The location makes it tough for surgeons to remove the entire tumor without damaging healthy brain tissue. This is where the skill of an experienced neurosurgeon comes in.
My tumor was nearly two inches long and was firmly attached to my brainstem. After surgery, I was hospitalized for nearly seven weeks due to several setbacks, including emergency abdominal surgery after doctors suspected that my PEG tube (a feeding tube they inserted because I could not swallow) had been placed incorrectly and post-operative pneumonia. I also had a tracheotomy and learned to speak with a Passy Muir Valve. I lost 20 pounds while in the hospital.
Thankfully, my incredible family and friends looked after me around-the-clock and advocated on my behalf. After hospitalization, I spent 10 days in in-patient rehab, which spurred my recovery.
Discovering Many Recurrences
One risk of any brain tumor is recurrence. My ependymoma has been relentless in its return. The first recurrence happened in 2003 and required a second surgery to remove 80 percent of the tumor. Removing the rest was simply too risky. I did whole-brain radiation, then chemotherapy, and later Gamma Knife surgery. The treatments left me with deficits. I was unable to drive, my speech was slurred, and I had trouble walking. My double vision, swallowing difficulties, and chronic headaches were permanent long-term effects.
The tumor spread again in 2014, but this time to my spine on my L1 and T6-9 vertebrae. I had two surgeries in October to remove the tumors. The pathology on both were grade 3 ependymoma. I also had my existing tracheotomy revised so I could begin using a ventilator at night to help with my breathing. A few days later, I had another PEG tube inserted in my stomach because I lost my ability to swallow. I was tube-fed until April 2015.
In the winter of 2016, a magnetic resonance imaging (MRI) scan revealed five new spinal cord tumors. I received 36 proton beam radiation treatments to my lower and mid-spine to pulverize the tumors and also bathe the spinal cord to help ward off future recurrences. I later had proton therapy on my cervical spine. Two of the tumors increased in size so I had a daily dose of lapatinib with Temodar for nine months. Still looking for a treatment, I tried Avastin to hopefully stabilize the tumors long-term. Unfortunately, this seemed to cause the tumors to grow, so I stopped that therapy after only a few months. Later I tried metronomic Temodar with a statin drug which did not stop the tumor growth. My most recent interventions were a total resection of my most worrisome tumor at level T3, followed by participation in the nivolumab clinical trial at NIH.
Surviving My Cancer Journey
I wish my fellow patients around the world could have access to the same superstar team of doctors that I've had, beginning with Neuro-Oncologist Mark Gilbert, M.D., of the NCI Center for Cancer Research's Neuro-Oncology Branch. Patients deserve the exceptional care offered at places like NIH. One special neuro-oncologist told me, "Brain tumor patients need TLC." She is so right!
I am grateful and surprised that I've lived this long through all my treatments, but it's only getting more difficult. My ependymoma tumors and treatments have affected nearly every part of me; I have double vision, speech and swallowing issues, and hearing loss (I now have hearing aids), as well as gait, balance, and coordination problems—add to that profound pain, most often in the form of a headache and in my muscles.
Sharing Hope
I urge you to keep your emotional health on your radar. It makes sense to focus on the physical treatment, but the emotional side is so important, too.
I need the support of my family and friends more than ever. I also benefit from the counsel of a therapist, who provides an objective ear and often has great tips to help navigate this rocky, unwanted life with cancer.
Helping others has also been important to help me cope. I believe that my participation in clinical trials might benefit future patients, even if I am too early for a cure. I launched a website in 2004 called Adult Ependymoma: A Patient's Story to share my experiences living with this disease. Over the years, I have heard from 300 survivors and caregivers from all over the world—we both give and receive advice and support.
Another highlight has been my family's participation in the Race for Hope in Washington, D.C., an annual road race that helps support brain cancer research. The spirit of the day and the outpouring of affection for all the survivors like me are powerful motivators.
The bottom line is: Although the damage I've experienced from this rare central nervous system tumor and its treatments is significant and life-altering, I am alive and hopeful that the research at NIH will help future patients.