An Immunotherapy Drug Trial Expands Across the Nation to Advance Research
, by Brittany Cordeiro, NCI-CONNECT Program Manager
NCI-CONNECT launched an immunotherapy drug trial across its national network of collaborative institutions to reach more people with rare brain and spine tumors, rapidly determine if the therapy is effective, and set the foundation for future trials.
Treatment options for rare brain and spine tumors are limited. So, when standard therapies such as chemotherapy, surgery, and radiation are not effective at preventing the tumor from returning, people have few or no options.
Marta Penas-Prado, M.D., associate research physician at the NCI Center for Cancer Research's Neuro-Oncology Branch (NOB), hopes to change this with a new multi-center clinical trial. The trial is studying the immunotherapy drug nivolumab in select recurrent rare central nervous system (CNS) cancers in adults. Nivolumab has proven effective in other cancers like melanoma, and its side effects are very well-known.
“This is a first-of-its-kind trial for these tumor types. After standard treatments fail, most people with these select rare CNS tumors don’t have access to experimental therapies, given the challenges of designing and conducting clinical trials for uncommon diseases,” says Dr. Penas-Prado, principal investigator of the nivolumab trial. The trial launched at NIH in 2017 and has enrolled 46 patients to date. Now, remarkably, the trial is opening at 10 other institutions across the United States that are part of the Brain Tumor Trials Collaborative (BTTC) network.
“This is an incredible opportunity for adults with these rare CNS cancers to have access to a clinical trial that uses an immunotherapy drug and is, hopefully, closer to their home or requires shorter travel,” says Dr. Penas-Prado.
Understanding the Trial Design
The drug nivolumab is an immune checkpoint inhibitor. By blocking immune checkpoint proteins, which generally keep immune responses from being too strong, immune checkpoint inhibitors restore the natural ability of immune cells called T cells to attack cancer cells.
Nivolumab blocks an immune checkpoint protein on T cells called PD-1 and is already broadly used to treat melanoma and many other cancer types. Immunotherapy offers promise to treat brain and spine cancers as well. “The fact that nivolumab has been tested in clinical trials for other cancers, and the FDA granted approval for some of them, means it has been used safely in clinical practice and is not an experimental drug that has never been used in humans,” explains Dr. Penas-Prado. The efficacy of the drug in these rare cancers is what the trial needs to prove.
The clinical trial is testing whether stimulating the immune system using nivolumab can shrink specific types of rare brain or spine tumors—or control the growth or spread of recurrent tumors. The trial is a basket trial, which means it is open to patients with different tumor types. Many of these tumors are so rare that designing trials specifically for them is not possible. The trial is also testing whether nivolumab can improve symptoms.
“It is very important to include patient-reported outcomes measures in the trial. If the drug can improve how a person feels and functions, it can be considered an effective treatment option,” says Dr. Penas-Prado.
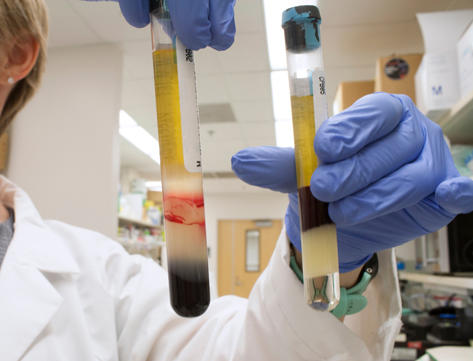
The clinical trial is also collecting blood and tumor tissue samples so researchers can study the tumor immune microenvironment. "This will help us understand why the treatment worked or didn’t work for specific tumor types, and from that information we can develop more studies," says Dr. Penas-Prado.
The study is for adults (age 18 or older) who are diagnosed with recurring CNS tumors, specifically 11 select rare CNS tumor types. A recurrence means the tumor was treated before and came back. Additional criteria for eligible patients include people who are not pregnant or breastfeeding and do not have hepatitis.
Expanding the Trial Across the Nation
NCI-CONNECT and Central Brain Tumor Registry of the United States (CBTRUS) data show the combined incidence for all 11 tumor types included on the nivolumab basket trial is 2,412 adults diagnosed per year, which is extremely rare. The lowest incidence is atypical teratoid rhabdoid tumor (ATRT) with less than 16 adults diagnosed per year, while the highest incidence is ependymoma with 923 adults diagnosed per year in the United States.
To reach more patients eligible to participate in the nivolumab basket trial, NCI-CONNECT looked to its network of investigators. The BTTC was created in 2003 as a network of professionals who investigate new treatments, allowing patients across a broad geographic range to participate in cutting-edge clinical trials and help medical professionals more rapidly determine the benefits of various therapies. It now includes over 30 institutions.
NCI-CONNECT identified 10 institutions to participate, including Washington University in St. Louis. “We are very excited to have the study open at our institution because there are no other treatment trials for these rare brain tumors,” says Jian Campian, M.D., Ph.D., associate professor in medical oncology and neurological surgery at Washington University School of Medicine.
Research shows that bringing studies closer to patients helps reduce barriers and enhance participation in clinical trials. “It is very gratifying to have a therapy to offer patients, which we have all been waiting years to have,” says Dr. Campian. “The study should also provide a lot of information about these tumors that can get us to the next phase of therapeutic options.”
The impact of opening the trial at institutions around the United States cannot be overstated. “Our aim is to prove the feasibility of conducting clinical trials for people with rare CNS tumors through collaborations among investigators,” says Dr. Penas-Prado. “Ultimately, this multi-center study should advance our understanding of these tumors, set the foundation for future trials, and provide better treatment options.