Common Moles, Dysplastic Nevi, and Risk of Melanoma
What is a common mole?
A common mole is a growth on the skin that develops when pigment cells (melanocytes) grow in clusters. Most adults have between 10 and 40 common moles. These growths are usually found above the waist on areas exposed to the sun. They are seldom found on the scalp, breast, or buttocks.
Although common moles may be present at birth, they usually appear later in childhood. Most people continue to develop new moles until about age 40. In older people, common moles tend to fade away.
Another name for a mole is a nevus. The plural is nevi.
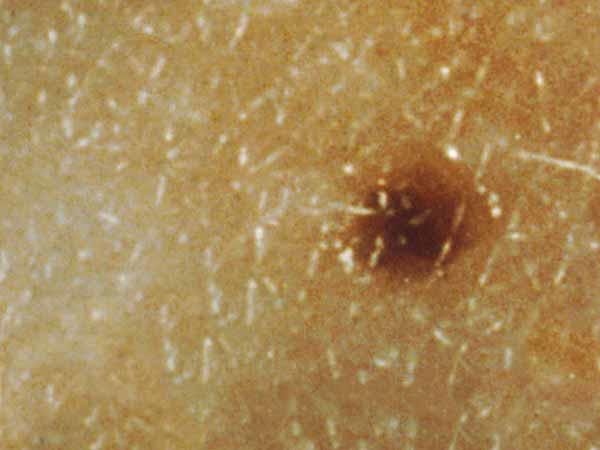
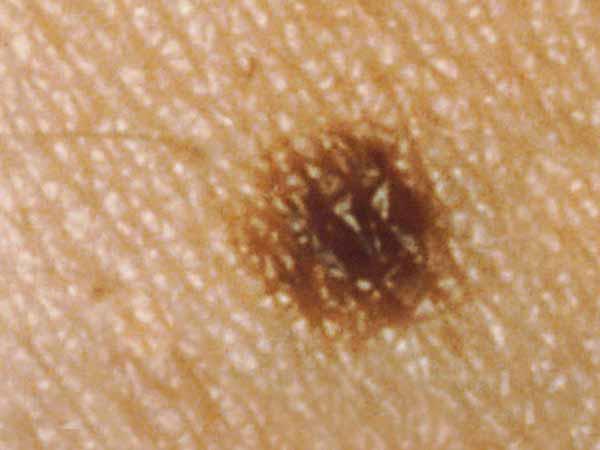
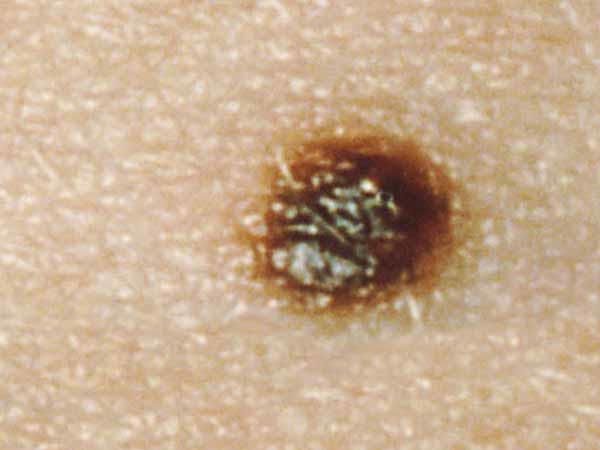
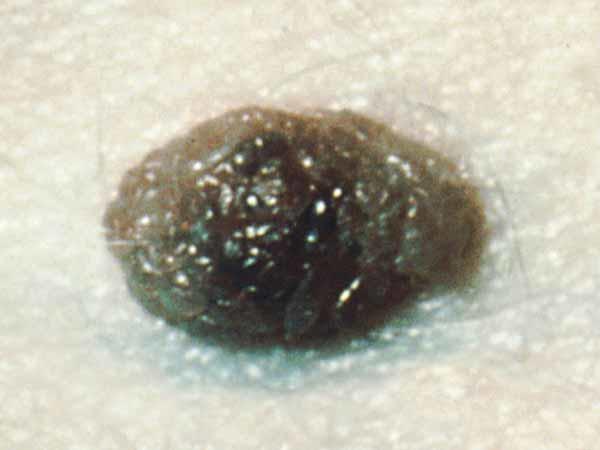
What does a common mole look like?
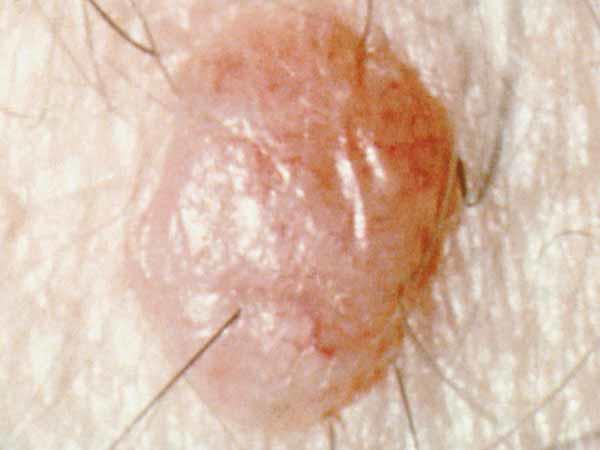
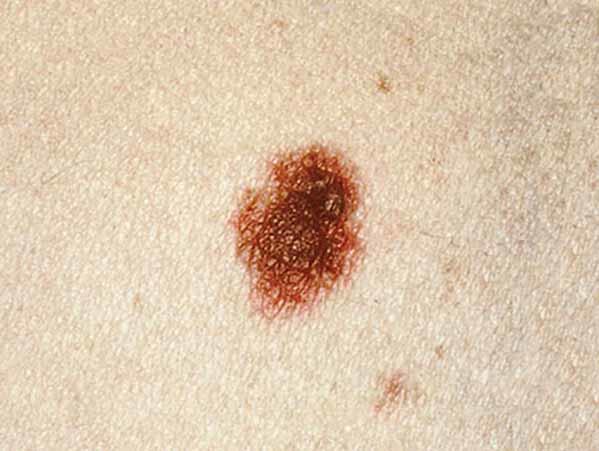
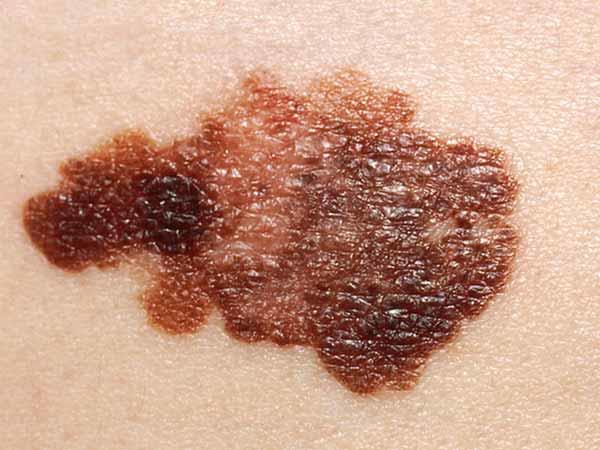
A common mole is usually smaller than about 5 millimeters wide (about 1/4 inch, the width of a pencil eraser). It is round or oval, has a smooth surface with a distinct edge, and is often dome-shaped. A common mole usually has an even color of pink, tan, or brown. People who have dark skin or hair tend to have darker moles than people with fair skin or blonde hair. Several photos of common moles are shown here, and What Does a Mole Look Like? has more examples.
Can a common mole turn into melanoma?
Only rarely does a common mole turn into melanoma, the most serious type of skin cancer.
Although common moles are not cancerous, people who have many small moles or several large ones have an increased risk of developing melanoma (1).
Certain changes in a mole may indicate that it is turning into a melanoma (2). People should tell their doctor if they notice
- The color of the mole changes
- The mole gets unevenly smaller or bigger (unlike normal moles in children, which get evenly bigger)
- The mole changes in shape, texture, or height
- The skin on the surface of the mole becomes dry or scaly
- The mole becomes hard or feels lumpy
- The mole starts to itch
- The mole bleeds or oozes
What is a dysplastic nevus?
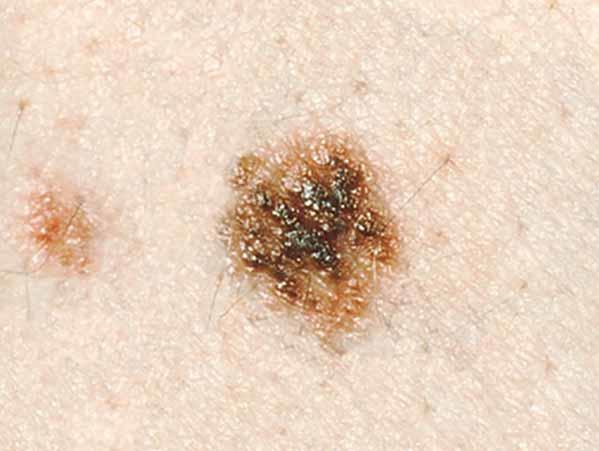
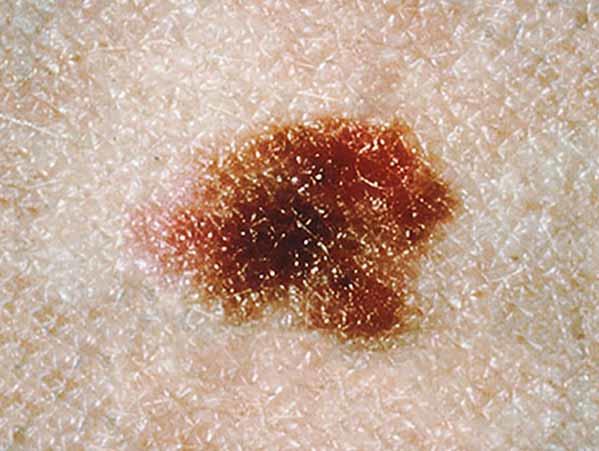
A dysplastic nevus is a type of mole that looks different from a common mole. (Some doctors use the term "atypical mole" to refer to a dysplastic nevus.) A dysplastic nevus may be bigger than a common mole, and its color, surface, and border may be different. It is usually more than 5 millimeters wide (1, 3). A dysplastic nevus can have a mixture of several colors, from pink to dark brown. It is usually flat, with a smooth, slightly scaly, or pebbly surface, and it has an irregular edge that may fade into the surrounding skin. Some examples of dysplastic nevi are shown here. What Does a Mole Look Like? has more examples.
A dysplastic nevus may occur anywhere on the body, but it is usually seen in areas exposed to the sun, such as on the back. A dysplastic nevus may also appear in areas not exposed to the sun, such as the breasts and areas below the waist (1, 3). Some people have only a couple of dysplastic nevi, but other people have more than 10. People who have dysplastic nevi usually also have an increased number of common moles.
Can a dysplastic nevus turn into melanoma?
Only rarely does a dysplastic nevus turn into melanoma (1, 3). However, dysplastic nevi are a risk factor for developing melanoma, and the more dysplastic nevi a person has, the greater their risk of developing melanoma (1, 3). Researchers estimate that the risk of melanoma is about 10 times greater for someone with more than five dysplastic nevi than for someone who has none.
What should people do if they have a dysplastic nevus?
Everyone should protect their skin from the sun and stay away from sunlamps and tanning booths, but for people who have dysplastic nevi, it is even more important to protect the skin and avoid getting a suntan or sunburn.
In addition, many doctors recommend that people with dysplastic nevi check their skin once a month (2, 4). People should tell their doctor if they see any of the following changes in a dysplastic nevus (2):
- The color changes.
- It gets smaller or bigger.
- It changes in shape, texture, or height.
- The skin on the surface becomes dry or scaly.
- It becomes hard or feels lumpy.
- It starts to itch.
- It bleeds or oozes.
People with dysplastic nevi should have their skin examined by a doctor regularly (2, 4). Sometimes, people or their doctors take photographs of dysplastic nevi so changes over time are easier to see (2). For people with more than five dysplastic nevi, doctors may conduct a skin exam once a year because of the moderately increased risk of melanoma. For people who also have a family history of melanoma, doctors may suggest a more frequent skin exam, such as every 3 to 6 months (3).
Should people have a doctor remove a dysplastic nevus or a common mole to prevent it from changing into melanoma?
No. Normally, people do not need to have a dysplastic nevus or a common mole removed. One reason is that very few dysplastic nevi or common moles turn into melanoma (1, 3). And most melanomas do not start as common moles or dysplastic nevi (2). That is why doctors usually remove only moles that have changed or new colored or otherwise suspicious areas on the skin.
What is melanoma?
Melanoma is a type of skin cancer that begins in melanocytes. It is potentially dangerous because it can invade nearby tissues and spread to other parts of the body, such as the lung, liver, bone, or brain. The earlier that melanoma is detected and removed, the more likely that treatment will be successful.
Most melanocytes are in the skin, and melanoma can occur on any skin surface. It can develop from a common mole or dysplastic nevus, but more often it develops in an area of apparently normal skin. In addition, melanoma can also develop in the eye (called uveal melanoma), under the nail, the digestive tract, and other areas of the body.
When melanoma develops in men, it is often found on the head, neck, or back. When melanoma develops in women, it is often found on the back or the lower legs.
People with dark skin are much less likely than people with fair skin to develop melanoma. For example, in 2017–2018, the lifetime risk of being diagnosed with melanoma was 2.9% (1 in 34) for White people but 0.1% (1 in 1,000) for Black people and 0.5% (1 in 200) for Hispanic people.
However, people with dark skin tend to be diagnosed with more advanced melanoma than people with fair skin (5). Advanced melanomas are harder to control and typically have a worse prognosis than melanomas diagnosed at an earlier stage. So it is very important that people with dark skin be aware of the warning signs of melanoma (see What does melanoma look like?). Melanomas in people with dark skin are typically found under the fingernails or toenails (usually initially appearing as a pigmented streak in the nail), on the palms of the hands, or on the soles of the feet.
What does melanoma look like?
Often the first sign of melanoma is a change in the shape, color, size, or feel of an existing mole. Melanoma may also appear as a new colored or otherwise unusual area on the skin.
The "ABCDE" rule describes the features of early melanoma (2, 6):
- Asymmetry. The shape of one half does not match the other half.
- Border that is irregular. The edges are often ragged, notched, or blurred in outline. The pigment may spread into the surrounding skin.
- Color that is uneven. Shades of black, brown, and tan may be present. Areas of white, gray, red, pink, or blue may also be seen.
- Diameter. There is a change in size, usually an increase. Melanomas can be tiny, but most are larger than 6 millimeters wide (about 1/4 inch wide).
- Evolving. The mole has changed over the past few weeks or months.
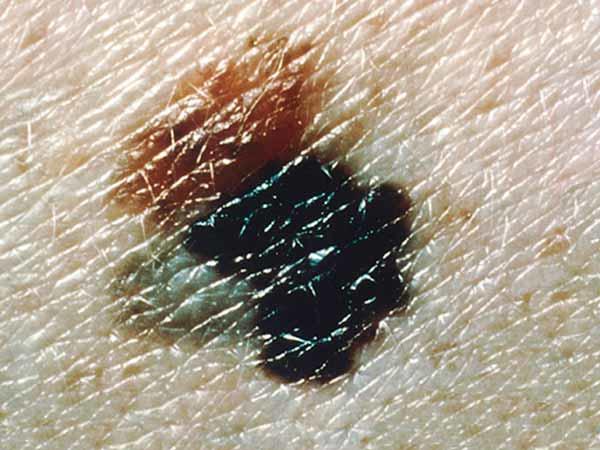
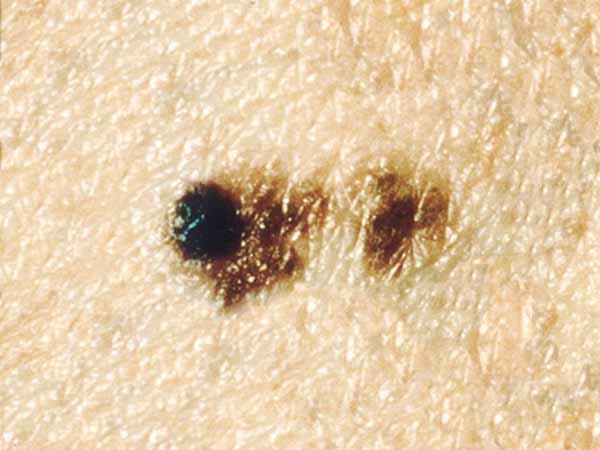
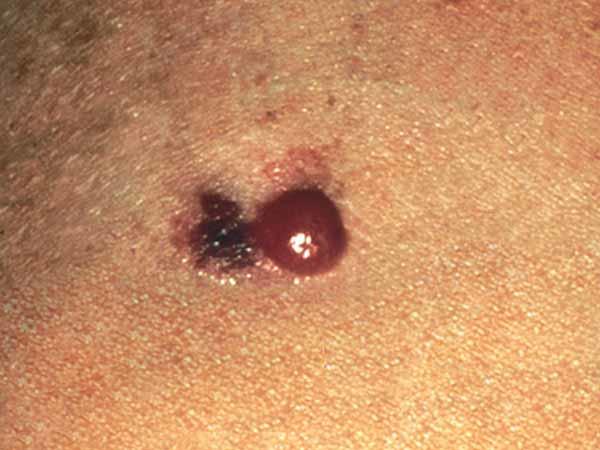
Melanomas can vary greatly in how they look. Many melanomas show all of the ABCDE features. However, some may show only one or two of the ABCDE features (6). Several photos of melanomas are shown here. More photos are on the What Does Melanoma Look Like? page.
In advanced melanoma, the texture of the mole may change. The skin on the surface may break down and look scraped. The mole may become hard or lumpy and the surface may ooze or bleed. Sometimes the melanoma is itchy, tender, or painful.
How is melanoma diagnosed?
The only way to diagnose melanoma is to remove tissue and check it for cancer cells. The doctor will remove all or part of the skin that looks abnormal. Usually, this procedure takes only a few minutes and can be done in a doctor's office, clinic, or hospital. The sample will be sent to a lab and a pathologist will look at the tissue under a microscope to check for melanoma.
What are the differences between a common mole, a dysplastic nevus, and a melanoma?
Common moles, dysplastic nevi, and melanoma vary by size, color, shape, and surface texture. The table below summarizes some differences between moles and cancer. Another important difference is that a common mole or dysplastic nevus will not return after it is removed by a full excisional biopsy from the skin, but melanoma sometimes grows back. Also, melanoma is cancer, so it can spread to other parts of the body.
| Questions | Common mole | Dysplastic nevus | Melanoma |
|---|---|---|---|
| Are they cancer? | No | No | Yes |
| Do they become cancer? | Rarely | Yes, but it is uncommon | It is cancer |
| How common are they? | Most Americans (about 332 million people) have common moles. | About 1 in 10 Americans have at least one dysplastic nevus (1). |
|
| How big are they? | Usually less than 5 millimeters wide, or about 1/4 inch | Often wider than 5 millimeters | Usually wider than 6 millimeters |
| What color are they? |
|
May be a mixture of tan, brown, and red or pink shades |
|
| What shape are they? | Usually round or oval, with a distinct edge that separates it from the rest of the skin |
|
|
| What's the surface texture? |
|
May have a smooth, slightly scaly, or rough, irregular, and pebbly appearance | May break down and look scraped, become hard or lumpy, or ooze or bleed |
What should people do if a mole changes or if they find a new mole or some other change on their skin?
People should tell their doctor if they find a new mole or a change in an existing mole. A family doctor may refer people with an unusual mole or other concerns about their skin to a dermatologist. A dermatologist is a doctor who specializes in diseases of the skin. Also, some plastic surgeons, general surgeons, internists, cancer specialists, and family doctors have special training in moles and melanoma.
What factors increase the risk of melanoma?
Although anyone can develop melanoma, people with the following risk factors have an increased risk of melanoma:
- Having a dysplastic nevus
- Having many small moles or several large ones
- Skin that burns easily: People who have fair (pale) skin that burns easily in the sun, blue or gray eyes, red or blond hair, or many freckles have an increased risk of melanoma.
- Sunlight: Sunlight is a source of UV radiation, which causes skin damage that can lead to melanoma and other skin cancers.
- Severe, blistering sunburns: People who have had at least one severe, blistering sunburn have an increased risk of melanoma. Although people who burn easily are more likely to have had sunburns as a child, sunburns during adulthood also increase the risk of melanoma.
- Lifetime sun exposure: The greater the total amount of sun exposure over a lifetime, the greater the risk of melanoma.
- Tanning: Although having skin that tans well lowers the risk of sunburn, even people who tan well without burning increase their risk of melanoma by spending time in the sun without protection.
- Use of sunlamps and tanning booths: UV radiation from artificial sources, such as sunlamps and tanning booths, can cause skin damage and melanoma.
- Personal history of melanoma: People who have had melanoma have an increased risk of developing other melanomas.
- Family history of unusual moles or melanoma: Melanoma sometimes runs in families. People who have two or more close relatives (mother, father, sister, brother, or child) with melanoma have an increased risk of melanoma. In rare cases, members of a family will have an inherited disorder that greatly increases the risk of melanoma. For example, people with xeroderma pigmentosum, have skin that is extremely sensitive to the sun because of a defect in DNA repair, which greatly increases their risk of melanoma. Another inherited disorder that increases the risk of melanoma is familial atypical multiple mole melanoma syndrome, which is usually caused by inherited mutations in the CDKN2A gene.
- Having a weakened immune system or being immunosuppressed: People who have a weakened immune system, including people with inherited disorders of the immune system, recipients of organ transplants (8), and people with lymphoma, have an increased risk of melanoma (9).
How can people protect their skin from the sun?
People can protect their skin from the sun by following the tips on NCI's Sunlight risk factor page. The best way to prevent melanoma is to limit exposure to sunlight. Having a suntan or sunburn means that the skin has been damaged by the sun, and continued tanning or burning increases the risk of developing melanoma.