Types of Cancer in Children
In the United States in 2025, an estimated 9,550 new cases of cancer will be diagnosed among children from birth to 14 years, and about 1,050 children are expected to die from the disease. Although cancer death rates for this age group have declined by 70 percent from 1970 through 2020, cancer remains the leading cause of death from disease among children. The most common types of cancer diagnosed in children ages 0 to 14 years are leukemias, brain and other central nervous system (CNS) tumors, and lymphomas.
NCI’s Cancer Stat Facts include detailed cancer rate and trend information for certain types of childhood cancer.
Treating Childhood Cancer
Children's cancers are not always treated like adult cancers. Pediatric oncology is a medical specialty focused on the care of children with cancer. It's important to know that this expertise exists and that there are effective treatments for many childhood cancers.
Types of Treatment
There are many types of cancer treatment. The types of treatment that a child with cancer receives will depend on the type of cancer and how advanced it is. Common treatments include: surgery, chemotherapy, radiation therapy, immunotherapy, and stem cell transplant. Learn about these and other therapies in our Types of Cancer Treatment section.
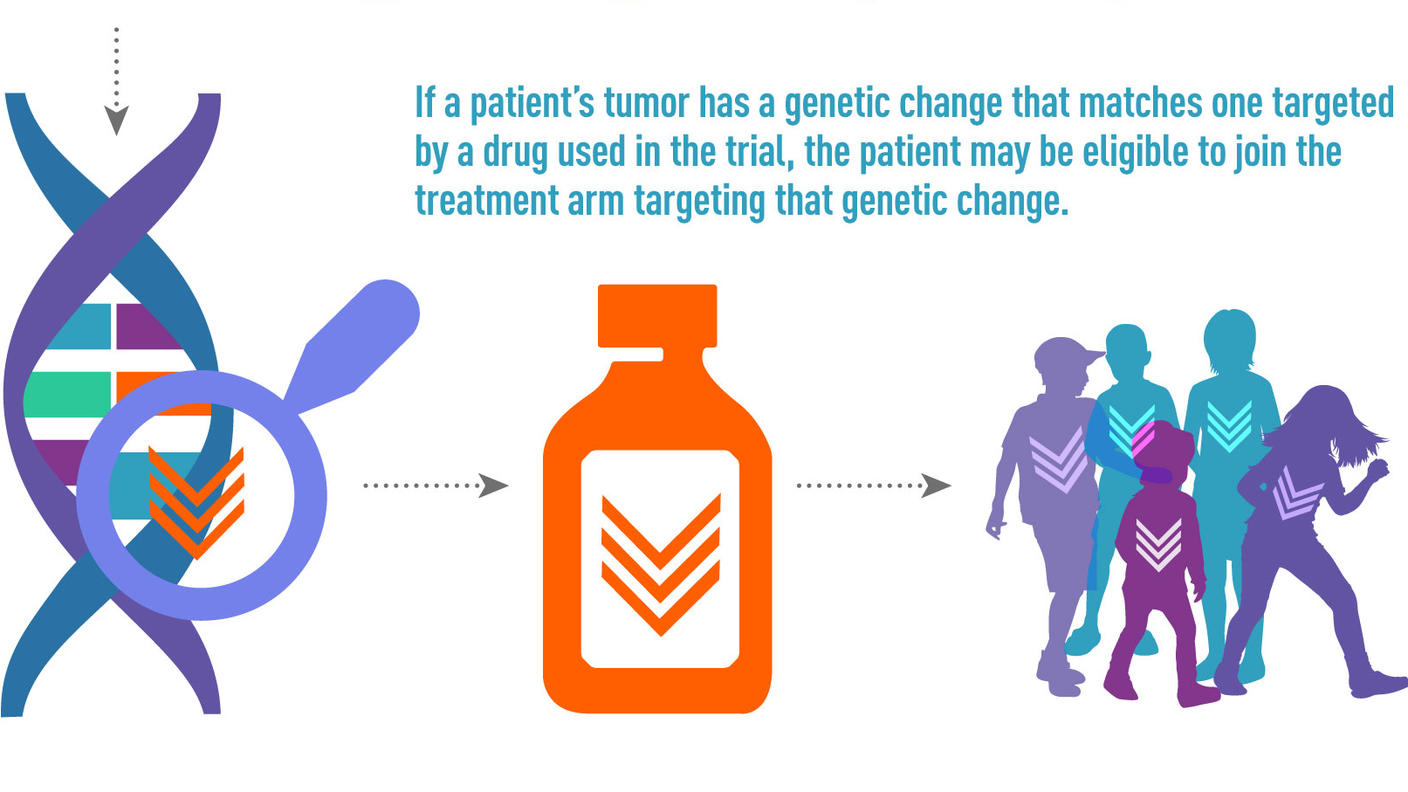
Clinical Trials
Before any new treatment can be made widely available to patients, it must be studied in clinical trials (research studies) and found to be safe and effective in treating disease. Clinical trials for children and adolescents with cancer are generally designed to compare potentially better therapy with therapy that is currently accepted as standard. Most of the progress made in identifying curative therapies for childhood cancers has been achieved through clinical trials.
Our site's Clinical Trials Information for Patients and Caregivers explains how clinical trials work. Information specialists who staff NCI’s Cancer Information Service can answer questions about the process and help identify ongoing clinical trials for children with cancer.
Treatment Side Effects
Children face unique issues during their treatment for cancer, after the completion of treatment, and as survivors of cancer. For example, they may receive more intense treatments, cancer and its treatments have different effects on growing bodies than adult bodies, and they may respond differently to drugs that control symptoms in adults. Late effects of treatment are discussed later on this page in the Survivorship section.
Where Children with Cancer Are Treated
Children who have cancer are often treated at a children’s cancer center, which is a hospital or unit in a hospital that specializes in treating children with cancer.
The doctors and other health professionals at these centers have special training and expertise to give complete care to children. Specialists at a children’s cancer center are likely to include primary care physicians, pediatric oncologists/hematologists, pediatric surgical specialists, radiation oncologists, rehabilitation specialists, pediatric nurse specialists, social workers, and psychologists. At these centers, clinical trials are available for most types of cancer that occur in children, and the opportunity to participate in a trial is offered to many patients.
Hospitals that have experts in treating children with cancer are usually member institutions of the NCI-supported Children’s Oncology Group (COG). COG is the world’s largest organization that conducts clinical research to improve the care and treatment of children with cancer. NCI's Cancer Information Service can help families find COG-affiliated hospitals.
At the NIH Clinical Center in Bethesda, Maryland, NCI’s Pediatric Oncology Branch cares for children and young adults with cancer. Health professionals and scientists conduct translational research that spans basic science to clinical trials to improve outcomes for children and young adults with cancer and genetic tumor predisposition syndromes.
Coping with Cancer
Adjusting to a child’s cancer diagnosis and finding ways to stay strong is challenging for everyone in a family. Our page, Support for Families When a Child Has Cancer, has tips for talking with children about their cancer and preparing them for changes they may experience. Also included are ways to help brothers and sisters cope, steps parents can take when they need support, and tips for working with the health care team. Various aspects of coping and support are also discussed in the publication Children with Cancer: A Guide for Parents.
Survivorship
It’s essential for childhood cancer survivors to receive follow-up care to monitor their health after completing treatment. All survivors should have a treatment summary and a survivorship care plan, as discussed on our Care for Childhood Cancer Survivors page. That page also has information on clinics that specialize in providing follow-up care for people who have had childhood cancer.
Survivors of any kind of cancer can develop health problems months or years after cancer treatment, known as late effects, but late effects are of particular concern for childhood cancer survivors because treatment of children can lead to profound, lasting physical and emotional effects. Late effects vary with the type of cancer, the child’s age, the type of treatment, and other factors. Information on types of late effects and ways to manage these can be found on our Care for Childhood Cancer Survivors page. The PDQ® Late Effects of Treatment for Childhood Cancer summary has in-depth information.
Survivorship care and adjustments that both parents and children may go through are also discussed in the publication Children with Cancer: A Guide for Parents.
Causes of Childhood Cancer
The causes of most childhood cancers are not known. About 8 to 10 percent of all cancers in children are caused by an inherited mutation (a genetic mutation that can be passed from parents to their children).
Most cancers in children, like those in adults, are thought to develop as a result of mutations in genes that lead to uncontrolled cell growth and eventually cancer. In adults, these gene mutations reflect the cumulative effects of aging and long-term exposure to cancer-causing substances. However, identifying potential environmental causes of childhood cancer has been difficult, partly because cancer in children is rare and partly because it is difficult to determine what children might have been exposed to early in their development. More information about possible causes of cancer in children is available in the fact sheet, Cancer in Children and Adolescents.
Research
NCI supports a broad range of research to better understand the causes, biology, and patterns of childhood cancers and to identify the best ways to successfully treat children with cancer. In the context of clinical trials, researchers are treating and learning from young cancer patients. Researchers are also following childhood cancer survivors to learn about health and other issues they may face as a result of their cancer treatment. To learn more, see Research on Childhood Cancers.