A meningioma is a primary central nervous system (CNS) tumor. This means it begins in the brain or spinal cord. Overall, meningiomas are the most common type of primary brain tumor. However, higher grade meningiomas are very rare.
To get an accurate diagnosis, a piece of tumor tissue will be removed during surgery, if possible. A neuropathologist should then review the tumor tissue.
What Are the Grades of Meningiomas?
Primary CNS tumors are graded based on a tumor tissue analysis performed by a neuropathologist. Meningiomas are grouped into three grades based on their characteristics. Each grade (1, 2, or 3, also written as I, II, or III) includes different meningioma subtypes.
- Grade 1 meningiomas are the most common meningiomas. They are low grade tumors, which means the tumor cells grow slowly.
- Grade 2 atypical meningiomas are mid-grade tumors. This means they have a higher chance of coming back after they’ve been removed. Grade 2 meningioma subtypes include chordoid and clear cell meningiomas.
- Grade 3 anaplastic meningiomas are malignant (cancerous). This means they are fast-growing tumors. Grade 3 meningioma subtypes include papillary and rhabdoid meningiomas.
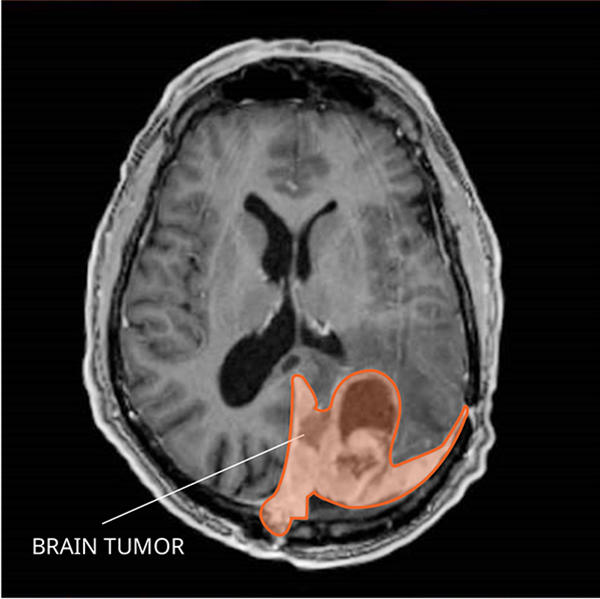
What Do Atypical and Anaplastic Meningiomas Look like on an MRI?
Grade 2 and 3 meningiomas usually appear as an enhancing mass on the outside lining of the brain tissue, which may or may not brighten with contrast on a magnetic resonance imaging (MRI) scan.
What Causes Atypical and Anaplastic Meningiomas?
Cancer is a genetic disease—that is, it is caused by certain changes to genes that control the way our cells function. Genes may be mutated (changed) in many types of cancer, which can increase the growth and spread of cancer cells.
The cause of meningiomas is not known. However, exposure to radiation, especially in childhood, can increase a person’s risk of developing a meningioma. People who have a genetic condition called Neurofibromatosis type 2 are also at increased risk.
Where Do Atypical and Anaplastic Meningiomas Form?
Meningiomas form along the dura mater—the outermost layer of tissue that covers and protects the brain and spinal cord. The dura mater is one of three layers that form the meninges. Meningiomas arise from meningeal cells. As a result, they tend to occur along the surface of the brain.
Do Atypical and Anaplastic Meningiomas Spread?
Meningiomas can spread to other areas of the CNS through cerebrospinal fluid (CSF). Grade 2 meningiomas can invade surrounding tissue, including nearby bone tissue. Grade 3 meningiomas have irregular cells and are likely to invade the brain or spread to other organs in the body.
What Are the Symptoms of Atypical and Anaplastic Meningiomas?
Symptoms related to a meningioma depend on the tumor’s location. Here are some possible symptoms that can occur:
- Vision changes
- Loss of hearing or smell
- Confusion
- Seizures
- Headaches that are worse in the morning
Who Is Diagnosed with Atypical and Anaplastic Meningiomas?
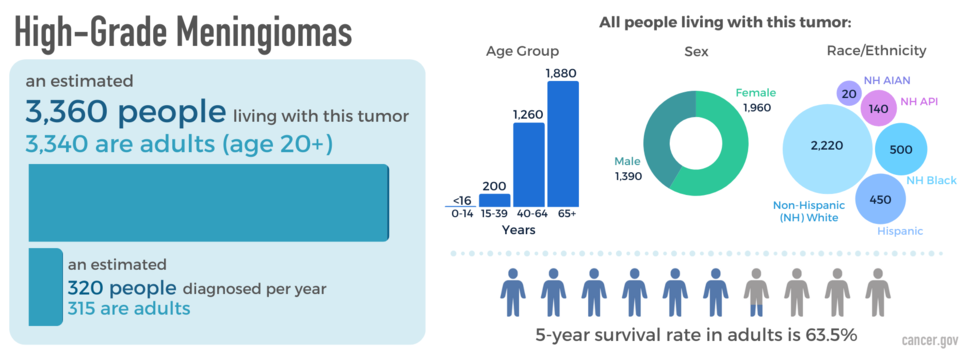
Grade 1 meningiomas are more common in females, but grades 2 and 3 occur more often in males. High-grade meningiomas are most common in non-Hispanic white people. High grade meningiomas tend to occur in people around 60 years old and risk of developing this tumor increases with age. An estimated 3,360 people are living with high-grade meningiomas in the United States.
What Is the Prognosis of Atypical and Anaplastic Meningiomas?
The likely outcome of the disease or chance of recovery is called prognosis. Prognosis is based on tumor grade, location, tumor type, extent of tumor spread, genetic findings, the patient’s age, and tumor remaining after surgery (if surgery is possible).
The relative five-year survival rate for high-grade meningioma is 63.5 percent. However, many factors can affect prognosis. These include the tumor grade and molecular type, the person’s age and health when diagnosed, and how they respond to treatment. If you want to understand your prognosis, talk to your doctor.
What Are the Treatment Options for Atypical and Anaplastic Meningiomas?
The first treatment for a malignant meningioma is surgery, if possible. The goal of surgery is to obtain tissue to determine the tumor type and remove as much tumor as possible without causing more symptoms.
Most people with atypical and anaplastic meningiomas receive additional treatments after surgery. These treatments may include radiation, chemotherapy, or clinical trials. Clinical trials test new chemotherapy, targeted therapy, or immunotherapy drugs. Treatments are decided by the patient’s health care team based on the patient’s age, remaining tumor after surgery, tumor type, and tumor location.
Open Clinical Studies for Atypical and Anaplastic Meningiomas
- PLX038 in CNS Tumors
- Immune Checkpoint Inhibitor Nivolumab for Patients with Rare CNS Cancers
- ONC206 for Patients with Rare CNS Neoplasms
Learn More
- Video: Clinical Trial Tests Nivolumab for Patients with Rare Brain and Spine Cancers
- Statistical Report Highlights Key Trends in Adolescents and Young Adults with Brain Tumors
- Modifying a Chemotherapy Drug Offers Hope to People with Rare Brain and Spine Tumors
- Smart Wearables Show Promise for Tracking Sleep Patterns in Brain Tumor Patients
- Read our NCI-CONNECTions Blog for current news and information on brain and spine tumors
Referrals
NCI-CONNECT doctors and nurses work with you and your primary doctor to collaborate on a comprehensive care plan that treats your brain or spine tumor. They will also help you cope with the physical and emotional aspects of your diagnosis. Learn about requesting a consultation >