Oligodendroglioma is a primary central nervous system (CNS) tumor. This means it begins in the brain or spinal cord. Diagnosing an oligodendroglioma requires finding two genetic alterations: an IDH mutation and a very specific change in the tumor cells’ chromosomes, where the short arm of chromosome 1 and the long arm of chromosome 19 are lost (also known as a 1p19q codeletion). Content on other IDH-mutated tumors will be coming soon to this page.
To get an accurate diagnosis, a piece of tumor tissue will be removed during surgery, if possible. A neuropathologist should then review the tumor tissue.
What Are the Grades of Oligodendrogliomas?
Primary CNS tumors are graded based on a tumor tissue analysis performed by a neuropathologist.
Oligodendrogliomas are grouped into two grades (grade 2 or grade 3, also written as grade II or grade III) based on their characteristics.
- Grade 2 oligodendrogliomas are low-grade tumors. This means the tumor cells grow slowly and invade nearby normal tissue. In many cases, they form years before being diagnosed because no symptoms appear.
- Grade 3 oligodendrogliomas are malignant (cancerous). This means they are fast-growing tumors. They are called anaplastic oligodendrogliomas.
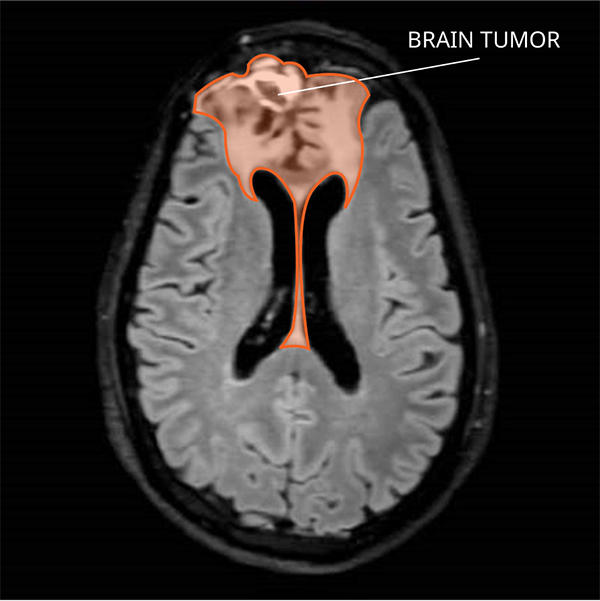
What Do Oligodendrogliomas Look like on an MRI?
Oligodendrogliomas usually appear as a single tumor with well-defined borders. They tend to have some swelling around them. The tumor may enhance with contrast on a magnetic resonance imaging (MRI) scan. This is most often seen in anaplastic oligodendrogliomas.
What Causes Oligodendrogliomas?
Cancer is a genetic disease—that is, it is caused by certain changes to genes that control the way our cells function. Genes may be mutated (changed) in many types of cancer, which can increase the growth and spread of cancer cells.
The cause of most oligodendrogliomas is not known.
However, exposure to radiation and certain gene changes that can be passed down through families have been linked to a higher chance of developing oligodendrogliomas.
Where Do Oligodendrogliomas Form?
Oligodendrogliomas are commonly found in the white matter and the outer layer of the brain called the cortex. However, they can also form anywhere in the CNS. They are called oligodendrogliomas because their cells resemble oligodendrocytes, a type of brain cell that supports and insulates nerve fibers in the CNS.
Do Oligodendrogliomas Spread?
Oligodendrogliomas can spread to other areas of the CNS through cerebrospinal fluid (CSF), but this is uncommon. They rarely spread outside the CNS to other organs.
What Are the Symptoms of an Oligodendroglioma?
Oligodendroglioma symptoms depend on the tumor’s location. The most common sign of an oligodendroglioma is a seizure. Around 60 percent of people have a seizure before being diagnosed.
Here are some additional symptoms people may have:
- Headaches
- Problems with thinking and memory
- Weakness
- Numbness
- Problems with balance and movement
Who Is Diagnosed with an Oligodendroglioma?
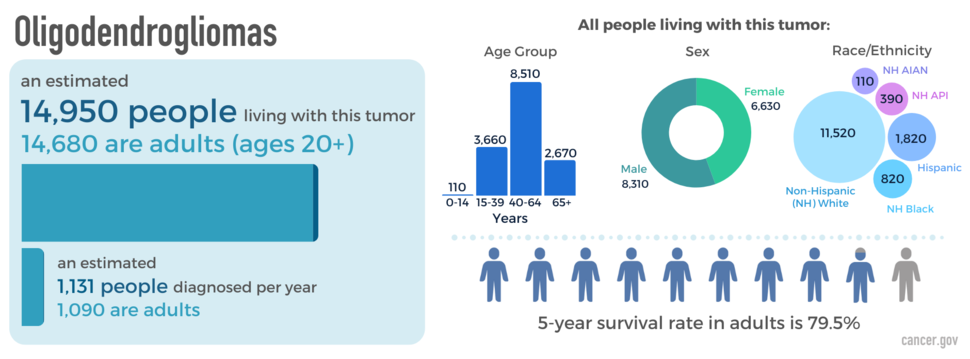
Oligodendrogliomas occur in people of any age but are most common in those between the ages of 35 and 44. They occur more often in males and are rare in children. They are most common in non-Hispanic white people. An estimated 14,950 people are living with this tumor in the United States.
What Is the Prognosis of an Oligodendroglioma?
The likely outcome of the disease or chance of recovery is called prognosis. Prognosis is based on tumor grade, location, tumor type, extent of tumor spread, genetic findings, the patient’s age, and tumor remaining after surgery (if surgery is possible).
The relative five-year survival rate for oligodendroglioma is 79.5 percent. However, many factors affect prognosis. These include the tumor grade and molecular type, the person’s age and health when diagnosed, and how they respond to treatment. If you want to understand your prognosis, talk to your doctor.
What Are the Treatment Options for Oligodendrogliomas?
The first treatment for an oligodendroglioma is surgery, if possible. The goal of surgery is to obtain tissue to determine the tumor type and remove as much tumor as possible without causing more symptoms. Treatments after surgery may include radiation, chemotherapy, or clinical trials. Clinical trials test new chemotherapy, targeted therapy, or immunotherapy drugs. Treatments are decided by the patient’s health care team based on the patient’s age, remaining tumor after surgery, tumor type, and tumor location.
Your oncologist might recommend a combination of medication, such as procarbazine, lomustine, and vincristine. A chemotherapy called temozolomide is also being studied in clinical trials.
Open Clinical Studies for Oligodendrogliomas
- PLX038 in CNS Tumors
- Zotiraciclib for Recurrent High-Grade Gliomas with IDH1 or IDH2 Mutations
- Nivolumab for Patients with IDH-Mutant Gliomas
- ONC206 for Patients with Rare CNS Neoplasms
Learn More
- Video: Clinical Trial Tests Nivolumab for Patients with Rare Brain and Spine Cancers
- New Clinical Trial Tests a Kind of Precision Medicine Treatment for IDH-Mutant Brain Tumors
- Oligodendroglioma Workshop Report
- A New Web-based Study of Low-Grade Gliomas
- Two Sons with a Rare Brain Cancer? We Choose to Fight through Advocacy
- Read our NCI-CONNECTions Blog for current news and information on brain and spine tumors
Referrals
NCI-CONNECT doctors and nurses work with you and your primary doctor to collaborate on a comprehensive care plan that treats your brain or spine tumor. They will also help you cope with the physical and emotional aspects of your diagnosis. Learn about requesting a consultation >