Medulloblastoma is a primary central nervous system (CNS) tumor. This means it begins in the brain or spinal cord.
To get an accurate diagnosis, a piece of tumor tissue will be removed during surgery, if possible. A neuropathologist should then review the tumor tissue.
What Are the Grades of Medulloblastomas?
Primary CNS tumors are graded based on a tumor tissue analysis performed by a neuropathologist. Medulloblastomas are all classified as grade 4 (also written as grade IV) tumors. This means they are malignant (cancerous) and fast-growing.
Additionally, medulloblastomas need staging—obtaining tests to detect if the tumor has spread to other areas of the CNS or outside the CNS. Using the stage of the cancer, the patient’s age, and whether the tumor remains after surgery (if surgery is possible), a health care team can estimate the risk of the tumor coming back. This also helps them decide on the best treatment. This process is called risk stratification, and medulloblastomas are classified into two risk groups: standard risk (or average risk) and high risk.
Currently, medulloblastomas are also classified based on their genetic features. There are at least four subgroups that have been identified in children and adults, although their frequency and genetic features vary depending on the age of the patient:
- WNT-activated
- SHH-activated
- Group 3 (non-WNT / non-SHH)
- Group 4 (non-WNT / non-SHH)
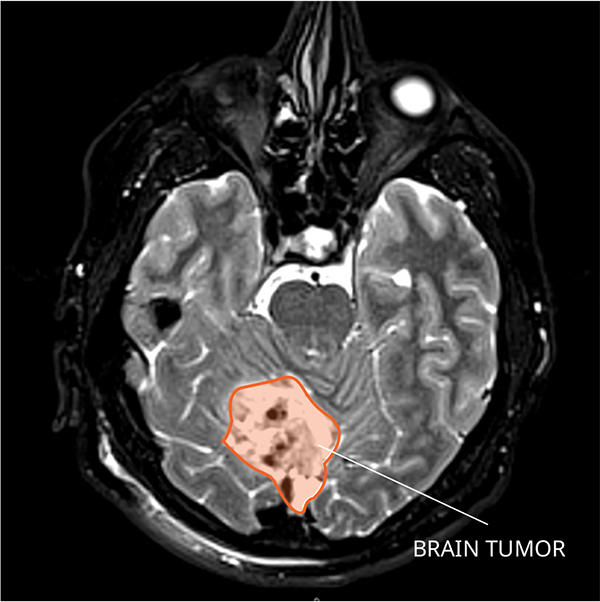
What Do Medulloblastomas Look like on an MRI?
Medulloblastomas usually appear as a solid mass in the cerebellum, which is the portion of the brain in the back of the head between the cerebrum and the brainstem. The tumor often brightens with contrast. It can also block the cerebrospinal (CSF) pathways, causing an abnormal build-up of fluid, which increases pressure on the skull. This is known as hydrocephalus. Once the mass is diagnosed as a medulloblastoma, a magnetic resonance imaging (MRI) scan of the spinal cord can show if it has spread.
What Causes Medulloblastomas?
Cancer is a genetic disease—that is, it is caused by certain changes to genes that control the way our cells function. Genes may be mutated (changed) in many types of cancer, which can increase the growth and spread of cancer cells. The cause of most medulloblastomas is not known. However, there’s a small percent of medulloblastomas that are related to gene changes and can be passed down through families.
Where Do Medulloblastomas Form?
Medulloblastomas most commonly form in the cerebellum, the bottom part of the brain located at the back of the skull. Medulloblastomas are known as embryonal neuroepithelial tumors, because they form in fetal cells that remain after birth.
Do Medulloblastomas Spread?
Medulloblastomas are very fast-growing. They often spread to other areas of the CNS through CSF. Medulloblastomas can also spread outside the CNS, for example, to the bones, lungs, or lymphatic system. This happens more frequently in children and in adults with recurrent tumors.
What Are the Symptoms of a Medulloblastoma?
Symptoms related to a medulloblastoma depend on the tumor’s location. Here are some possible symptoms that can occur.
People with a medulloblastoma in the cerebellum may have:
Issues with walking, balance, and/or fine motor skills
If the tumor is causing hydrocephalus, signs and symptoms may include:
- Headaches
- Nausea
- Vomiting
- Blurred and double vision
- Extreme sleepiness
- Confusion
- Seizures and even passing out
If a medulloblastoma has spread to the spine, symptoms may include:
- Weakness or numbness in the arms and/or legs
- A change in normal bowel or bladder habits
- Spinal pain
If a medulloblastoma has spread to other organs, symptoms may include:
- Coughing, chest pain, and shortness of breath
- Enlarged lymph nodes
- Bone pain
Who Is Diagnosed with a Medulloblastoma?
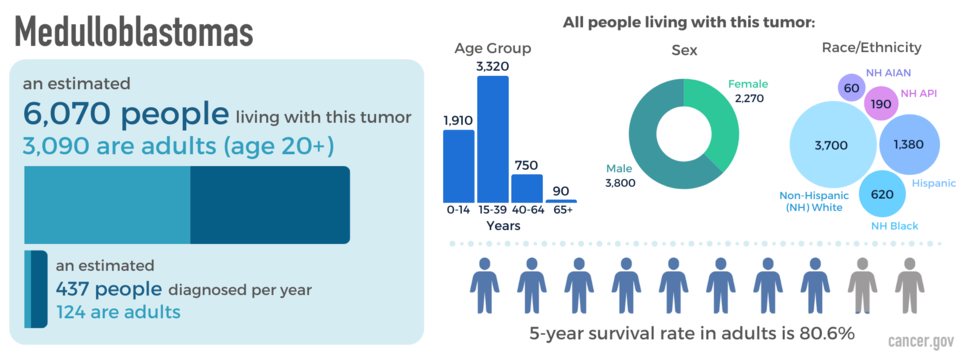
Seventy percent of medulloblastoma cases occur in children and 30 percent occur in adults. In adults, medulloblastoma typically affects those between 20 and 40 years of age.
Medulloblastomas occur more often in males than females. They are most common in non-Hispanic white and Hispanic people. An estimated 6,070 people are living with this tumor in the United States.
What Is the Prognosis of a Medulloblastoma?
The likely outcome of the disease or chance of recovery is called prognosis. The relative five-year survival rate for medulloblastoma is 80.6 percent. However, many factors can affect prognosis. These include the tumor molecular group, staging, extent of resection, the person’s age and health when diagnosed, and how they respond to treatment. If you want to understand your prognosis, talk to your doctor.
What Are the Treatment Options for a Medulloblastoma?
The first treatment for medulloblastoma is surgery, if possible. The goal of surgery is to obtain tissue to determine the tumor type and remove as much tumor as possible without causing more symptoms for the person.
Most people with medulloblastomas also receive additional treatments. These may include radiation, chemotherapy, or clinical trials. Because this disease tends to spread in the brain and spine, surgery is usually followed by radiation to the entire brain and spine (called craniospinal radiation). Proton beam radiation therapy is often recommended, because of problems with bone marrow and surrounding organs that occur due to brain and spine radiation.
Chemotherapy is often part of the treatment plan, depending on the tumor subtype, how much the tumor has spread, how the person responds to treatment, the side effects, and the impact on their quality of life.
Clinical trials—with new chemotherapy, targeted therapy, or immunotherapy drugs—may also be available. It is important to seek expert recommendations from a neuro-oncologist with experience in adult medulloblastoma. Treatments are decided by the patient’s health care team based on the patient’s age, the tumor remaining after surgery, tumor type, and tumor location.
Open Clinical Studies for Medulloblastoma
- PLX038 in CNS Tumors
- Immune Checkpoint Inhibitor Nivolumab for Patients with Rare CNS Cancers
- ONC206 for Patients with Rare CNS Neoplasms
Learn More
- Video: Clinical Trial Tests Nivolumab for Patients with Rare Brain and Spine Cancers
- Statistical Report Highlights Key Trends in Adolescents and Young Adults with Brain Tumors
- Modifying a Chemotherapy Drug Offers Hope to People with Rare Brain and Spine Tumors
- Smart Wearables Show Promise for Tracking Sleep Patterns in Brain Tumor Patients
- Adult Medulloblastoma Workshop Report
- Researching Medulloblastoma with Care and Knowledge
- Read our NCI-CONNECTions Blog for current news and information on brain and spine tumors
Referrals
NCI-CONNECT doctors and nurses work with you and your primary doctor to collaborate on a comprehensive care plan that treats your brain or spine tumor. They will also help you cope with the physical and emotional aspects of your diagnosis. Learn about requesting a consultation >