Could Bacteria Help Find Cancer?
, by Elia Ben-Ari
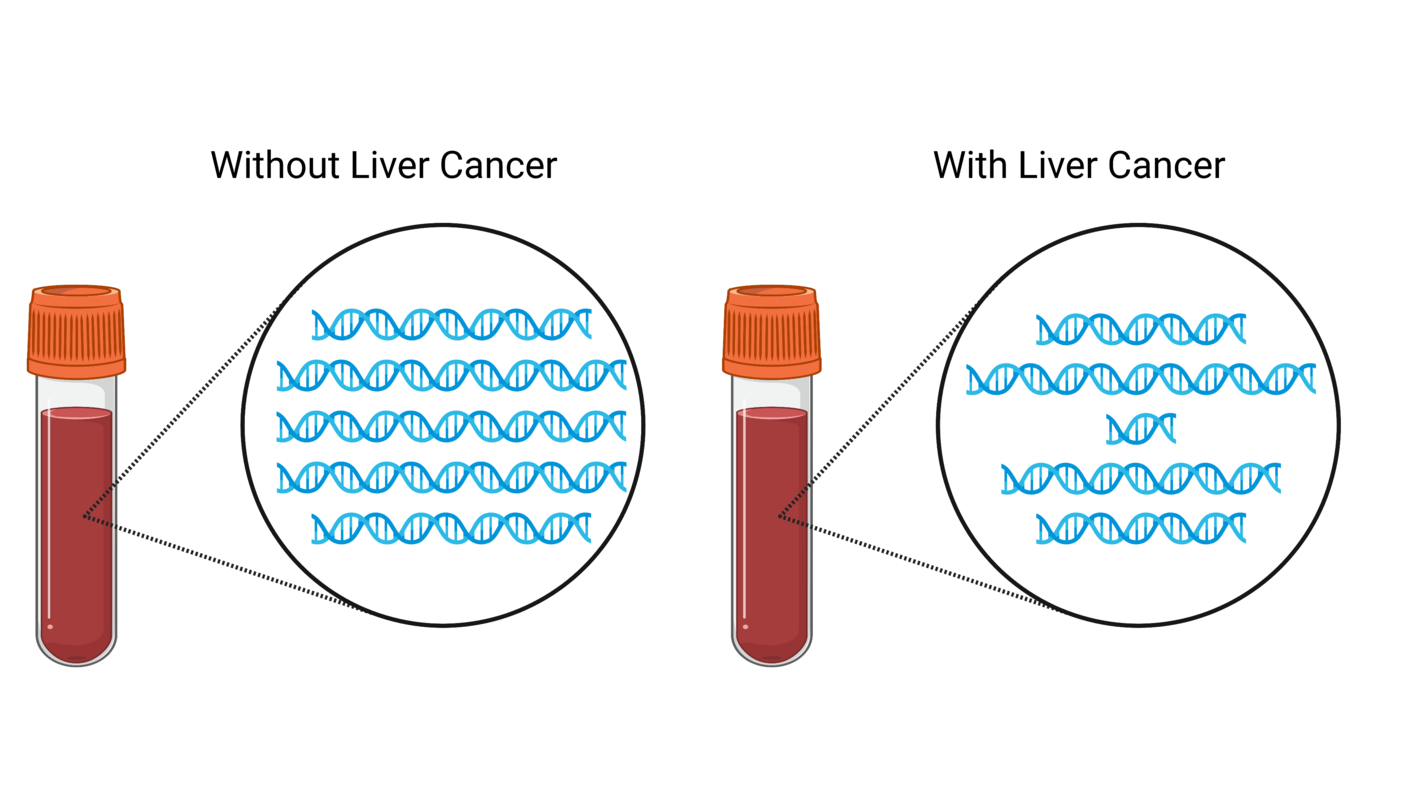
A team of US and Australian scientists has engineered bacteria that can detect DNA that has been released from tumors.
In a new study, the team showed that, in mice, their engineered “bacterial biosensors” picked up mutated DNA shed into the gut by colorectal tumors.
The bacteria are programmed to go on a sort of molecular manhunt, seeking and capturing DNA with mutations in the KRAS gene. When the mutated DNA is captured, a genetic switch is tripped, triggering the bacteria to put out a signal indicating that cancer was detected.
The results were published August 11 in Science.
In addition to detecting cancer noninvasively, these bacterial biosensors could possibly be designed to diagnose the precise type of cancer they’re finding, said Miguel Ossandon, Ph.D., of NCI’s Division of Cancer Treatment and Diagnosis (DCTD), who was not involved in the research.
There’s also the potential to use the engineered bacteria to deliver treatments to tumors in the gut when and where they’re detected, said one of the study’s senior investigators, Daniel Worthley, M.D., Ph.D., of the Colonoscopy Clinic in Brisbane, Australia. In other words, “to unite diagnosis and therapy,” Dr. Worthley said.
At least one previous study has reported the engineering of bacteria to detect cancer. But, according to DCTD's Avraham Rasooly, Ph.D., who also was not involved in the work, this study describes the most advanced engineering of bacteria specifically for cancer detection and, potentially, diagnosis.
However, Dr. Rasooly added, much more work is needed before the approach could be used in people.
And the new technology won’t replace colonoscopy—at least, not anytime soon, Dr. Worthley said. Colonoscopy is still the best way to find and remove precancerous growths in the gut, he noted.
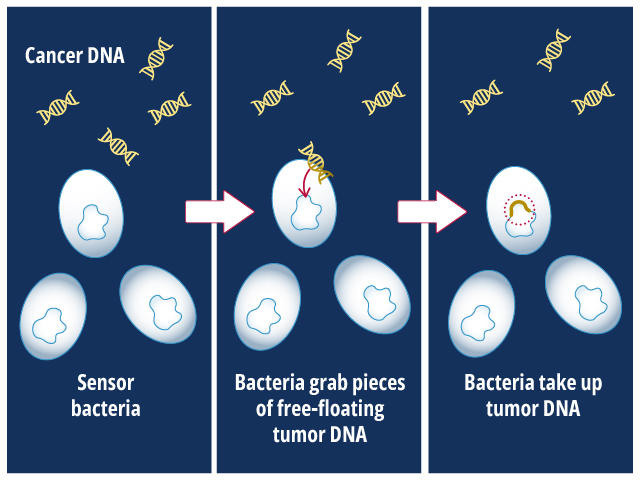
Bacteria can take up DNA from their environment
To create the biosensors, the scientists exploited a natural ability of many bacteria. The bacteria can grab free-floating DNA from their environment and stitch it into their own genomes in place of a similar piece of DNA, explained co-lead investigator Robert Cooper, Ph.D., of the University of California San Diego. Under normal circumstances, this ability lets bacteria gain new traits that help them grow and survive.
The team used a type of bacteria called Acinetobacter baylyi that’s especially good at pulling in DNA from its surroundings. A. baylyi bacteria can live in a mouse’s gut but “are generally not found in people,” Dr. Cooper said.
Using genetic engineering techniques, the scientists programmed the bacteria to find and take up snippets of KRAS. Harmful mutations in KRAS fuel many cases of colorectal cancer and other cancers, including lung and pancreatic.
The team further rigged the bacteria so that if they take up one particularly harmful form of mutated KRAS called G12D, they respond by switching on a gene that makes them resistant to the antibiotic kanamycin. Resistance to kanamycin can easily be detected in the lab by seeing if the bacteria grow in the drug’s presence.
Testing the engineered bacteria
In a series of lab dish experiments, the team showed that the engineered bacteria could detect DNA containing KRAS G12D from lab-grown colorectal cancer cells and organoids (mini-organ-like structures). Bacteria that took up KRAS G12D—but not normal, unmutated KRAS—were able to grow in petri dishes laden with kanamycin.
Finally, the team delivered the engineered bacteria directly into the gut of mice with or without colorectal tumors. Only A. baylyi bacteria recovered from the gut of animals with tumors grew in the presence of kanamycin. And the genomes of those bacteria were shown to contain the altered KRAS gene.
For this initial set of experiments, Drs. Worthley and Cooper explained, they used an optimized system to ensure the best chances of success. That included using tumor DNA engineered in the lab as the “donor DNA” to be picked up by the engineered bacteria.
Once the team had shown that their basic engineering concept worked, they further engineered A. baylyi to detect “natural, non-engineered” tumor DNA.
So far, Dr. Cooper said, this retooled biosensor “will work in a lab dish but is not accurate enough to work well in mice,” meaning it could give false-negative as well as false-positive results. However, he said, “we think that’s a surmountable obstacle.”
One thing is clear, the research team and experts not involved in the study agreed: More work is needed to develop and fine-tune the new technology for possible use in cancer care.
That will include adapting the system for use with types of bacteria that are better suited for human use, such as those that are able to live in the human gut, and developing a way to deliver the bacteria by mouth. It also means further engineering and testing the system to ensure it’s safe.
And to apply the approach beyond cancers of the gut, more research will be needed to engineer bacteria “so they are able to get into less-accessible tumors, like those in the pancreas,” Dr. Ossandon said.
A "modular" and adaptable approach
“This is a novel approach … that has a lot of potential to build on and improve,” said Claudia Gravekamp, Ph.D., of Albert Einstein College of Medicine, who works on bacteria-based cancer therapies and vaccines and was not involved in the new study.
Because the bacteria are engineered with components that can easily be switched out, the approach “is adaptable to detecting other types of known cancer-causing mutations and could be applied to a number of different settings,” said Phil Daschner, M.S., a program director in NCI’s Division of Cancer Biology, which funded the work.
One advantage of this “modular” genetic engineering technique, Dr. Cooper explained, is that “we can easily tell the bacteria to look for other bits of DNA,” and to respond in different ways once cancer is detected.
For example, he continued, the bacteria might be engineered to produce a compound that is easily detected in a urine or blood sample instead of becoming resistant to an antibiotic.
And while the proof-of-principle study was limited to detecting a single KRAS mutation often seen in colorectal cancer, the bacteria could also be engineered to detect mutations more commonly found in other types of cancer, Daschner said.
Indeed, Dr. Cooper said, the team hopes to engineer the bacteria to detect more than one genetic mutation at a time.
Another potential advantage of the new approach compared with other tests that screen for cancer, Daschner said, is that “the bacteria can detect the mutated DNA where it is, [and] when the mutation happens.”
DNA is often destroyed by enzymes in the gut, “so unless there’s a lot of tumor DNA, other tests, such as [existing] stool-based tests, might not detect it in a sample,” he continued.
Envisioning a wide range of possible clinical uses
For Dr. Worthley, the real long-term promise of the engineered bacteria is as a form of targeted therapy, not just as a way to look for cancer. Because the bacteria “can respond directly at the time and place of disease detection,” he explained, they could be used to deliver treatments on the spot once cancer—or even a precancerous lesion—is detected.
Dr. Worthley holds stock in a company that is developing engineered bacteria for cancer therapy, which was co-founded by another senior author on the study, Jeff Hasty, Ph.D., of UC San Diego.
On the other hand, Drs. Rasooly and Ossandon believe the most exciting potential of the technology, which was not discussed in the study, is as a noninvasive alternative to tissue biopsy for diagnosing and monitoring cancer.
Instead of a tissue biopsy, which may involve a large needle or surgery, they said, engineered bacteria could someday be used to “sample” tumor DNA from the gut—and perhaps also tumors in other parts of the body—and deliver the DNA for genetic analysis. This could potentially revolutionize cancer biopsy and diagnosis, Dr. Rasooly said.
However, Dr. Ossandon noted, this possible application is “way in the future.”
In the nearer term, Dr. Gravekamp proposed, the engineered bacteria could be used outside the body as a sensitive way to detect specific cancer-related mutations in patient blood samples.
“If [the researchers] were able to get that working, it would be beautiful and may be applicable to so many cancers,” she said.