Treatment of Non-Hodgkin Lymphoma (NHL)
Most people diagnosed with lymphoma have a subtype of non-Hodgkin lymphoma. Non-Hodgkin lymphoma can either be aggressive or indolent.
Aggressive non-Hodgkin lymphoma grows and spreads quickly and usually requires immediate treatment. With modern treatment regimens, almost 70% of people with aggressive non-Hodgkin lymphoma will be considered cured. Research is now largely focused on finding better treatments for the minority of people with aggressive lymphoma who are not cured with initial therapy.
Indolent non-Hodgkin lymphoma grows slowly, and in some cases may not cause symptoms for years. People with indolent disease can often postpone treatment until their symptoms worsen, with no negative effects on survival. Sometimes, an indolent lymphoma can turn into aggressive lymphoma, which requires immediate treatment.
Indolent non-Hodgkin lymphoma largely cannot be cured with currently available therapies. The past two decades have seen improvements in extending the survival of people who are treated for this type of lymphoma. However, researchers are studying how to improve long-term survival further and working toward potentially curative treatments.
Chemotherapy, radiation therapy, targeted therapy, and immunotherapy are all used in the treatment of non-Hodgkin lymphoma. A stem cell transplant is sometimes used for lymphoma that has recurred, but this procedure has serious side effects. Four CAR T-cell therapies have been approved to treat some types of recurrent lymphoma. However, these newer therapies still can't cure many people with recurrent lymphoma.
Most research on treatment for non-Hodgkin lymphoma is now focused on targeted therapy and immunotherapy. Researchers are also trying to identify gene changes in different types of lymphoma that might be targets for new drug development.
For example, in 2018, a study led by NCI researchers identified genetic subtypes of diffuse large B-cell lymphoma (the most common type of non-Hodgkin lymphoma) that could help explain why some patients with the disease respond to treatment and others don’t. Further studies may lead to more tailored treatments for patients with this type of lymphoma.
New targeted therapies
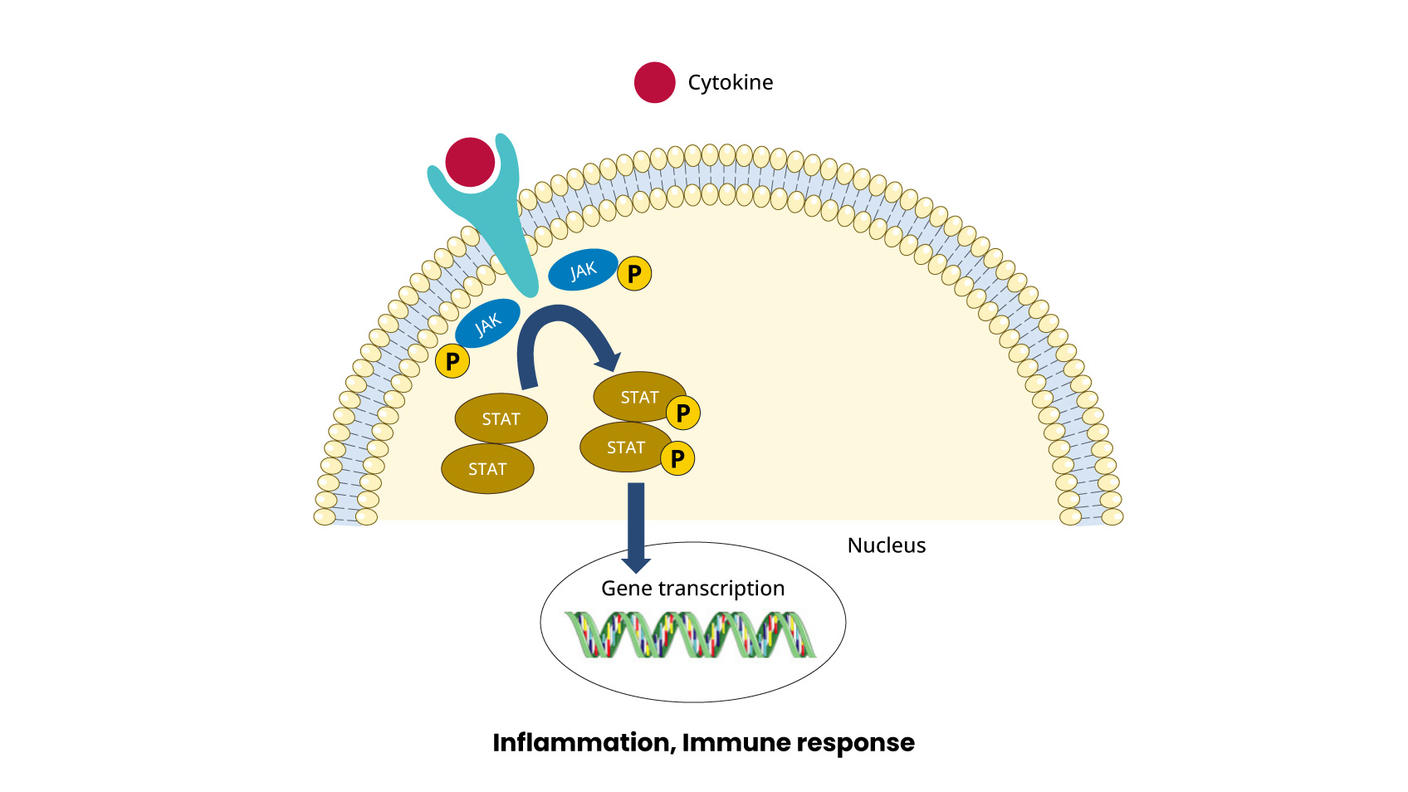
A signaling pathway is a series of chemical reactions that control one or more cell functions. Many types of non-Hodgkin lymphoma are driven by a signaling pathway called the B-cell receptor signaling pathway. A drug called ibrutinib (Imbruvica) has been developed to shut down that pathway. It is being used and tested in a number of ways:
- In the last several years, the drug has been approved for the treatment of small lymphocytic lymphoma and Waldenstrom macroglobulinemia, both indolent non-Hodgkin lymphomas.
- NCI took part in a randomized clinical trial that tested the addition of ibrutinib to chemotherapy and rituximab (Rituxan) in people newly diagnosed with a certain type of diffuse large B-cell lymphoma. People over the age of 60 had worse outcomes with the addition of ibrutinib. However, patients under the age of 60 who were given ibrutinib had substantially improved survival.
- Other studies have suggested that people whose diffuse large B-cell lymphoma has specific genetic characteristics may especially benefit from treatment with ibrutinib.
- An early-phase NCI-supported study tested ibrutinib plus chemotherapy in people with primary central nervous system lymphoma, a very aggressive subtype of non-Hodgkin lymphoma. More than half of the patients in this small study went into complete, long-term remission.
- Two larger studies at the NIH Clinical Center have been testing additional treatment regiments that include ibrutinib and chemotherapy. One is testing the combination plus the targeted drug rituximab in patients with primary central nervous system lymphoma. The second is testing a similar combination in people with lymphoma that began elsewhere in the body but has spread to the central nervous system.
The FDA has approved three other drugs that target the B-cell receptor signaling pathway: acalabrutib (Calquence), zanubrutinib (Brukinsa), and pirtobrutinib (Jaypirca).
- Acalabrutinib is approved for relapsed mantle cell lymphoma and small lymphocytic lymphoma. An ongoing study at NCI is testing acalabrutinib, in combination with chemotherapy and rituximab, in people with previously untreated diffuse large B-cell lymphoma.
- In 2019, zanubrutinib was approved for relapsed mantle cell lymphoma.
- In 2024, the combination of zanubrutinib with obinutuzumab (Gazyva), a drug that kills B cells, was approved for follicular lymphoma that has relapsed or not responded to initial treatment.
- In 2023, pirtobrutinib was approved for the treatment of mantle cell lymphoma and for chronic lymphocytic leukemia and small lymphocytic lymphoma that has gotten worse after two or more previous treatments. This drug is now being tested in clinical trials for several different types of non-Hodgkin lymphoma.
Many other targeted therapies are being studied in non-Hodgkin lymphoma. Some that are approved for specific subtypes are listed below.
- Venetoclax (Venclexta) for chronic lymphocytic leukemia and small lymphocytic lymphoma.
- Loncastuximab (Zynlonta) for large B-cell lymphoma that has recurred or did not shrink after other treatments.
- Selinexor (Xpovio) for large B-cell lymphoma that has recurred or did not shrink after other treatments.
- The combination of tafasitamab (Monjuvi) and lenalidomide (Revlimid) for people with large B-cell lymphoma who cannot undergo a stem cell transplant.
- Tazemetostat (Tazverik) for some people with follicular lymphoma that has recurred or did not shrink after other treatments.
- Polatuzumab vedotin (Polivy) for the treatment of diffuse large B-cell lymphoma. Clinical trials are testing this drug and related drugs for other types of non-Hodgkin lymphoma.
However, in lymphoma, resistance to a single agent can develop quickly. Researchers are now testing combinations of targeted therapies to treat non-Hodgkin lymphoma to try to overcome resistance. For example, ongoing trials led by NCI researchers are testing a five-drug regimen and a six-drug regimen in people with aggressive or indolent B-cell lymphomas whose cancer has relapsed or is resistant to treatment.
Early results showed that the five-drug regimen, called ViPOR, shrank tumors substantially in about half of participants. Over a third of patients’ tumors disappeared entirely, called a complete response. Two years after treatment, most people who had a complete response remained in remission. These benefits were seen mainly in people with two specific subtypes of B-cell lymphoma.
Researchers are also trying to make standard treatment regimens less toxic. In one study, NCI researchers found that the intensity of standard chemotherapy could be reduced in adults with lower risk Burkitt lymphoma, an aggressive type of non-Hodgkin lymphoma, without compromising the potential for a cure.
Immunotherapy
Immunotherapy uses substances to stimulate or suppress the immune system to help the body fight cancer. Several immunotherapies have shown promise in treating different types of lymphoma.
CAR T cells. CAR T cells are a type of immunotherapy in which a patient's T cells, a type of immune cell, are changed in the laboratory so they will better attack cancer cells. Four CAR T-cell therapies have been approved for the treatment of non-Hodgkin lymphoma:
- Axicabtagene ciloleucel (Yescarta) for people with large B-cell lymphoma or follicular lymphoma whose cancer has progressed after receiving one prior treatment regimen.
- Tisagenlecleucel (Kymriah) for adults with one of three types of non-Hodgkin lymphoma.
- Lisocabtagene maraleucel (Breyanzi) for people with some types of B-cell non-Hodgkin lymphoma that has relapsed or has not gotten better after at least two other treatments.
- Brexucabtagene autoleucel (Tecartus) for some people with mantle cell lymphoma that has come back or did not get better with other treatments.
To date, CAR T cells have provided long-term remissions for about one third of adults with aggressive lymphoma who receive them. Large randomized trials have been comparing CAR T-cell therapy to autologous stem cell transplantation at first relapse. In two of these trials, people who received the CAR T-cell therapy were less likely to have died or had a disease relapse after treatment compared with people who received chemotherapy followed by stem cell transplantation. Participants in one other trial are still being followed to see if differences in survival emerge over time.
Early results from a phase 2 trial tested CAR T cells as initial therapy in people at very high risk of relapse showed that over three-quarters of patients had their cancer go into remission. However, long term results are not yet available and CAR T cells are not FDA approved in this setting.
CAR T cells are also being tested in other lymphoma subtypes, both aggressive and indolent, as well as in patients with lymphoma that has spread to the central nervous system.
Immunomodulating drugs. Immunomodulators are drugs that either stimulate or suppress the immune system. One such drug, lenalidomide (Revlimid), has been approved in combination with targeted therapies for previously treated follicular lymphoma and marginal zone lymphoma. It is also often used to treat diffuse large B-cell lymphoma.
Novel immunotherapies. Researchers are also testing novel ways to stimulate the immune system to fight lymphoma. For example, in 2018, a small trial showed that combining radiation therapy with the injection of a compound that stimulates the immune system could shrink some indolent B-cell lymphomas.
Immunotherapy drugs called bispecific antibodies are also under development. These drugs bind to lymphoma cells and the body’s own immune cells at the same time to bring them together. This allows the immune cells to kill the lymphoma cells. Five bispecific antibodies are in clinical trials for various types of lymphoma, including:
- glofitamab (Columvi), which in a phase 1 trial shrank aggressive lymphoma in people who had received several prior treatments
- epcoritamab (Epkinly), which also shrank previously treated aggressive lymphoma in an early-phase clinical trial
- mosunetuzumab (Mosun), which triggered long-lasting remissions in almost 20% of people with aggressive B-cell non-Hodgkin lymphoma and almost 50% of people with indolent B-cell non-Hodgkin lymphoma in an early-phase clinical trial
Glofitamab, epcoritamab, and mosunetuzumab have all received accelerated approval from the FDA for the treatment of some lymphomas that have returned or gotten worse after at least two other treatments.
Hodgkin Lymphoma Treatment
Hodgkin lymphoma is much less common than non-Hodgkin lymphoma. It is mostly seen in early adulthood (age 20–39) and in late adulthood (age 65 and older). More than 75% of all adults newly diagnosed with Hodgkin lymphoma can be cured with standard chemotherapy, radiation therapy, or both. Over the last 5 decades, deaths from Hodgkin lymphoma among adults have fallen more rapidly than deaths from any other cancer type.
Researchers are now focusing on adjusting standard treatment regimens to reduce the long-term side effects and improve quality of life for survivors. They are also testing better ways to treat the minority of patients whose cancer does recur.
Targeted therapies
A protein called CD30 is commonly found on the surface of Hodgkin lymphoma cells. A drug called brentuximab vedotin (Adcetris) that targets this protein has been approved as part of initial treatment for people with advanced Hodgkin lymphoma. Use of this new drug may help older patients avoid what had been the standard treatment with an especially toxic chemotherapy drug.
Clinical trials are now testing brentuximab vedotin combined with other chemotherapy drugs and with immunotherapies. The drug has also been approved by the FDA in combination with chemotherapy for some children and adolescents with Hodgkin lymphoma.
Immunotherapy
Immune checkpoint inhibitors that help T cells to better kill cancer cells have been effective in some people with recurrent Hodgkin lymphoma. Two such drugs—nivolumab (Opdivo) and pembrolizumab (Keytruda)—have been approved for some patients with Hodgkin lymphoma that has recurred after previous treatments.
Researchers are now testing these drugs in combination with other therapies, as well as earlier in treatment for some people with cancer that is likely to recur. For example, a large clinical trial recently found a benefit to giving nivolumab as part of initial treatment to teens and adults with advanced forms of classic Hodgkin lymphoma. More than 90% of trial participants who received nivolumab plus chemotherapy and targeted therapy were alive without their cancer starting to grow again 2 years after treatment, compared with 83% of those who received chemotherapy and targeted therapy alone
NCI-Supported Research Programs
The Lymphoma Specialized Programs of Research Excellence (Lymphoma SPOREs) are designed to quickly move basic scientific findings into clinical settings. The Lymphoma SPOREs support the development of new immunotherapies, novel targeted therapies, and new methods for determining prognosis for individual patients.
The goal of the International Lymphoma Epidemiology Consortium (InterLymph) is to enhance collaboration among epidemiologists studying lymphoma, provide a forum for the exchange of research ideas, and create a framework for collaborating on analyses that compile data from multiple studies.
The Lymphoma Epidemiology of Outcomes (LEO) Cohort Study was established to address the current and long-term health needs of non-Hodgkin lymphoma patients and survivors. The goal is to support a broad research agenda aimed at identifying novel clinical, epidemiologic, host, genetic, tumor, and treatment factors that significantly influence non-Hodgkin lymphoma prognosis and survivorship.
The Cancer Genome Characterization Initiative (CGCI) is supporting research to identify common gene changes in adult and pediatric cancers. Its results are freely available to the wider cancer research community, to spur the development of new targeted drugs. The HIV+ Tumor Molecular Characterization Project (HTMCP) and Burkitt Lymphoma Genome Sequencing Project (BLGSP) are two active CGCI projects.
Within the Center for Cancer Research, the Lymphoid Malignancies Branch focuses on identifying abnormalities in the immune system and looking at molecular disorders that underlie lymphoid malignancies.
The Clinical Trial Sequencing Project (CTSP) promotes the use of genomics in NCI-supported clinical trials. CTSP’s goal is to clarify the molecular basis of response and resistance to therapies studied. Diffuse large B-cell lymphoma is one of the cancer types under study, along with breast and renal cell carcinoma.
Clinical Trials
NCI funds and oversees both early- and late-phase clinical trials to develop new treatments and improve patient care. Trials are available for lymphoma treatment.
Lymphoma Research Results
The following are some of NCI's latest news articles on lymphoma research:
- Nivolumab Appears to Boost Cure Rate in Advanced Hodgkin Lymphoma
- Combination Targeted Treatment Produces Lasting Remissions in People with Resistant Aggressive B-cell Lymphoma
- Cholesterol Drug May Help Protect the Heart during Chemotherapy for Lymphoma
- Three-Drug Regimen Improves Protection against GVHD after Stem Cell Transplant
- Trial Confirms CAR T-Cell Therapy Benefits People with Aggressive Lymphomas
- Brentuximab Approved for High-Risk Hodgkin Lymphoma in Children and Adolescents
View the full list of Lymphoma Research Results and Study Updates.