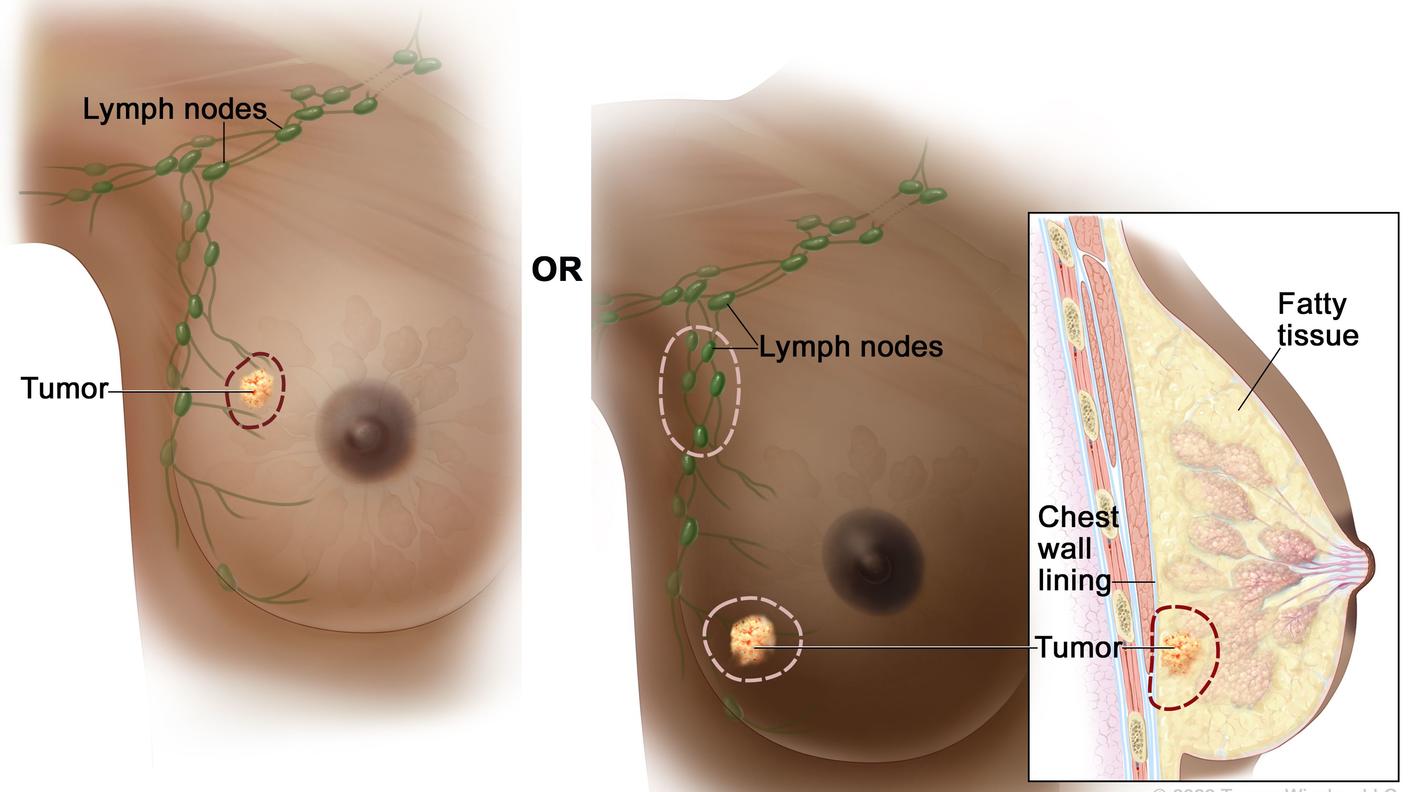
Can Some People with Breast Cancer Safely Skip Lymph Node Radiation?
, by Elia Ben-Ari
From more targeted drugs to less extensive surgery, doctors continue to refine how breast cancer is treated. Results of a clinical trial reported last month suggest that further fine-tuning may be possible—in this case, when it comes to treatment with radiation following surgery.
Specifically, the new findings suggest that some people who have undergone surgery (either lumpectomy or mastectomy) for breast cancer that has already spread to nearby lymph nodes can safely skip radiation therapy that’s targeted to those lymph nodes. In particular, the findings apply only to people who respond to chemotherapy given prior to surgery and no longer have signs of cancer in the lymph nodes at the time of surgery.
The type of radiation in question, known as regional nodal irradiation (RNI), aims to destroy cancer cells that remain in the lymph nodes and lower the chances that the cancer will come back or spread to other parts of the body. However, its use also can lead to side effects, including a potentially debilitating condition called lymphedema.
In the trial, there was no difference in the likelihood of cancer coming back, or recurring, between those who got RNI to the lymph nodes and those who didn't. Initial results of the NCI-supported clinical trial were presented in December 2023 at the San Antonio Breast Cancer Symposium.
Since then, “there’s been a lot of talk about this study in the oncology community,” said Abram Recht, M.D., a breast radiation oncologist at Beth Israel Deaconess Medical Center in Boston, who was not involved in the trial.
Some experts in treating breast cancer said the new findings should change the way some people with breast cancer are treated. But while some doctors plan to stop recommending RNI to certain patients based on the results presented in San Antonio, others, including Dr. Recht, say they want to see more data before changing treatment recommendations.
“This will be a very important study for our practice of radiation oncology,” Dr. Recht said. “[But] to me, it’s premature to change what we do and what we recommend to people” until more detailed results of the trial are available.
Having those details will help radiation oncologists make more informed recommendations for people with breast cancer that has spread to nearby lymph nodes, said Kilian Salerno, M.D., of NCI’s Radiation Oncology Branch, who also was not involved in the trial. Because, Dr. Salerno explained, there will be other aspects of their cancer—and its treatment—that also influence its likelihood of returning.
“[So] the benefit of adding a treatment like RNI to further lower the risk of recurrence will vary based on what that initial risk is,” she said. The bottom line: Decisions about radiation therapy will still need to be tailored to the individual.
Changing when chemo is given may change the need for radiation therapy
For people with early-stage breast cancer, doctors traditionally have recommended surgery to remove as much of the cancer as possible, followed by additional treatment with chemotherapy and radiation therapy to kill any cancer cells that remain in the body.
“The biggest danger of breast cancer is that it can spread through the bloodstream to other parts of the body before we even know about it,” Dr. Recht said.
And the lymph nodes are often the first way station in that spread.
If cancer is found in lymph nodes near the breast, radiation therapy that targets those lymph nodes has been shown to reduce the chances that the cancer will come back and improve how long people live, said Eleftherios (Terry) Mamounas, M.D., M.P.H., of the Orlando Health Cancer Institute in Orlando, Florida, who led the clinical trial and presented the results in San Antonio.
But in recent years, Dr. Mamounas said, it’s become more common to give people with breast cancer chemotherapy and sometimes hormone therapy before they have a lumpectomy or mastectomy. This is done to shrink the tumor, making it easier to remove.
And in some patients, this pre-surgery (neoadjuvant) chemotherapy eliminates the cancer in nearby lymph nodes, which is typically associated with a better outlook.
When this happens, doctors wondered, do patients still benefit from radiation therapy directed at the lymph nodes? Or should they be treated as if they did not have cancer in nearby lymph nodes in the first place, which would mean skipping RNI?
Design and results of the NSABP B-51 study
To answer this question, Dr. Mamounas and his colleagues designed the clinical trial known as NRG Oncology/NSABP B-51/RTOG 1304. The trial was run by the NCI-funded NRG Oncology clinical trials group.
Starting in 2013, the trial enrolled more than 1,600 people with invasive breast cancer that had spread only to lymph nodes under the arm (axillary lymph nodes) at the time of their diagnosis. The size of breast tumors ranged from less than 2 cm across to 5 cm or greater.
All study participants had received chemotherapy before surgery and their axillary lymph nodes were found to be cancer free at the time of surgery. Participants whose tumors were HER2-positive also received treatment with trastuzumab (Herceptin) or other HER2-targeted drugs along with chemotherapy.
Participants were randomly assigned to one of two treatment groups, RNI or no RNI. People who had a lumpectomy still received radiation to the whole breast, which is standard. Those in the RNI group who had a mastectomy received radiation to the chest wall in addition to RNI (see table below).
| Type of Surgery | RNI Group | No-RNI Group |
|---|---|---|
| Lumpectomy | Whole-breast radiation + RNI | Whole-breast radiation only |
| Mastectomy | Chest-wall radiation + RNI | No radiation |
Skipping RNI did not increase the risk of disease recurrence, Dr. Mamounas’s team found. After a median follow-up of almost 5 years, 92.7% of those who received RNI and 91.8% who didn’t receive it had not had a breast cancer recurrence 5 years after surgery.
The chances of dying 5 years after surgery, as well as other measures of how people fared, also did not differ between the two groups.
The side effects of radiation therapy were generally mild or moderate, with more people in the RNI group experiencing side effects, and none were unexpected. The rate of more severe side effects was also somewhat higher in the RNI group (10% versus 6.5%) and the most common severe effect was skin irritation from the radiation.
“Our findings suggest that we can customize radiation therapy … and potentially avoid RNI for patients with invasive breast cancer who respond well to chemotherapy and no longer have cancer in the lymph nodes” at the time of surgery, Dr. Mamounas said.
A benefit of skipping radiation to the lymph nodes is the potential to reduce the risk of certain side effects, Dr. Salerno said, including lymphedema and inflammation and scarring of lung tissue. Lymphedema is swelling that occurs when lymph fluid builds up in soft tissues along the arm.
Omitting RNI could also lessen the risk of complications in people who have breast reconstruction after a mastectomy, Dr. Mamounas said.
Dr. Mamounas believes the results will change how people like those in the study are treated, but “we are also being a little bit cautious,” he stressed.
Breast cancer sometimes comes back many years after initial treatment, especially with certain subtypes of breast cancer. So to see if any differences emerge between the two treatment groups, particularly in people with different subtypes, the team will continue to follow trial participants for an extended period.
“We plan to report 10-year data and 15-year data and hopefully we’ll solidify our findings,” Dr. Mamounas said.
More detailed information would help doctors tailor treatment
One key reason Dr. Recht believes it’s too soon to change standard treatment is that “in some ways, this was not really one trial but two separate trials with different designs.”
One involved people who had a lumpectomy and the other involved those who had a mastectomy. And while all participants who had a lumpectomy received some form of radiation (to the operated breast only in the no-RNI group), those in the no-RNI group who had a mastectomy did not receive any radiation at all.
In addition, although all participants had some lymph nodes removed and examined for signs of cancer at the time of breast surgery, the type of lymph node surgery differed between patients. Some had a more extensive procedure known as axillary lymph node dissection, while others had a more targeted sentinel lymph node biopsy.
Those differences are important, Dr. Salerno explained, because whether and to what extent RNI is likely to be beneficial may depend on the type and extent of the breast and lymph node surgeries.
Drs. Recht and Salerno said they would like to see the study results for the mastectomy and lumpectomy groups broken down by the kind of lymph node surgery patients had, as well as by tumor size and breast cancer subtype (for example, whether the cancer is hormone receptor–positive or negative).
With this more detailed information, doctors will be able to make recommendations about RNI that are more tailored to the individual patient.
In addition, Dr. Salerno emphasized, RNI following surgery continues to be the standard treatment for anyone who still has cancer in the lymph nodes near the breast following pre-surgery chemotherapy or other systemic therapy.
Even after more detailed information from the trial is available, treatment recommendations might still differ from one radiation oncologist to another, Dr. Recht said. But “our job as physicians is to wait until we have the information we need about who is and isn’t likely to benefit from skipping RNI before making those decisions.”