New Therapy Benefits Patients with Neuroendocrine Tumors
, by NCI Staff
Results from a clinical trial suggest that a targeted drug that’s linked to a radioactive isotope to help kill tumor cells may soon be a new treatment option for some patients with advanced neuroendocrine tumors (NETs).
Patients in the phase III trial had tumors that were progressing despite treatment with standard first-line therapies. Those who were treated with the new drug, 177Lu-Dotatate, lived substantially longer without their cancer progressing than patients who received high doses of octreotide LAR (Sandostatin® LAR Depot).
The findings also suggest that the drug may improve how long patients live overall. But longer follow up is needed before it’s clear whether that’s the case, said the trial’s lead investigator, Jonathan Strosberg, M.D., of the Moffitt Cancer Center in Tampa, FL.
The results were published January 12 in the New England Journal of Medicine (NEJM).
Trial participants had advanced NETs that originated in the middle portion of their gastrointestinal tract, known as midgut NETs. Few treatments have proven to be effective in patients with midgut NETs that have stopped responding to standard therapies, Dr. Strosberg said.
Particularly given the limited side effects seen in the trial, the trial results are "very encouraging," he continued.
Based on earlier data from the trial and smaller trials conducted primarily in Europe, 177Lu-Dotatate is currently being reviewed by the Food and Drug Administration (FDA) for the treatment of patients with midgut NETs as well as those with NETs in several other parts of the gastrointestinal tract.
Targeting and Killing NET Cells
NETs originate in neuroendocrine cells, which largely resemble nerve cells but behave like endocrine, or hormone-producing, cells. Neuroendocrine cells play important physiologic functions in the lungs and gastrointestinal tract.
Although at least 40 different types of NETs have been identified, including benign forms, these tumors are relatively rare. They also are infamous for their diverse, or heterogeneous, behavior, even among those that form in the same anatomical location.
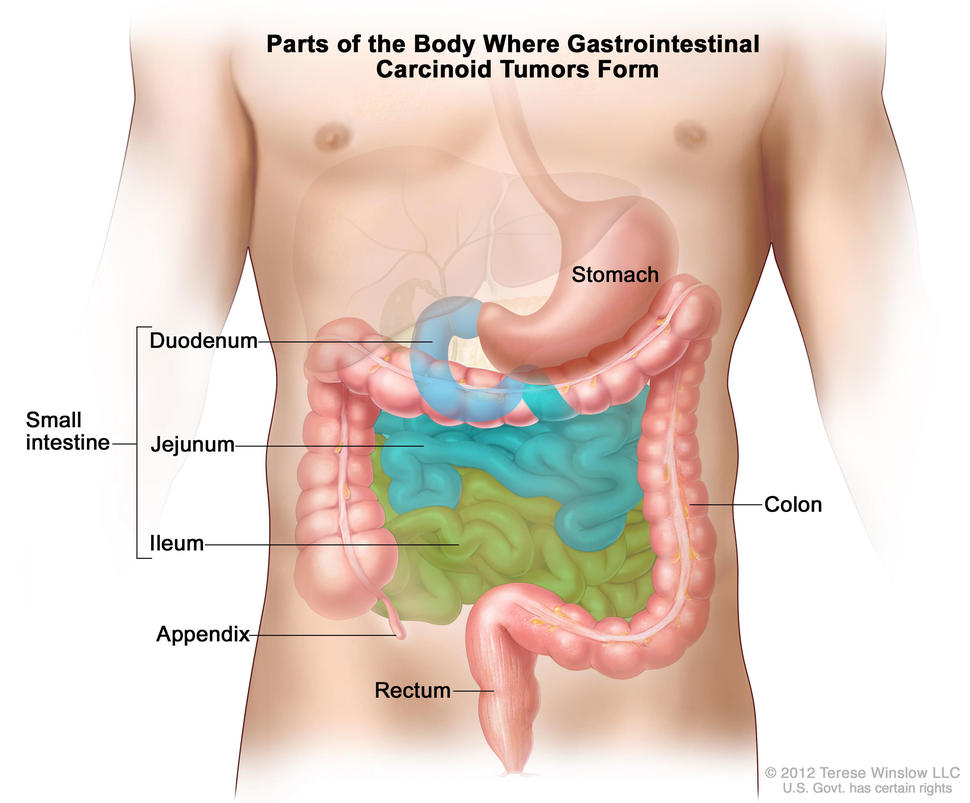
NETs that form in the midgut—typically defined as the area from the middle portion of the small intestine (jejunum) to the initial portion of the colon (ascending colon)—are the most common cancerous NET. Patients who develop metastatic midgut NETs have a poor prognosis, with only about half surviving for 5 years or longer.
Most current therapies for NETs take advantage of the fact that these tumors overexpress receptors for a hormone called somatostatin. When somatostatin binds to these receptors, it blocks the cells from releasing excessive amounts of some other hormones, such as serotonin and growth hormones.
Among other problems, NETs can release large amounts of hormones into the blood, causing numerous problems such as diarrhea and flushing—a condition known as carcinoid syndrome.
Somatostatin itself only lingers in the circulation for a few hours. So different formulations, or analogues, of somatostatin that can remain viable in the circulation for longer have become the bedrock of NET treatment.
The currently FDA-approved somatostatin analogues, however, such as octreotide LAR, primarily only stabilize tumors and delay their growth rather than shrink them, Dr. Strosberg explained.
177Lu-Dotatate is different from other somatostatin analogues used to treat NETs in an important way: it incorporates a radioactive isotope.
The somatostatin analogue component of the drug is octreotate, which has a stronger affinity than other somatostatin analogues for a key receptor on NET cells, Dr. Strosberg said. The radioactive isotope to which it’s linked is 177lutetium.
Dual-component somatostatin analogues are not new. They are also being tested as imaging agents to locate tumors using PET scans, and at least one has been approved by the FDA this purpose.
In the case of 177Lu-Dotatate, however, the radioactive isotope plays a therapeutic role: once delivered to tumor tissue, Dr. Strosberg explained, the drug has a much more substantial cell-killing, or cytotoxic, effect than traditional somatostatin analogues.
Improved Tumor Response, Survival
The trial randomly assigned 229 patients with metastatic midgut NETs that were progressing on a somatostatin analogue to receive either 177Lu-Dotatate or high-dose octreotide LAR.
Patients who received 177Lu-Dotatate also received a standard dose of octreotide to help control symptoms. High-dose octreotide LAR is not considered to be a standard of care in this patient population, Dr. Strosberg noted. But because it’s often used in the clinic in this fashion, the trial investigators and regulatory authorities felt that it was a “reasonable choice” for use in the control group, he explained.
The trial, called NETTER-1, was funded by the drug's manufacturer, the French company Advanced Accelerator Applications, and was conducted primarily at hospitals in the United States and Europe.
At 20 months after initiating treatment, approximately 65% of patients in the 177Lu-Dotatate group and only 11% in the control group had not experienced disease progression. Overall, 18% of patients in the 177Lu-Dotatate group experienced significant tumor shrinkage, compared with only 3% in the octreotide LAR group.
Historically, tumor responses in these patients are uncommon. So the double-digit tumor response rates seen in this trial "are very high," he said.
There were nearly twice as many deaths among patients in the high-dose octreotide LAR group as the 177Lu-Dotatate group: 26 versus 14. The available data suggest that 177Lu-Dotatate "probably does have an effect on [overall] survival," Dr. Strosberg said. "Hopefully for patients, that will be borne out in the final analysis."
Given the heterogeneous nature of NETs, it was important to have a phase III trial of this therapy strictly in patients with midgut NETs, said Electron Kebebew, M.D., chief of the Endocrine Oncology Branch in NCI's Center for Cancer Research.
"The study findings are significant, and it provides a new alternative treatment" for patients with advanced disease, he said.
But Dr. Kebebew cautioned that more data are needed to better understand who is most likely to benefit from treatment with 177Lu-Dotatate. Patients were eligible to participate in the trial if their disease had progressed within 3 years after their treatment began, he noted.
Including patients with a relatively long interval to cancer progression could have skewed the progression-free or overall survival data relative to what has been seen in trials testing other therapies, Dr. Kebebew said.
Side Effects Limited So Far
Somatostatin analogues linked to radioactive isotopes can cause serious kidney problems but, to date at least, there has been no evidence of this problem in the NETTER-1 trial.
Although more patients who received 177Lu-Dotatate experienced side effects, severe toxic effects were limited and manageable, Dr. Strosberg explained.
It will be important to monitor patients long-term, Dr. Kebebew said, because "we have seen patients have progressively declining renal function" after treatment with these agents.
The most common problem linked to the treatment in the trial was nausea and vomiting. But these problems were usually not caused by 177Lu-Dotatate, but rather by the accompanying infusion of a cocktail of approximately 20 amino acids to help prevent any kidney damage, Dr. Strosberg said.
Outside of the trial, patients treated in Europe—where 177Lu-Dotatate was developed and has been widely studied—typically receive infusions of only two amino acids along with the drug and experience much less nausea, he continued.
In June 2016, the FDA granted priority review for the New Drug Application submitted by Advanced Accelerator Applications for 177Lu-Dotatate, meaning it would expedite its review process.
But late last year, the agency requested revisions to how the data to support the application were presented and additional data on the drug's safety and its effects in different patient subgroups, which has delayed its decision on whether to approve the drug.