New Mouse Model Closely Mimics Most Common Leukemia in Infants
, by NCI Staff
Researchers have created a long-sought-after mouse model for the most common form of infant leukemia, an aggressive form of acute lymphoblastic leukemia (ALL) for which prognosis is poor. The model closely mimics how this cancer arises and progresses in humans.
The overall cure rate of childhood B-cell ALL has improved dramatically in recent decades. But this same success has not extended to children under age 1 with the most common type of infant leukemia, an aggressive ALL subtype known as t(4;11) pro-B ALL or MLL-AF4 leukemia. About two-thirds of infants diagnosed with this leukemia subtype relapse or die within 5 years.
For nearly two decades, researchers have been trying to develop a mouse model of this ALL subtype that closely reflects the human disease. This goal may finally have been achieved, reported a research team led by Michael Thirman, M.D., of the University of Chicago, and James Mulloy, Ph.D., of Cincinnati Children’s Hospital Medical Center, November 14 in Cancer Cell.
The new model “provides a giant step forward,” Nancy Zeleznik-Le, Ph.D., of Loyola University Chicago, wrote in an accompanying editorial on the study. In particular, she continued, having an animal model that closely resembles the human disease “may be particularly valuable for studies of therapies directed at this…leukemia with an unfavorable prognosis.”
Overcoming Technical Challenges
In B-cell ALL, the bone marrow makes too many immature B lymphocytes, a type of white blood cell. In patients with the pro-B, or early pre-B, subtype of B-cell ALL, these dysfunctional cells (leukemia cells) are at a very early stage of B-cell development. The leukemia cells eventually crowd out healthy cells in the bone marrow and blood.
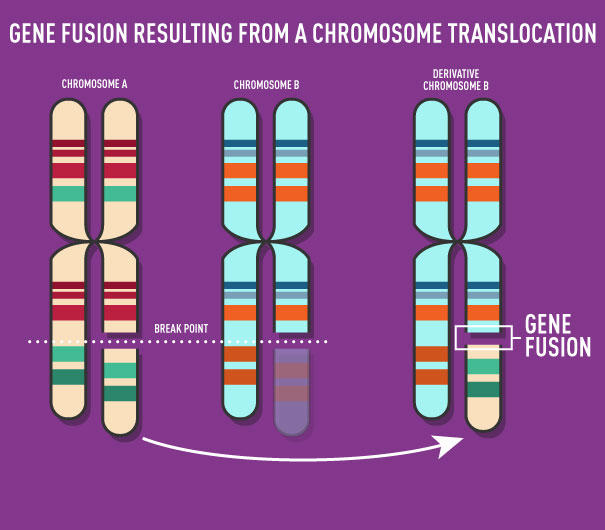
The MLL-AF4 subtype of B-cell ALL results from the joining, or fusion, of parts of two separate genes: the MLL gene from chromosome 11 and a gene known as AF4 from chromosome 4. The resulting MLL-AF4 fusion protein is a transcription factor that alters the expression of numerous genes in affected cells.
Leukemias with MLL gene fusions account for about 70% of infant ALL cases and about 6% of ALL cases in older children, and the MLL-AF4 fusion is found in about half of MLL gene fusion cases for both infants and older children with ALL. Infants and older children whose leukemia cells carry MLL fusions have a poor prognosis.
To create the new model of MLL-AF4 leukemia, the researchers had to overcome two key challenges. Their initial attempts to use a type of virus called a retrovirus to transfer the human MLL-AF4 fusion gene into the genome of mouse cells failed because the retrovirus carrying the fusion gene did not replicate well. But when the researchers replaced the human AF4 gene fragment with the slightly different mouse version, Af4, the levels of virus increased 30-fold.
The researchers then put the retrovirus carrying the MLL-Af4 human–mouse fusion gene into blood-forming stem cells from mice and transplanted those cells into laboratory mice. That led to challenge number two: The mice with the transplanted cells developed acute myeloid leukemia, instead of ALL.
To overcome this second challenge, the team tried transferring the retrovirus carrying the MLL-Af4 gene into blood-forming stem cells from humans, instead of into mouse stem cells. The researchers transplanted them into a strain of mouse with a deficient immune system, which permits the growth of human cells that would otherwise be rejected by the mice.
That approach was successful. By 22 weeks after transplant of human stem cells carrying the MLL-Af4 gene, the mice developed leukemia with “hallmarks of classic t(4:11) pro-B ALL,” the authors wrote. These hallmarks included an enlarged spleen, infiltration of leukemia cells into multiple organs, and the presence of specific types of immature B cells in the bone marrow and bloodstream.
All Fusion Partners Not Alike
To further assess whether the leukemia that the mice developed is similar to the human disease, the team compared several molecular features of leukemia cells from the mice with those of leukemia cells from patients with the MLL-AF4 fusion.
These experiments showed that the mouse model closely mirrors molecular aspects of the disease in humans, including the ability of the fusion protein to associate with certain proteins critical for altered gene expression and for leukemia development, targeting of the fusion protein to specific chromosome regions, and distinct gene expression patterns.
The study also provided some possible new glimpses into the human disease.
For example, the MLL gene can have about 80 different gene partners in the MLL fusion leukemias. And it’s not entirely clear whether all leukemias induced by MLL fusions are identical.
To examine this question, the study authors did a comparative analysis of mice with B-cell ALL induced by MLL-Af4 or by a fusion protein encoded by the same MLL gene fragment but fused to a fragment of another gene, AF9. The specific changes in gene expression seen with one MLL fusion partner were different from those seen with another partner, they found, indicating that leukemias induced by MLL fusions to different gene fragments are indeed different.
This is an important insight, the researchers believe.
“Although different MLL-fusion proteins share some common properties, each has its own genetic and biological features associated with particular fusion partner proteins,” they wrote. “These differences could potentially impact response to therapy and highlight the need for models specific to each fusion.”