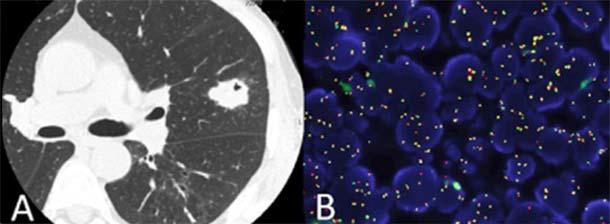
FDA Approves Alectinib for ALK-Positive Non-Small Cell Lung Cancer
, by NCI Staff
The Food and Drug Administration (FDA) approved alectinib (Alecensa®) on December 11, 2015, for some patients with metastatic non-small cell lung cancer (NSCLC) with mutations in the ALK gene.
The agency granted an accelerated approval for alectinib for patients whose cancer is no longer responding to the ALK-targeted agent crizotinib (Xalkori®) or who are unable to tolerate further treatment with crizotinib because of side effects.
Tumors in up to 7 percent of patients with NSCLC have rearrangements in the ALK gene—the fusion of a portion of ALK with a portion of another gene. Alectinib is now the third ALK-targeted drug approved by the FDA. The agency approved ceritinib (Zykadia™) in 2014 for patients with NSCLC who have progressed on crizotinib.
Although tumor responses are seen in about 60 percent of patients with ALK-positive NSCLC who receive crizotinib, more than half also experience gastrointestinal side effects, particularly diarrhea, nausea, vomiting, and constipation, said Anish Thomas, M.D., of the Thoracic and Gastrointestinal Oncology Branch in NCI’s Center for Cancer Research. Patients appear to tolerate alectinib better than crizotinib, with fewer patients needing dose reduction, interruption, or withdrawal to manage side effects, Dr. Thomas said.
Alectinib does have side effects, including fatigue, edema, constipation, and muscle pain, Dr. Thomas noted. “But the gastrointestinal side effects are much less than those associated with crizotinib,” he said. “For patients with ALK-positive NSCLC who are not able to tolerate crizotinib, the approval of alectinib is encouraging.”
The approval of alectinib was based on the results of two small single-arm clinical trials of patients with ALK-positive NSCLC who were previously treated with crizotinib. In the first trial, tumor reductions were observed in 38 percent of patients, with median survival of 7.5 months. In the second trial, tumor reductions were observed in 44 percent of patients, with median survival of 11.2 months.
In both trials, treatment with alectinib also had an effect on tumors that had spread to the brain. Collectively, 61 percent of patients in the trials who had brain metastases had partial or complete reductions in the tumors that lasted a median of 9.1 months.
Like ceritinib, alectinib is a second-generation ALK inhibitor. But, Dr. Thomas cautioned, direct comparisons between the two drugs are limited.
Alectinib’s ability to shrink brain metastases “is an important effect for clinicians to understand,” said Richard Pazdur, M.D., director of the Office of Hematology and Oncology Products in the FDA’s Center for Drug Evaluation and Research, in a news release on the approval.
Although alectinib has several advantages over crizotinib and ceritinib, based on studies conducted so far, it is approved only for patients who have progressed on or who do not tolerate crizotinib, Dr. Thomas stressed. A clinical trial that is comparing alectinib and crizotinib head-to-head is ongoing.
“The field of ALK-positive NSCLC is rapidly evolving,” Dr. Thomas concluded. “A number of novel agents targeting specific resistance mechanisms are in clinical trials. Hopefully, in the not too distant future, we will be able to routinely perform molecular profiling of tumors that become resistant to initial treatment with an ALK inhibitor to help us specifically select second- and third-line treatments.”