Prescription Subsidies Reduce Breast Cancer Treatment Disparities
, by NCI Staff
Subsidies for prescription drugs can increase the use of hormone therapies among women with early-stage breast cancer, according to the results of a new study. The subsidies may also help to decrease racial/ethnic disparities in the use of these medications, the study found.
According to the study authors, the findings suggest that, by improving the likelihood that patients will follow the prescribed treatment (adherence) and continue the treatment for the duration prescribed (persistence) for these adjuvant therapies, prescription subsidies could help reduce the risk of cancer returning in a sizable portion of women.
The study results were reported October 24 in the Journal of Clinical Oncology.
“The study findings add to the research showing that costs matter in cancer care,” said the study’s lead author, Alana Biggers, M.D., M.P.H., of the University of Illinois-Chicago. “Subsidies based on economic status can benefit all women and, by lowering out-of-pocket costs, can improve the likelihood that women and, in particular, nonwhite women, will continue their medications and improve breast cancer outcomes.”
Adjuvant hormone therapy reduces the risk of cancer recurrence and death among women with early-stage hormone receptor-positive breast cancer. But according to the most recent data, more than one-third of patients do not complete their full course of adjuvant treatment.
Historically, black women and women with low socioeconomic status have poorer outcomes and higher breast cancer mortality rates than women from other racial/ethnic and socioeconomic groups. These disparities have been attributed, at least in part, to these women having less access to quality medical care, resulting in later detection and lower-quality adjuvant treatment. These populations also have low rates of adherence and persistence to adjuvant therapy. Little is known, however, about adherence or persistence to adjuvant therapy among Hispanic women.
“If women diagnosed with breast cancer do not complete their therapies, they are at a higher risk for recurrence, so it is important to examine the barriers they face in completing treatments,” said Dr. Biggers. “We wanted to examine how a subsidy influences the medication adherence and persistence practices of women with early-stage breast cancer.”
To do so, Dr. Biggers and her colleagues examined Medicare data for more than 25,000 women aged 65 years and older who had surgery for early-stage breast cancer between 2006 and 2007 and at least one prescription filled for oral adjuvant hormone therapy.
In the population sample studied, the majority of Hispanic and black women (77% and 70%, respectively) received financial assistance via the Medicare Part D Low-Income Subsidy program (also known as Extra Help), a federal program that provides full or partial coverage for out-of-pocket medication costs to people with limited financial resources. Among white women in the sample, only 21% received the subsidy.
The researchers found that the rates of adherence and persistence were higher among blacks and Hispanic women overall. However, upon further analysis, the researchers determined that this finding was largely due to the majority of Hispanic and black women receiving subsidies.
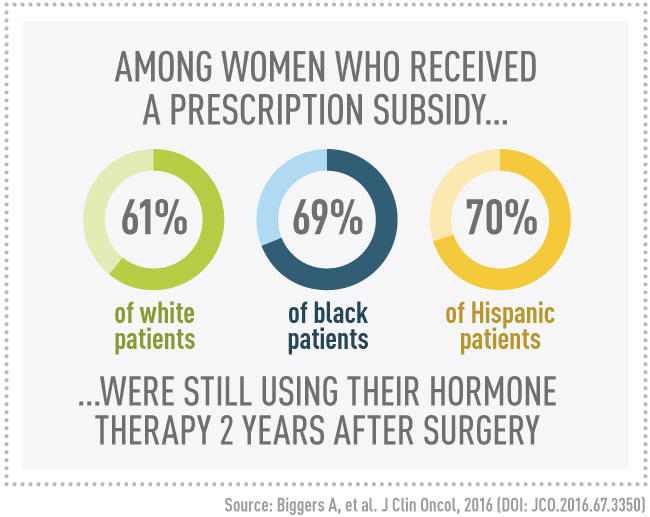
When the data were stratified by who received the subsidy and who did not, it was clear that subsidies were associated with increased adherence and persistence rates among all three racial/ethnic groups. Among the unsubsidized women, black and Hispanic women had lower rates of adherence and persistence to hormonal therapy. But, among the women who received the subsidy, blacks and Hispanics had rates of taking medications and continuing hormonal therapy treatments equal to or better than whites. Two years after their surgery, 69% of black and 70% of Hispanic patients were continuing their treatment, compared with 61% of white patients.
The findings are consistent with earlier studies that have shown that subsidies can help to reduce patients’ out-of-pocket costs for both cancer and noncancer medications, and subsequent adherence and persistence, Dr. Biggers said.
In a previous study of women with breast cancer, for example, her team found large discrepancies in persistence and adherence to an aromatase inhibitor prescribed as adjuvant treatment for women whose costs were unsubsidized (90-day median out-of-pocket costs ranging from $106 to $183) and those whose costs were subsidized (90-day median out-of-pocket costs less than $10).
Other studies have demonstrated similar patterns of an association of high out-of-pocket costs with reduced treatment adherence and persistence. In some cases, patients with high out-of-pocket costs reported delaying or even stopping their prescribed medication.
“This research has important implications for understanding factors that may boost treatment persistence and improve cancer outcomes for women with breast cancer,” said Joanne Elena, Ph.D., M.P.H., of NCI’s Division of Cancer Control and Population Sciences.
“These kinds of studies are useful because they demonstrate the effect of policies that are designed to ensure that all women can continue their prescribed medications, with the ultimate goal of reducing disparities in cancer outcomes,” she said.