New Class of Compounds Rewires Cancer Cells to Self-Destruct
, by Nadia Jaber
Researchers have designed a molecule that kills blood cancer cells by tricking them into self-destructing, according to results of a new study. Experts say the molecule represents a new class of compounds that could have broad potential as cancer treatments.
Like a cyanide pill hidden in the teeth of a James Bond villain, human cells have a quick means of self-destruction if necessary. This natural safeguard is a way for the body to rid itself of old, damaged, or infected cells—including cancer cells.
But in many types of cancer, those means of self-destruction are subverted or blocked off. In some diffuse large B-cell lymphoma (DLBCL) tumors, for example, genes that orchestrate cell death are shut off by a protein called BCL6.
For the research team, the question was: “Can we turn something that is good for the cancer into something that will kill [it]?” said Nathanael Gray, Ph.D., of Stanford University, who led the new study along with Gerald Crabtree, Ph.D., also of Stanford University.
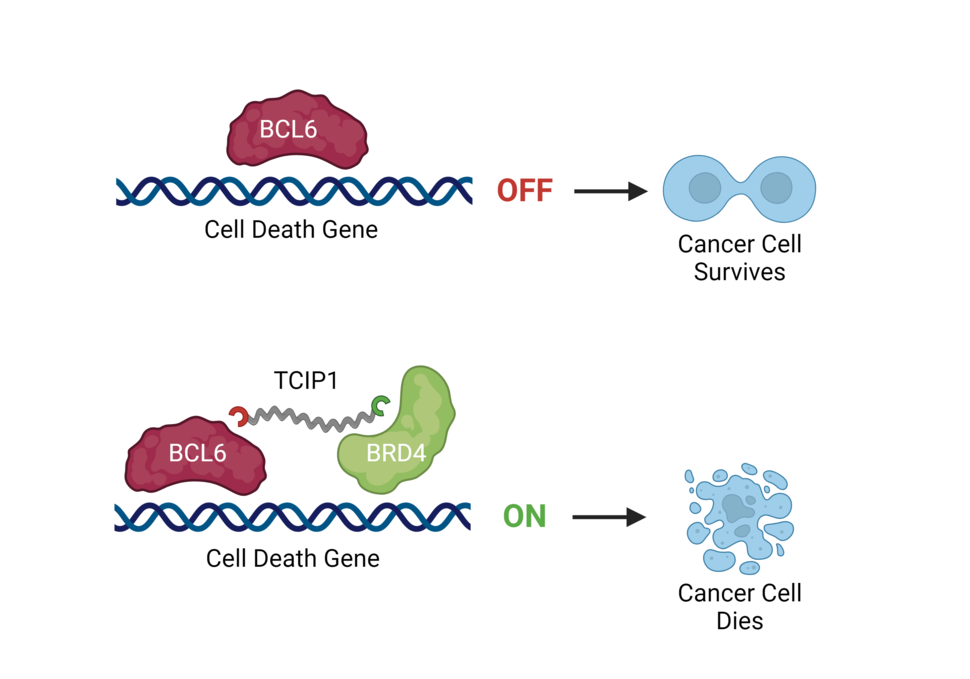
To do that, the researchers created a molecule that acts like a bungee cord, hooking onto BCL6 at one end and to another protein that turns genes on at the other end. Because of this connection, when BCL6 gets near genes that control cell death, the genes are turned up instead of getting shut off.
The molecule quickly triggered cell death in DLBCL cells in lab dishes and didn’t appear to cause any serious side effects in healthy mice, the NCI-funded study showed. The findings were published July 26 in Nature.
“There's still a substantial need for new therapies [for DLBCL],” said Louis Staudt, M.D., Ph.D., chief of NCI’s Lymphoid Malignancies Branch, who wasn’t involved in the research. In particular, he added, there is a need for targeted therapies that are likely to be less toxic than the standard chemotherapy.
Given the promising study results, “I think [the researchers] should vigorously pursue the development of this molecule and related molecules,” Dr. Staudt said.
The distance between us
Like a bungee cord connecting two objects, compounds called “chemical inducers of proximity” squeeze two proteins close together to achieve a biological effect. For example, some compounds bring immune and cancer cells in close proximity.
The new class of compounds developed by Dr. Gray and his colleagues bring together proteins, called transcription factors, that turn genes on or off. So, they dubbed the new compounds transcriptional chemical inducers of proximity (TCIPs).
The molecule tested in the new study, called TCIP1, hooks onto the transcription factors BCL6 and BRD4. The trick is that TCIP1 binds to BCL6 in a way that allows it to grab onto genes but not repress them. Once BCL6 gets near a gene, BRD4 swoops in and activates it.
A handful of companies are developing drugs that block BCL6 activity, mainly by degrading the protein, Dr. Staudt noted. “But this [new approach] does something completely unique; it's not just getting rid of BCL6 [activity],” he said.
TCIP1 prompts an activity “in the cell that didn’t exist before. It’s creating an artificial, new activity through the induced proximity” of BCL6 and BRD4, Dr. Gray explained.
TCIP1 kills lymphoma cells in lab experiments
In experiments involving cells growing in lab dishes, the molecule quickly killed several kinds of DLBCL cells with high levels of BCL6, but it had no effect on DLBCL cells that lacked BCL6.
Additional experiments showed that TCIP1 did exactly what the researchers had hoped: It pulled BRD4 to cell death genes that are normally shut off by BCL6, leading to the activation of those genes.
And it was incredibly potent, meaning that only a small amount of TCIP1 was needed to kill lymphoma cells. In fact, TCIP1 killed lymphoma cells at concentrations that are a thousand times lower than the active concentrations of most drugs used in cell experiments.
The research team hopes TCIP1 or another molecule like it can eventually help people with DLBCL. But several more years of laboratory studies are needed before a clinical trial could get started, Dr. Gray emphasized.
Side effects of TCIP1 in mice
BCL6 is only found in certain kinds of immune cells, and therapies that target BCL6 could pose potential health problems, said Dr. Staudt, whose early research helped identify BCL6 and define its role.
In healthy B cells, BCL6 staves off cell death while the cells undergo the complicated process of making new antibodies—such as when a person gets a new infection or a vaccine.
Like other treatments for DLBCL, there is a good chance that TCIP1 could wipe out healthy B cells and heighten the risk of deadly infections, Dr. Staudt said. But “we limit the damage” to healthy B cells by giving DLBCL treatments for short periods of time, he noted.
BCL6 also reins in genes that cause inflammation. When Dr. Staudt and others created mice lacking the BCL6 gene, the mice died of an inflammatory disease, he explained.
But when the Stanford researchers gave TCIP1 to healthy mice for 5 days, there were no noticeable side effects.
Although there was no evidence of inflammation in the mice, future “clinical trials of TCIP1 or related molecules should watch out for possible inflammatory side effects,” wrote Dr. Staudt and James Phelan, M.D., also of NCI’s Lymphoid Malignancies Branch, in an accompanying editorial on the new study.
Dr. Gray added that, because TCIP1 prompts cells to do something entirely new, “likely there will be surprises” when it comes to side effects.
Targeting other transcription factors
Scientists have long struggled to find drugs that block transcription factors, which typically lack “pockets” where a drug could squeeze into, Dr. Gray explained.
TCIPs could be a plausible approach for targeting other repressive transcription factors that drive cancer growth and survival, he said.
For instance, many childhood cancers are driven by abnormal transcription factors, Dr. Staudt pointed out.
“The hope is that this TCIP approach can work on other transcription factors, and we’re busy trying to do that now,” Dr. Gray said. More specifically, the researchers are working on designing TCIPs that tether abnormal transcription factors to other proteins that trigger cell death.
“There are definitely opportunities” to apply this approach more broadly, Dr. Staudt said. “It's up to the creativity of cancer biologists to find those opportunities.”