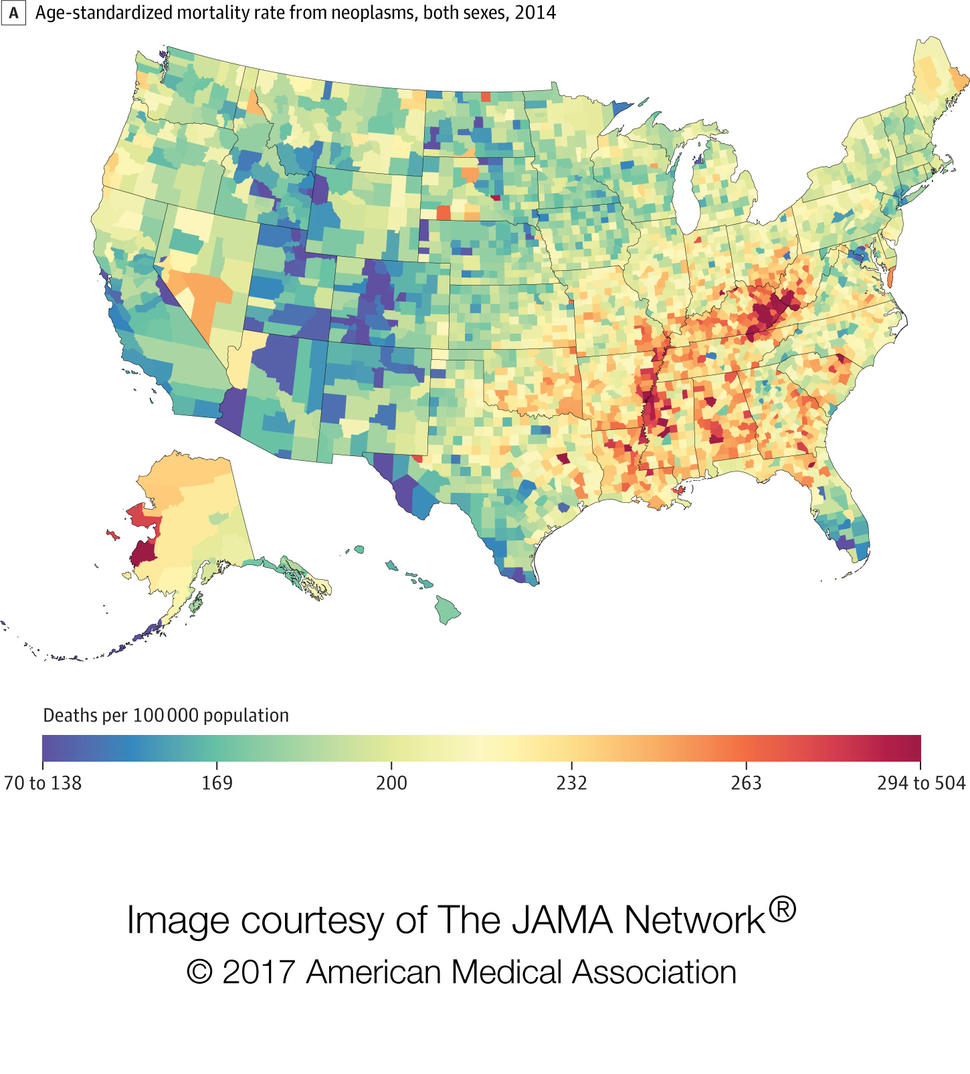
U.S. Cancer Mortality Rates Falling, But Some Regions Left Behind, Study Finds
, by NCI Staff
Rates of death from cancer in the United States dropped by 20% between 1980 and 2014, according to new research from the Institute for Health Metrics and Evaluation at the University of Washington.
However, these gains were not distributed equally across the country. In 160 of the United States' approximately 3,000 counties, cancer mortality rose substantially during the same time period.
The disparities in mortality between some counties were stark, the researchers found. In 2014, for example, the county with the highest overall cancer mortality had about 7 times as many cancer deaths per 100,000 residents as the county with the lowest overall cancer mortality.
Although disparities in cancer incidence and mortality have been well documented, Ali Mokdad, Ph.D., who led the study, said that the magnitude of the disparities seen in this study "was a surprise."
The findings were published January 24 in JAMA.
Cracks in the System
To conduct the study, Dr. Mokdad and his colleagues analyzed data on deaths from 29 cancer types recorded by the National Center for Health Statistics (NCHS) of the Centers for Disease Control and Prevention and compared the data to population counts collected from the Census Bureau, the NCHS, and the Human Mortality Database.
Previous studies had looked at variations in mortality at the state level, but none examined the differences at the county level. These granular differences matter, explained Dr. Mokdad, since public health interventions are ultimately designed and delivered locally.
Overall, the researchers found that U.S. cancer mortality rates dropped from about 240 cancer deaths per 100,000 people in 1980 to 192 per 100,000 in 2014.
However, disparities in mortality at the county level actually widened during the same period. In 1980, the lowest county-level mortality rate was about 130 per 100,000 and the highest was about 380 per 100,000. In 2014, the county with the lowest overall cancer mortality saw about 70 deaths from cancer per 100,000 people, and the county with the highest mortality had more than 500 deaths per 100,000 residents.
Clusters of high mortality were found in many states, including Kentucky, West Virginia, Alabama, and Alaska.
Four main factors drive these disparities, explained Dr. Mokdad. One is socioeconomic status; people with higher income and education levels are more likely to seek medical advice and have the means to do so, he said. The second is access to health care; many people in the United States lack health insurance or are underinsured, with plans that don’t cover some preventive care.
The third, he added, is the quality of health care available: whether patients are seen and treated promptly and followed appropriately after treatment. The fourth is the prevalence of risk factors, such as smoking, obesity, and lack of physical activity, which differ widely across the country.
County-level variations in these factors reflected trends the researchers saw in mortality from individual cancer types.
Dr. Mokdad, for example, pointed to what the researchers saw when they mapped county-level death rates from lung cancer against county-level smoking rates. "Where there is high smoking, there is high lung cancer," he said.
Other disparities—such as one the researchers found in deaths from testicular cancer— are more likely due to systemic problems within the health care system, he continued.
"The survival rate for testicular cancer is over 95%, so theoretically, almost nobody should die from it," Dr. Mokdad said. "When you see people are dying, then you know there are [issues of] access to and quality of health care."
Going Too Small?
Analyzing cancer mortality on a more granular level is important, said Eric Durbin, Dr.P.H., director of Cancer Informatics for the Kentucky Cancer Registry at the University of Kentucky Markey Cancer Center.
"We really have no other way to guide cancer prevention and control activities other than using [that] data," Dr. Durbin said. "Otherwise, you're just throwing money or resources at a problem without any way to measure the impact."
Having regional data on outcomes like cancer mortality can help researchers develop and test interventions, he continued.
"And then we can measure the success or failure of those interventions based on the data. If they’re successful, we should see shifts in incidence and mortality," he said.
However, Dr. Durbin recommended exercising extreme caution when basing any assumptions about changes in mortality on data at the county level, especially rural, sparsely populated counties.
He cited the example of Owsley County, Kentucky, which was highlighted in the paper as having the highest increase in mortality rates from lung cancer between 1980 and 2014 and the highest rate for women in 2014. Owsley County has the second smallest population in Kentucky, explained Dr. Durbin, making year-to-year measurements of cancer mortality "very unstable."
From 2000 to 2005, he noted, there was a 214% increase in cancer mortality in Owsley County, "which sounds horrific. But when you realize that this county has a relatively small population and relatively few cancer cases per year—no more than six to ten or so—just a few additional cases per year can result in these seemingly dramatic swings in mortality. Likewise, the greater than 200% reduction in lung cancer mortality observed in Owsley County from 2005 to 2011 was not so remarkable."
Because of this limitation in gathering accurate data at the county level, data-driven cancer control efforts in Kentucky are organized—and measured—by regions called Area Development Districts, explained Dr. Durbin. These groups of about 5 to 10 adjacent counties with similar geography and risk factors have proven small enough to allow for personalized interventions but large enough to provide stable data on cancer incidence and mortality.
For example, starting in 2002, Kentucky targeted public health interventions in these districts to improve their colorectal cancer screening rates, which went from second-worst in the country to 20th from the top, he said.
"What was really cool about this was that shortly after the intervention started, our state immediately saw our [colorectal cancer] incidence rates begin to drop. They've dropped almost every single year since then, and mortality has dropped as well," he added.
"You can't change anything in public health unless you are able to measure it and able to monitor it," said Dr. Mokdad. "We wanted counties to know their 'number,' and to empower public-health professionals to take action."