Neratinib Approved by FDA for HER2-Positive Breast Cancer
, by NCI Staff
On July 17, the Food and Drug Administration (FDA) approved neratinib (Nerlynx™) to prevent recurrence in patients with early-stage HER2-positive breast cancer who have finished at least 1 year of post-surgery trastuzumab (Herceptin®) therapy.
In the international randomized clinical trial that led to the approval, about 94% of patients who received 1 year of adjuvant neratinib were alive without their disease returning, compared with just under 92% of women who received a placebo.
Trial participants who received neratinib were more likely to experience severe diarrhea than those who received the placebo. Diarrhea led to a dose reduction of neratinib among 26% of patients, and 17% of patients receiving neratinib discontinued the drug early.
Despite the approval, several factors—the modest reduction in the recurrence rate, the fact that data on overall survival are not yet available, and the high rate of side effects—mean that neratinib is unlikely to be widely used by these patients, explained Alexandra Zimmer, M.D., of the Women’s Malignancies Branch in NCI’s Center for Cancer Research.
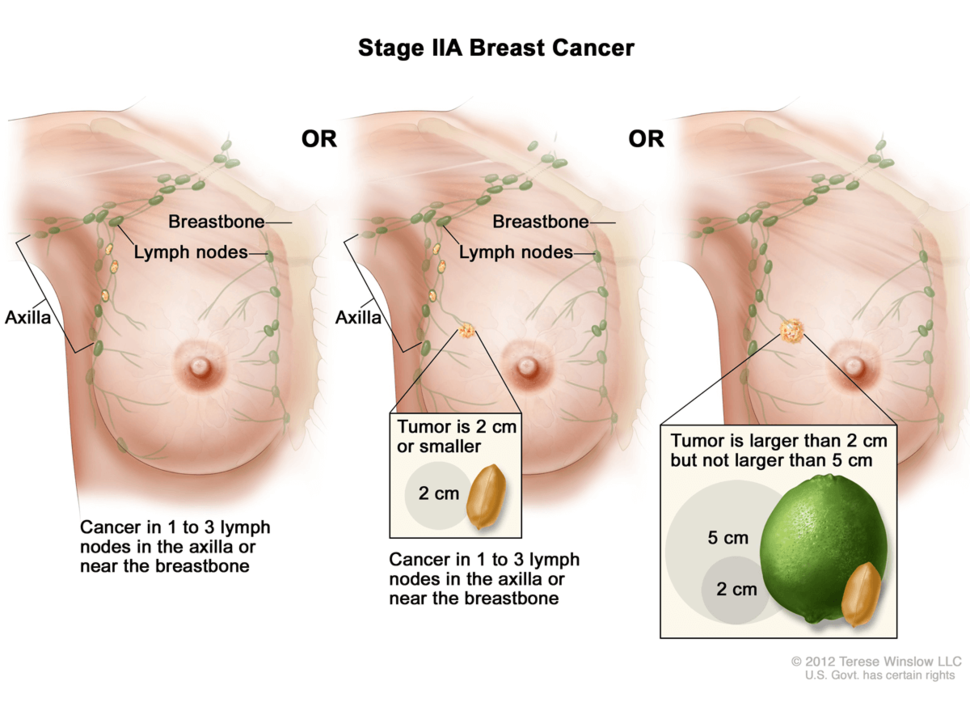
However, she added, "the use of neratinib could be considered in patients with early-stage HER2-positive breast cancer and clinical features that indicate a higher likelihood of relapse," such as larger tumors or cancer cells found in the axillary lymph nodes.
HER2: A Continuous Target
Breast cancers that overexpress the HER2 protein (HER2-positive cancers) tend to be aggressive. The availability of drugs that target HER2—which began with the development of trastuzumab and now includes pertuzumab (Perjeta®), lapatinib (Tykerb®), and trastuzumab emtansine (Kadcyla™)—has significantly improved survival for patients with HER2-positive disease.
Unfortunately, any cancer cells remaining after surgery may develop resistance to the initial HER2-targeted treatment. Neratinib was developed to overcome this resistance by targeting the HER2 signaling pathway in a different way than trastuzumab and other HER2-targeted agents.
In the trial that led to neratinib’s approval, more than 2,800 women who had already completed up to 2 years of adjuvant treatment with trastuzumab were randomly assigned to receive 1 additional year of neratinib or a placebo.
The trial had three different pharmaceutical sponsors over its course, and three large amendments were made to the study design during the trial. In the final design, patients in the two groups were to be compared for disease-free survival at 2 years and for overall survival at 5 years. FDA approval was based on the data from the first 2 years of follow-up.
After 2 years of follow-up, the women in the neratinib group had a 33% reduced risk of a recurrence of their disease: 70 women in the neratinib group experienced a recurrence, compared with 109 women in the placebo group.
In addition to experiencing more diarrhea than women in the placebo group, women receiving neratinib also experienced more nausea and vomiting. Heart problems, which are a concern with HER2-targeted drugs, were rare in both groups.
The researchers plan to continue following the women to evaluate possible differences in 5-year overall survival.
Another Option for Patients with HER2-Positive Disease
Therapies targeting HER2 are a rapidly evolving area of treatment. Currently, many women with higher-risk, early-stage HER2-positive tumors receive both trastuzumab and pertuzumab, beginning either before or after surgery. Whether neratinib would benefit these women could not be answered by the current trial, explained Dr. Zimmer.
“It’s important for patients to realize that FDA approval doesn’t mean the drug is now indicated for every HER2-positive breast cancer patient after one year of trastuzumab treatment,” she said. “It’s another option for therapy that’s available, and patients should carefully discuss it with their doctors, to consider benefit versus side effects in every case.”