The Imperative of Addressing Cancer Drug Costs and Value
, by Barbara K. Rimer, Dr.P.H.
The President's Cancer Panel is an independent panel that was established under the National Cancer Act of 1971. The panel's charge under the law is to identify high-priority issues that are impeding progress against cancer, engage the relevant stakeholders, and develop recommendations for addressing each respective issue. The recommendations are included in a report that is submitted to the President.
Barbara K. Rimer, Dr.P.H., dean of the University of North Carolina's Gillings School of Global Public Health, is the panel's chair.
This week, the President’s Cancer Panel released its latest report to the White House and the public, Promoting Value, Affordability, and Innovation in Cancer Drug Treatment.
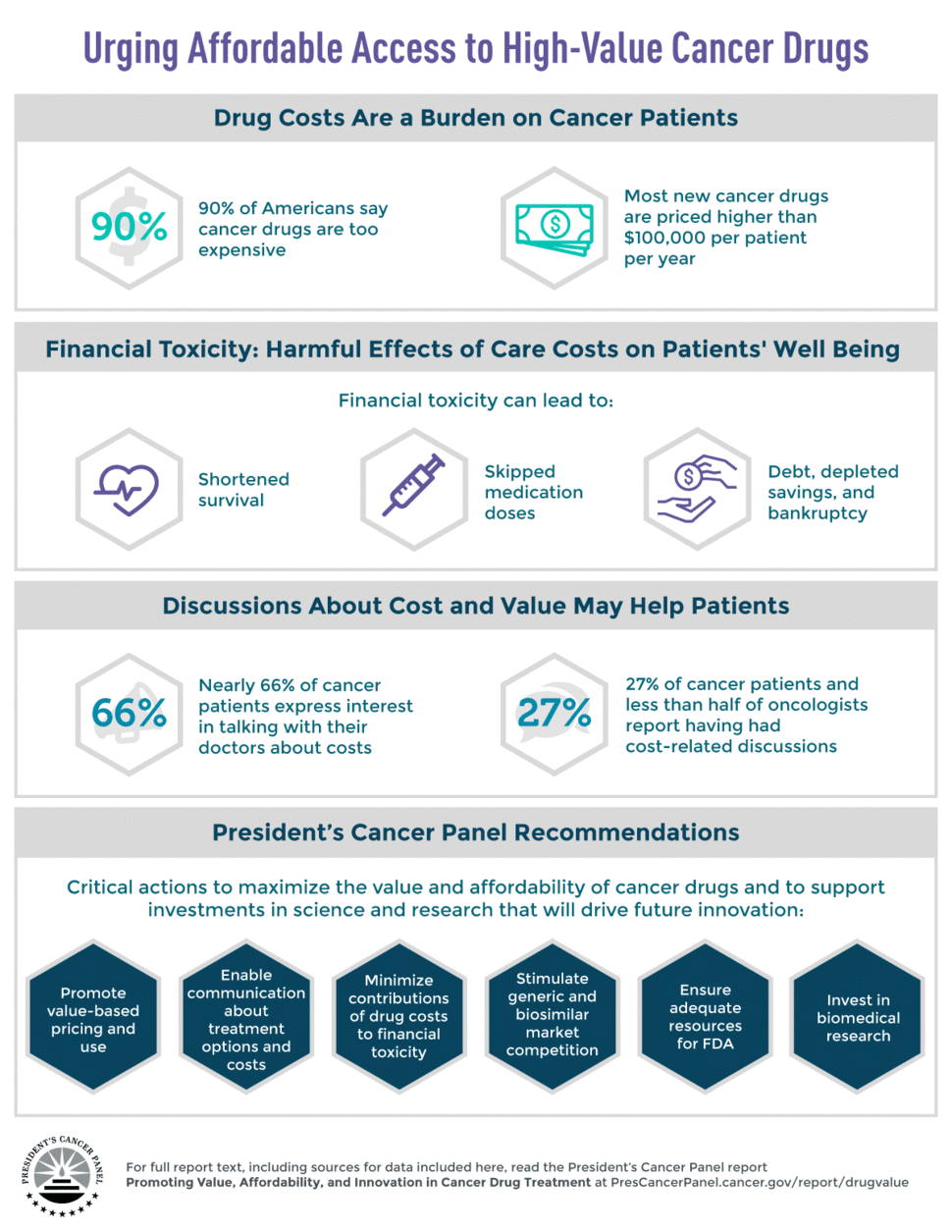
The report recommends six critical actions to maximize the value and affordability of cancer drug treatment and to support investments in science and research that will drive future innovation.
I’ve been member and chair of the panel since 2011. The topic of drug costs and value was, in many ways, the most challenging we have taken on during my tenure.
As a panel, we began discussing the possibility of focusing our next report on cancer drug prices because it seemed that, everywhere we turned, we heard stories—some heartbreaking—about the impact of the rising cost of cancer care and the escalating costs of cancer drugs.
From 1995 to 2014, in fact, there was a sharp increase in the launch price of new cancer drugs—that is, the cost of a new drug being introduced to the market for the first time. Most cancer drugs launched between 2009 and 2014 were priced at more than $100,000 per patient for one year of treatment. More recently, we’ve seen launch prices of more than $400,000 for a year of treatment.
As a consequence of these increasing prices, according to one recent analysis, some patients may face out-of-pocket costs of nearly $12,000 a year for one drug.
On one hand, thanks to investments in research on immunology, genomics, and related areas, some of the new cancer drugs that have reached the clinic are truly transformative for some patients, offering the hope of long-term remissions, if not cures, for previously refractory cancers.
On the other hand, many patients fear that these new drugs will be out of reach given their high price tags.
As the panel considered the topic of drug prices, we recognized that the issues are incredibly complex and there are no simple solutions.
In the end, though, we concluded that these issues were so urgent, so high-stakes, and so consistent with our legislatively mandated task of reporting to the President on the barriers to progress against cancer in the United States that we could not ignore the rising price of cancer drugs.
Patients at the Head of the Stakeholder Table
Although the debate around the cost of cancer drugs can often be contentious and seek to place blame, we were determined to approach this topic without any biases and to bring all of the key stakeholders to the table to help inform our recommendations.
We invited participants to several workshops with specific themes, where we discussed and debated important questions about the cost of cancer drugs and cancer care more broadly.
Participants included patients, health care providers, representatives from academia and government (including NCI, the Food and Drug Administration, and the Centers for Medicare and Medicaid Services), leaders from the pharmaceutical and insurance industries, and others.
They all came to these workshops with their own analyses of the problem and their own proposed solutions.
It was essential that patients be at the table. They brought a range of viewpoints and circumstances, and they all shared stories that were poignant and painful.
Ide Mills introduced herself as a woman who has worn many hats: lung cancer patient, retired pediatric oncology social worker, and caregiver to her mother, whom she lost to lung cancer more than 30 years ago. Ide spoke of the challenges faced by patients who are burdened by financial distress; who routinely have to choose between paying for their medicines or their mortgages; who skip doses of their medications to stretch prescriptions longer, potentially reducing the effectiveness of their treatments.
Andrew Schorr leads an advocacy organization called Patient Power and is on long-term maintenance therapy to manage two different cancers. As Andrew introduced himself, he held up a tiny white pill that carries a price tag of $10,000 a month. He will have to take this medication, along with others, for the rest of his life. He worries, he told us, about the day his doctor tells him he needs to start taking another high-priced drug.
Heather Block, who has worked overseas for the State Department and United Nations helping those in need, said that she worries about potential bankruptcy from treatment costs as much as she worries about her metastatic breast cancer. “[This is] the reality of what it's like to live day to day and to stay in treatment forever,” Heather told us.
Financial Toxicity: Harmful Side Effects of Cancer Treatment
Those stories are just a sampling of many that we heard. The financial distress caused by the cost of cancer care can cause patients to lose their homes or jobs. For patients, it can affect the livelihood of their families and, often, can leave debt as their legacy long after their deaths.
One patient talked about having to leave her job and move to another city temporarily to undergo a bone marrow transplant. Others talked about family members who have had to stop working to care for them or others.
The negative and often profound impact that cancer treatment costs can have on patients and their families and caregivers has come to be called financial toxicity.
During our workshops, it became clear to the panel that the challenges presented by financial toxicity raise serious questions about who we are as a country: Will we be a society that shares the fruits of our scientific enterprise so that all may benefit, or will innovative therapies be available only to those who can pay?
If drug prices continue on their current trajectory, we concluded, then as a country we will be on the path to making decisions about who will live and who will die.
Report Recommendations: Promoting Cancer Drug Value, Affordability, and Innovation
While the panel found no easy solutions, we did arrive at several key recommendations.
First and foremost, we recommend developing ways to better align drug costs with their value to patients. Some cancer drugs are both highly effective and very expensive. Those drugs can be a good value, and they should be available to all patients who can benefit. Some drugs, on the other hand, provide only small benefits—such as extending life by only days or weeks—and, perhaps, with a diminished quality of life. Those drugs are not a good value.
Of course, perspectives on the value of a given treatment can differ. But the panel concluded that addressing drug costs and financial toxicity will require a concerted and coordinated effort to better define drug value. And those conversations should always keep in mind the people most affected by these deliberations: patients.
We also recommend that patients and their families be offered conversations about the potential costs of treatments, including both the direct (e.g., drugs, surgery) and indirect (e.g., managing side effects, travel) costs. The most appropriate individuals to initiate these discussions, however, remain to be determined.
We also conclude that investments in science are critical to support a robust drug pipeline. Biomedical research is the foundation of innovative drug development, and support for regulatory science and infrastructure is essential to ensure that drugs are efficiently and effectively evaluated.
Promoting healthy competition in the generics and biosimilars markets is another key recommendation. Limiting competition can lead to troubling spikes in prices and drug shortages and even cause some manufacturers to leave markets. A functioning generics market is key to providing patients affordable access to needed drugs.
Role for the Cancer Research Community
Many unanswered questions remain regarding the best ways to prevent, detect, and address financial toxicity among individuals with cancer. In our recommendations, we stress the important opportunity for researchers to close these knowledge gaps.
Ann Geiger, Ph.D., M.P.H., of NCI’s Healthcare Delivery Research Program, provided invaluable input as we planned the series of workshops and prepared the report.
Dr. Geiger offered the critical research perspective and highlighted the role that research can play in ensuring that patients have affordable access to high-value drugs.
The panel believes that research is essential to determining how best to equip patients and clinicians with the information and communication skills they need to balance financial considerations with other treatment risks and benefits.
Urgent Action Needed to Ensure Affordable Access to Cancer Drugs
Ide Mills died in April 2017, only months after we met her. Patients like Ide, Andrew, Heather, and countless others don’t have the luxury of time to wait for drugs that could extend their lives at prices they can afford.
With this report, we’ve added a voice to the growing chorus of stakeholders who are deeply concerned that escalating cancer drug prices are straining societal resources, putting clinicians in difficult ethical positions, and risking serious financial distress for patients and their families.
Collaborative efforts to guarantee value in cancer drug treatment, better communication about treatment options and costs, a robust biomedical research enterprise, and a healthy generic drug market will move us closer to the goal of affordable access to high-value cancer drugs for all patients who need them.
Reaching that goal will require us, as a society, to make hard choices.