Studies Highlight Potential of Targeting HIF-2 in Kidney Cancer
, by NCI Staff
Two new studies show that a new class of drugs can block the activity of a molecular driver of the most common type of kidney cancer, clear cell renal cell carcinoma (ccRCC). Both studies were published online September 5 in Nature.
The drugs target HIF-2, a transcription factor that controls the activity of a group of genes, which can promote tumor growth. In both studies, a HIF-2-targeting drug shrank human-derived ccRCC tumors in mice.
And in one of the studies, conducted at the University of Texas (UT) Southwestern Harold C. Simmons Comprehensive Cancer Center, the HIF-2 inhibitor was more effective in the mouse model than sunitinib (Sutent®), a targeted therapy currently approved to treat advanced kidney cancer. In addition to being “more potent than sunitinib, the current standard of care, [the HIF-2 inhibitor] showed activity in tumors that progressed after sunitinib,” said the study’s senior author, James Brugarolas, M.D., Ph.D.
Researchers at UT Southwestern and Dana-Farber Cancer Institute, where the other study was conducted, lead the two NCI Specialized Programs of Research Excellence (SPOREs) for kidney cancer.
The Road to HIF-2α
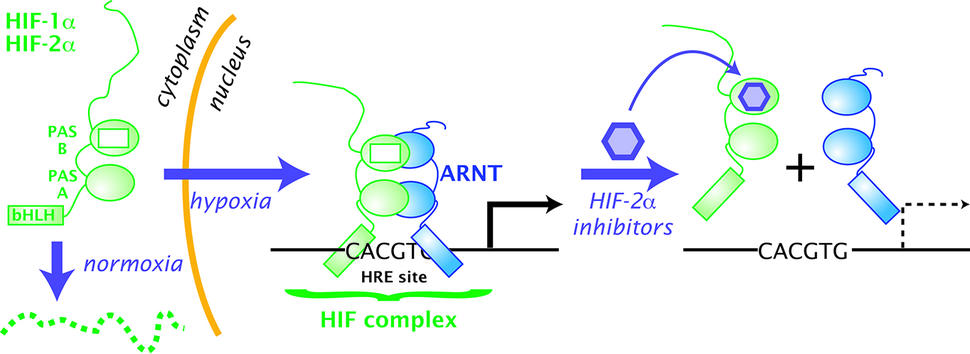
A common event in ccRCC tumor development is increased levels of HIF-2α, one of two proteins that bind together to form the HIF-2 transcription factor. The overactivity of HIF-2 is the result of a mutation in the tumor suppressor gene VHL, explained Marston Linehan, M.D., chief of the Urologic Oncology Branch in NCI’s Center for Cancer Research, who was not involved in either study.
More than 20 years ago, Dr. Linehan and his colleagues at NCI identified the VHL gene and demonstrated its critical role in kidney cancer.
HIF proteins help cells survive in situations where they lack access to enough oxygen, a condition called hypoxia. HIF-2 helps hypoxic cells survive in several ways, including by turning on genes that promote the development of new blood vessels and erythropoietin, which spurs the generation of red blood cells.
Due to their role in ccRCC, HIF proteins have been a long-sought target for researchers. Unfortunately, because proteins like HIF-2 lack the typical features that are needed to be bound by drugs, they have traditionally been considered “undruggable,” Dr. Brugarolas said.
But over the past two decades, Richard Bruick, Ph.D., and Kevin Gardner, Ph.D., of UT Southwestern conducted a series of studies to detail HIF-2α’s structure, identifying a “cavity in the protein that could be exploited” as a potential drug target, Dr. Brugarolas continued. The result of their work was the development of several agents that target this site in HIF-2α. These agents were licensed to Peloton Therapeutics, which is testing one of these drugs, PT2385, in several early-phase clinical trials.
Shrinking Tumors
Both Nature studies involved PT2399, a HIF-2 inhibitor closely related to PT2385. In their study, Dr. Brugarolas and his colleagues tested PT2399 in an advanced type of mouse model, called a patient-derived xenograft, or PDX, which more closely mimics how tumors behave in humans than do other mouse models.
They compared mice that received PT2399 with mice that received sunitinib. The PT2399 treatment led to greater reductions in tumor size than sunitinib, they reported, and also appeared to be less toxic.
In the second study, led by the Dana-Farber SPORE, treatment with PT2399 also shrank tumors in mouse models of metastatic ccRCC, including a PDX model.
Both teams also sought to determine how the drug was exerting its antitumor effects. The UT Southwestern team confirmed that the drug was affecting its intended target, showing, for example, that it caused the two proteins in the HIF-2 complex to come apart. And in experiments involving ccRCC cell lines with an inactive VHL gene, the Dana-Farber-led team showed that treatment with PT2399 disrupted the activation of several genes controlled by HIF-2.
Treatment Resistance, Potential Biomarkers
Both studies also highlighted a problem that has dogged other targeted therapies: treatment resistance.
Resistance to PT2399 occurred even when there was evidence that the drug had hit its target, such as reduced levels of circulating erythropoietin, Dr. Brugarolas and his colleagues reported. And in ccRCC cell lines, the Dana-Farber team found that there was “variable sensitivity” to the drug, even in cell lines known to depend on HIF-2 for survival.
The UT Southwestern investigators, however, identified a potential mechanism that may be responsible for resistance to the HIF-2 inhibitor: mutations in HIF-2α and HIF-1β, the protein with which HIF-2α binds to form HIF-2, that allowed them to remain bound despite treatment with PT2399.
Both teams also identified biomarkers that may identify patients who are likely to respond to the drug. Such biomarkers are an increasingly important element in the development of targeted therapies.
For example, both teams showed that a better response to PT2399 was associated with higher tumor levels of HIF-2α. And senior author William Kaelin, Jr., M.D., of Dana-Farber and his colleagues also reported that ccRCC cell lines with mutations in the TP53 gene—another tumor suppressor often called the “guardian of the genome”—developed resistance to PT2399.
The findings, they wrote, suggest that the use of HIF-2-targeted therapies in patients with ccRCC “will demand predictive biomarkers, perhaps including measures of HIF-2α activity and [TP53] status.”
Identifying potential biomarkers of treatment response and mechanisms of treatment resistance is critical and will help to guide future investigations, Dr. Linehan said. “To me, that’s as exciting and important as the tumor response data,” he said.
“We are learning a huge amount about the role of HIF-2 in clear cell kidney cancer,” Dr. Linehan continued. These and other studies, he stressed, are also allowing researchers to identify potential drugs to test in combination with HIF-2 inhibitors.
Early-Stage Trials
Initial findings from an ongoing phase I trial of PT2385 were presented in June at the American Society of Clinical Oncology (ASCO) annual meeting. Of the 51 patients treated in the trial at that point, one had a complete response to treatment, three had partial responses, and 16 others had stable disease.
In their Nature paper, Dr. Brugarolas and his colleagues provided a brief update on one patient from the trial who had stable disease following treatment with PT2385. The patient, a 47-year-old man who had received seven different therapies—including several targeted therapies—before enrolling in the trial, has continued to live without his cancer progressing for 11 months, they reported.
The patient has tolerated the drug well, with little in the way of side effects. “His quality of life has been better than it was with any of the other molecularly targeted therapies he received,” Dr. Brugarolas said.
Dr. Linehan cautioned against “overinterpreting this result from a single patient in a small clinical trial.” Nevertheless, he continued, the data generated on HIF-2 inhibitors so far “are definitely very exciting.”
Because patients appear to tolerate PT2385 well, “there is an opportunity for combining it with other drugs,” Dr. Brugarolas said. The phase I trial presented at the ASCO meeting, for example, has been expanded to include a group of patients who will receive PT2385 in combination with the immunotherapy drug nivolumab (Opdivo®).