HPV Infections Targeted by Vaccine Decrease in U.S.
, by NCI Staff
Infection with human papillomavirus (HPV) types targeted by the quadrivalent HPV vaccine has declined by nearly two-thirds among teenage girls since HPV vaccination was recommended in the United States, according to new study results. The study also is the first to show a reduction in national prevalence of these four HPV types among U.S. women in their early twenties since the vaccine was introduced.
In the United States, routine vaccination against HPV, which causes virtually all cervical cancers and is transmitted through sexual contact, has been recommended since mid-2006 for 11- to 12-year old girls and for females up to age 26 who have not previously been vaccinated. HPV vaccination has been recommended for males since 2011.
The new study, published in Pediatrics on February 22, used data from U.S. girls and women 14 to 34 years old who participated in NHANES, a national survey that assesses the health of adults and children in the United States.
Declining HPV Prevalence in the Post-Vaccine Era
Through 2014, almost all HPV-vaccinated individuals in the United States received the quadrivalent vaccine (Gardasil®), which protects against infection with HPV types 6, 11, 16, and 18. HPV 16 and 18 are high-risk types that together cause about 70 percent of all cervical cancers as well as a large proportion of anal, oropharyngeal, vaginal, vulvar, and penile cancers. HPV 6 and 11 do not cause cancer but can cause warts on or around the genitals, anus, mouth, or throat.
For the study, researchers led by Lauri Markowitz, M.D., of the Centers for Disease Control and Prevention (CDC), compared HPV prevalence in females of various age groups during 2003-2006, before the vaccine was introduced, with that during 2009-2012, the most recent years for which NHANES results are available.
The analysis showed “a decline in HPV prevalence in the age groups in which we would first expect to see an impact of vaccination,” Dr. Markowitz said.
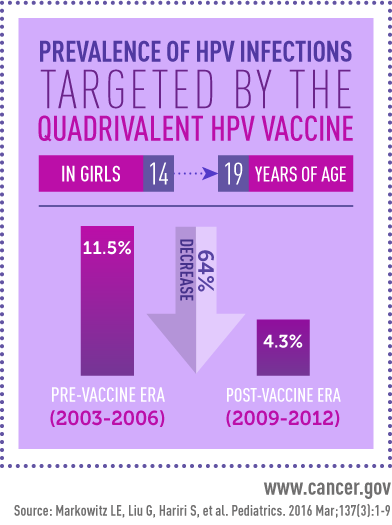
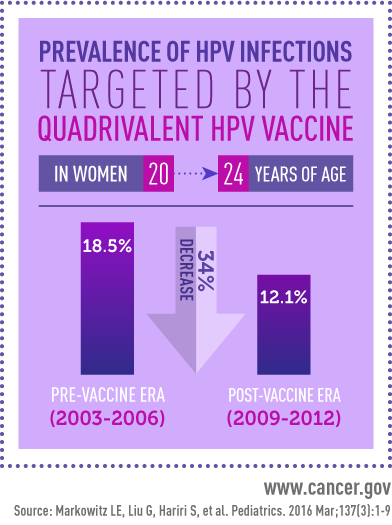
Among girls 14 to 19 years old, the prevalence of the four HPV types targeted by the quadrivalent vaccine dropped from 11.5 percent in the pre-vaccine years to 4.3 percent in the post-vaccine era. In women 20 to 24 years old, the prevalence of HPV infection fell from 18.5 percent to 12.1 percent. By contrast, prevalence of the four HPV types did not change in women aged 25 to 29 or 30 to 34 years. In sexually active females aged 14 to 24 years, prevalence of the four types was 2.1 percent in those who had received one or more doses of the vaccine, versus 16.9 percent in unvaccinated females.
The reduction in HPV prevalence was somewhat higher than expected, given the relatively low proportion of U.S. girls and young women who have received the recommended three-dose series of the vaccine, Dr. Markowitz said. “According to our national surveys, in 2014 about 60 percent of girls aged 13-17 years had received one or more doses and about 40 percent had received all three doses.”
Dr. Markowitz said the higher-than-expected reduction could be due either to protection achieved by fewer than three doses of the vaccine, a possible explanation that is supported by findings of recent studies, or to decreased transmission from people who were vaccinated to unvaccinated individuals, a phenomenon known as herd protection.
Room for Improvement
“While it’s really encouraging that we’ve seen this impact [of the vaccine], our vaccine coverage is not as high as we’d like it to be in the United States,” Dr. Markowitz said. “If we could get that coverage higher we could have a larger impact” toward the ultimate goal of preventing cervical cancers and other HPV-caused cancers in women and men.
NCI is working with the CDC and other government and nongovernment organizations to increase HPV immunization rates in the United States. In addition to “funding cancer researchers to develop interventions to promote the vaccine and to understand…the barriers to immunization, we’re also collaborating with a wide group of stakeholders interested in promoting the vaccine,” said Sarah Kobrin, Ph.D., M.P.H., of the Health Systems and Interventions Research Branch in NCI’s Division of Cancer Control and Population Sciences (DCCPS).
“We are also working to ensure that the research is influencing practice,” said Cynthia Vinson, Ph.D., of the DCCPS Implementation Science Team. With encouraging results such as those of the new CDC study, “we can continue to argue with confidence that vaccination is [eventually] going to reduce cervical cancer and other HPV-associated cancers,” added Dr. Kobrin.