Study Uncovers Previously Unrecognized Effect of Chemotherapy
, by NCI Staff
A new study conducted primarily in mice suggests that chemotherapy given before surgery for breast cancer can cause changes in cells in and around the tumor that are tied to an increased risk of the cancer spreading to other areas of the body. However, the study also identifies an experimental therapy that could potentially reduce this risk.
Working with mouse models of breast cancer, researchers showed that several chemotherapy drugs commonly used to treat localized and advanced breast cancer increased the number of microscopic structures in breast tumors called tumor microenvironment of metastasis (TMEM), as well as the number of tumor cells circulating in the blood.
TMEM act as portals that help invasive cancer cells escape from a tumor and move into the circulation—a key step in cancer metastasis.
The new findings were published July 5 in Science Translational Medicine.
The findings are intriguing and could ultimately be important to patients, said Kent Hunter, Ph.D., and Stanley Lipkowitz, M.D., Ph.D., of NCI’s Center for Cancer Research (CCR), who were not involved in the study. But they cautioned that further studies will be needed to demonstrate a tighter connection between chemotherapy-related changes in TMEM and patient outcomes.
Some news reports of the findings have raised concern among patients and patient advocates. But Dr. Lipkowitz, who heads the Women’s Malignancies Branch in CCR, emphasized that “many clinical studies have compared chemotherapy given before or after surgery and have found no evidence that patients who get neoadjuvant therapy have worse outcomes.”
Maja Oktay, M.D., Ph.D., of Albert Einstein College of Medicine and Montefiore Health System in New York, one of the senior authors on the study, agreed that more research is needed to learn how to apply the findings to patient care and emphasized the important role that chemotherapy plays in the treatment of breast cancer.
“Overwhelming evidence shows that chemotherapy is potentially curative for patients with localized breast cancer and prolongs life in patients with metastatic disease,” Dr. Oktay said.
Prime Suspects in Promoting Metastasis
Death from breast cancer is mainly due to distant metastasis, when cancer cells from the primary tumor form tumors elsewhere in the body.
Previous research by the Einstein team, led by the other senior author of the new study, John Condeelis, Ph.D., has provided insights into how breast cancer spreads, including the role of TMEMs.
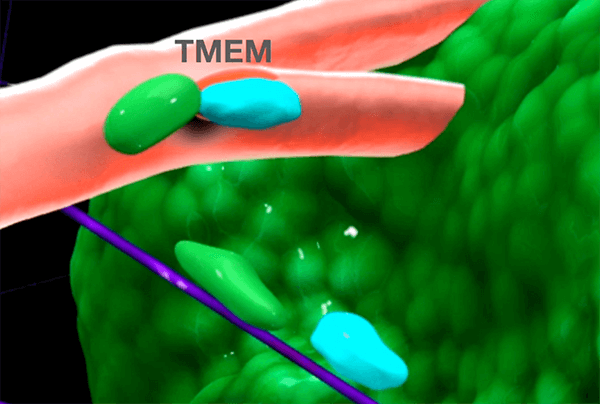
Each TMEM is made up of three different types of cells that are in close contact with each other on a blood vessel wall: an endothelial cell (a type of cell that lines blood vessels); an immune cell called a macrophage; and a tumor cell that produces high levels of a specific form of Mena, a protein that enhances the tumor cell’s ability to invade blood vessels and spread.
A 2015 study led by Dr. Condeelis monitored TMEM in living mice in real time. It showed that the macrophages in a TMEM loosen the normally tight connection that exists between endothelial cells, creating a temporary opening in the wall of a blood vessel for the tumor cell to squeeze through and enter the bloodstream, facilitating its spread to other parts of the body.
In several other studies, the Einstein researchers and their colleagues showed a correlation between the number of TMEM sites in patient tumor samples and an increased risk of metastasis in estrogen receptor (ER)–positive, HER2-negative breast cancer, which is the most common type of breast cancer.
Some studies in animal models, the researchers wrote, have shown that the chemotherapy drug paclitaxel (Taxol) causes tissue damage that, in turn, induces an inflammatory response resulting in an increase in the density of two TMEM components: certain specialized macrophages and endothelial cell precursors.
Given the findings from these studies, the researchers decided to investigate whether chemotherapy increases TMEM formation in breast tumors.
Chemotherapy-Induced Changes in TMEM
For the new study, the researchers worked with four different mouse models of breast cancer in experiments led by the first author, George Karagiannis, D.V.M., Ph.D. The models were developed to mimic the clinical scenario in which chemotherapy is given before surgery to patients with locally advanced disease to shrink the primary tumor and kill cancer cells that have spread to nearby lymph nodes and beyond.
The researchers found that the tumors of mice treated with paclitaxel had two to three times more TMEM than those of mice that did not receive the drug. Paclitaxel also increased TMEM activity in two mouse models as compared with untreated mice.
Increased TMEM activity in breast tumors was indicated by a greater density of macrophages found in the TMEM, an increase in the permeability of blood vessels in the tumors, and increased expression of several forms of Mena protein that are seen in invasive cancer cells.
In addition, paclitaxel treatment roughly doubled the number of tumor cells in the circulation—a marker of TMEM function and metastasis—and increased micrometastasis in the lungs of treated versus untreated mice.
Paclitaxel was not alone in promoting TMEM formation, Dr. Oktay and her colleagues reported. Mice treated with two other chemotherapy drugs commonly given to patients before breast cancer surgery, doxorubicin, and cyclophosphamide, also had more TMEM sites, increased TMEM activity, and more circulating tumor cells compared with untreated mice.
The researchers then compared biopsy specimens previously collected from 20 women with ER-positive breast cancer before and after treatment with a neoadjuvant regimen of paclitaxel, doxorubicin, and cyclophosphamide.
They found that most patients showed some increase in the number of TMEM sites after neoadjuvant chemotherapy, five had more than a fivefold increase in TMEM, and none showed a decrease in TMEM numbers after chemotherapy.
“The clinical relevance of this finding still needs to be determined,” Dr. Oktay said.
Counteracting the Effects of Chemotherapy
Finally, the research team investigated whether an experimental drug called rebastinib could counteract the effects of paclitaxel on TMEM activity. Rebastinib targets a receptor called TIE2 on the surface of the specific type of macrophage found in TMEM. In two different mouse models, the team found that rebastinib blocked paclitaxel-induced increases in both the blood vessel permeability and cancer-cell spread associated with TMEM activity.
If confirmed in human studies, the rebastinib findings suggest that “there may be modifications of current neoadjuvant therapy that could improve outcomes [for some patients], and that this may be achieved by blocking the activity of these TMEM structures,” Dr. Hunter said.
As a first step, Joseph Sparano, M.D., a coauthor of the study and his colleagues at Einstein and Montefiore Medical Center are now enrolling patients with metastatic, HER2-negative breast cancer in an early-phase clinical trial that will test the safety of combining rebastinib with paclitaxel or eribulin (Halaven®), a drug with actions similar to paclitaxel.
After completion of that trial, the team plans to initiate randomized trials to test the effectiveness of rebastinib given with chemotherapy before surgery in patients with locally advanced and metastatic disease, and to study the effects of rebastinib treatment on TMEM function.
More work will be needed to determine whether changes in TMEM identify a subset of patients with early-stage breast cancer who do worse on preoperative chemotherapy, and to test whether drugs that target TMEM sites can improve long-term outcomes in these patients, Dr. Lipkowitz said.
Demonstrating that the addition of a drug that inhibits TMEM formation or function to neoadjuvant chemotherapy improves patient outcomes will require a large randomized prospective trial with many years of follow-up. But analogous studies in mouse models, where researchers follow the animals for recurrence or death due to metastasis, could provide important information in the short term, Dr. Lipkowitz said.
“Overall, our findings have uncovered a previously unrecognized effect of chemotherapy, and a potential strategy for reversing it,” Dr. Sparano said.
Ultimately, Dr. Oktay said, “Our findings in this study and our other work could lead to testing of new prognostic and predictive markers, including TMEM density, to identify patients at risk of cancer recurrence. This work may also lead to an entirely new treatment approach for preventing metastasis, the primary cause of death in breast cancer.”